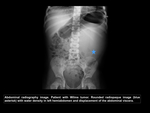
Wilms tumor is usually a solitary lesion in a kidney and there is usually no metastasis at the time of diagnosis,
although throughout the disease can develop lung metastases,
liver and rarely in bone and brain.
Occasionally the tumor extends intravascularly to the renal vein and inferior vena cava (ICV).
Below we present the less frequent presentations of Wilms tumor,
showing the most representative images in each case.
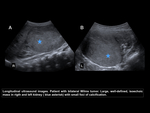
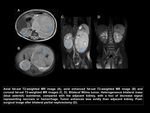
Bilateral Wilms tumor.
Usually,
Wilms tumor is a single lesion in a single kidney.
They are large lesions due to the insidious growth of the lesion and can cross the midline.
However,
up to 6-10% of cases can be bilateral.
The contralateral kidney needs to be carefully screened.
The presence of a synchronous lesion changes the stage to stage V,
and this will change the therapeutic approach.
The staging of the bilateral tumor must be done independently for each kidney,
and the prognosis depends on the higher individual stage.
The unilateral Wilms tumor is usually treated with nephrectomy followed by adjuvant chemotherapy.
In bilateral tumor,
preoperative chemotherapy is important,
since the current approach is resection of the tumor with preservation of the normal parenchyma.
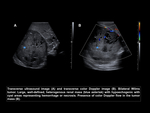
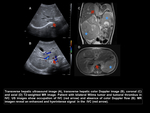
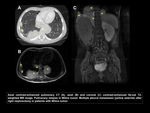
Intravascular thrombus
It has been reported that intravascular thrombus occurs in 20 to 35% of Wilms Tumor,
while IVC involvement is reported in only 4 to 10%.
A thrombus that reaches the atrium occurs in less than 1% of all patients.
Children with WT and a thrombus in their IVC are usually asymptomatic.
This is probably due to the persistence of venous blood flow despite the presence of a tumor thrombus within the lumen of the cava.
When the thrombus is below the hepatic veins,
management options include initial surgery or neoadjuvant chemotherapy followed by delayed surgery.
With greater extension of the proximal thrombus and in stable patients,
neo-adjuvant chemotherapy has gained consensus as the primary approach of choice regardless of the protocol adopted.
In those cases in which there is thrombus in the IVC and right atrium,
in which surgery is decided as the first option,
cardiopulmonary bypass for removal is required.
Adherent ICV thrombus has been treated by different surgical procedures.
Anticoagulation is not indicated routinely.
The presence of thrombus tumor represents a major surgical risk.
The preoperative identification,
the determination of extension and the possible invasion of the IVC wall are crucial factors in the planning of the therapy.
It must be identified for decreases the rate of surgery complications.
Therefore,
the presence of thrombus in the ICV is not a prognostic factor,
not decrease survival rate,
however the patient's morbidity increases due to the risk of pulmonary thrombosis.
It is crucial to identify thrombus in imaging studies because changes the therapeutic plan.
Not identifying the intravascular thrombus in pre-surgical studies increases complications during surgery.
The technique of choice for the detection of thrombus is the US with color Doppler because it sometimes goes unnoticed in CT studies.
MR is also an ideal technique for the identification of the thrombus and its extension.
The performance of presurgical echocardiography is important to detect the presence of thrombus in the right atrium.
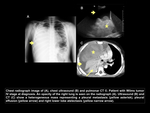
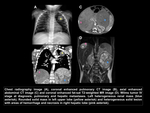
Metastatic lung disease
The lung is the most common site of metastatic disease in Wilms Tumor (85% of cases of metastatic disease).
10% of patients have pulmonary metastases at diagnosis.
The 5-year survival rate decreases to 20% -70%.
The traditional diagnostic method to detect metastatic disease in the lung in children with Wilms tumor is chest radiography.
The use of chest radiography versus CT for evaluation for lung metastasis at diagnosis remains controversial.
The results obtained from the most of studies are based on the use of radiography.
However,
CT is more sensitive for small nodules.
There are studies that shown no substantial differences in the outcome after the administration of local therapy of those who were treated as a metastatic disease in those patients with pulmonary metastases only visible by CT.
However,
CT is essential for those with unfavorable histology or stage III.
Relapse
Approximately 15% of primary tumors with favorable histology and 50% of cases of high-risk tumors develop relapse.
Approximately 95% of tumor recurrences occur within 2 years of the initial diagnosis.
The long-delayed recurrence,
> 5 years after diagnosis,
is very infrequent,
only 0.5% of cases.
The most frequent relapse sites are the lung,
abdomen and less frequently bone and brain.
Recurrent tumors are defined as very high risk to develop a chemoresistant disease,
which correlates with a poor prognosis.
In response to a series of items,
patients with Tumor Wilms were classified into 3 risk categories for recurrence:
- Standard risk (30% of cases of recurrence): patients with favorable-histology WT with relapse after therapy with only vincristine and/or actinomycin D.
Free survival range 70-80% range.
- Highrisk (45-50% relapse): with favorable-histology WT with relapse after therapy with three or more agents.
Free survival range 40-50%.
- Very-high-risk (10-15% relapse): patients with recurrent anaplastic or blastemal-predominant WT.
Free survival range 10%.
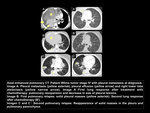
Pulmonary relapse
The most Wilms tumors recurrences occur in the lung,
58% of cases.
The sites of pulmonary relapse included in the lung parenchyma,
pleura,
and less frequent mediastinum.
The 3-year survival rate decreases to 45% in those patients with Wilms tumor with relapse confined to the lung.
The chest X-ray is,
until now,
the test of choice for the detection of lung disease.
CT helps identify a subset of patients with local disease who have an increased risk of relapse of the lung.
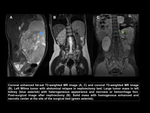
Abdominal relapse
Abdominal relapse is uncommon.
The incidence of local recurrence is widely reported in the literature and it varies from 7-20%.
This rate drops to about 3% in small tumors.
While Tumor Wilms is generally favorable in patients with abdominal relapse carries a worse prognosis.
Decreasing the 3-year survival rate to 28-30%.
The most frequent sites of abdominal relapse included the kidney,
peritoneum and lymph nodes.
Relapse in the surgical bed is uncommon,
being the less frequent site of relapse in the published articles.
The patients with highest risk of abdominal relapse are those with unfavorable histology,
nephroblastomatosis,
spillage tumor,
the inflammatory pseudocapsule and tumors > 4cm.
It's recommended to closely follow-up with imaging studies of high-risk patients.
Ultrasound is sufficient for routine monitoring.
It is suggested that high-risk patients be examined every 3 months during the first 3 years.
The CT and MR should be used for uncertain findings.
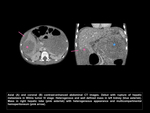
Multifocal disease
It's estimated that the risk of multifocal Wilms tumor is as high as 15%,
but it is much lower among patients with smaller and lower stage tumors.
Patients with nephroblastomatosis have a high risk for the development of multifocal cancer.
These patients should be monitored closely during the first 3-years after diagnosis due to high risk of recurrence.