Generally,
high signal intensity and loss of the intranuclear cleft on T2WI are reliable findings of spondylodiscitis,
but it is difficult to detect them in the early stage.
Some noninfectious diseases (Modic type I endplate change,
acute Schmorl node,
seronegative spondyloartropathies,
Charcot arthropathy,
tumoral and posttraumatic pathologies) may present with a similar radiological pattern.
The following is a list of typical spondylodiscitis findings and some non-infectious pathologies that mimic spinal infections studied in our center.
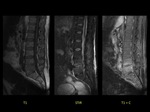
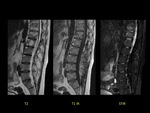
Case 1 (Fig 1)
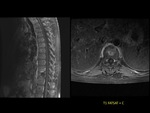
A 52-year-old patient with methicilin-sensitive staphylococcus aureus bacteriemia (MSSA) developing back pain.
MRI showed increased signal intensity in sagittal STIR sequence in the L4-L5 disk.
Sagittal T1-weighted contrast-enhanced fat-suppressed MR image showed enhancement of L5-S1 vertebral endplates related to inflamatory edema and also inflamatory changes in anterior epidural space.
The diagnosis was acute infectious spondylodiscitis.
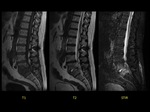
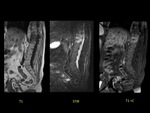
Case 2 (Fig 2,
3)
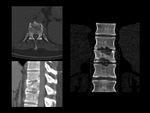
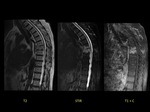
A 79-year-old man with chronic back pain that was not improving after correct treatment.
MRI showed increased signal intensity in sagital T2-weighted and STIR sequences in the L5-S1 disc.
Sagittal T1-weighted MR image showed decreased signal intensity and STIR hyperintensity of the subchondral bone marrow adjacent to the L5-S1 intervertebral disk.
Fat-suppressed,
contrast-enhanced sagittal T1-weighted imaging showed marked paraspinal and anterior phlegmonous epidural enhancement.
The diagnosis was acute infectious spondylodiscitis.
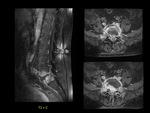
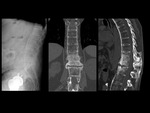
Case 3 (Fig 4,
5,
6)
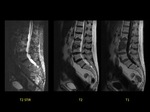
A 43-year-old man with history of Non-Hodgkin´s lymphoma started with fever and low back pain.
MRI showed diffuse low signal intensity of bone marrow in different sequences related to lymphoma infiltration.
We also observed structural alterations and abnormal signal intensity of D11 vertebral body,
with cystic lesion in the anterior margin.
Fat-suppressed,
contrast-enhanced sagittal T1-weighted imaging showed enhancement related to edema.
In addition,
CT scan confirmed osseus lesion with involvement of adjacent vertebral endplates.
The patient underwent bone biopsy and was diagnosed with non-Hodgkin´s lymphoma of the spine.
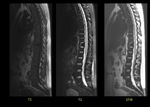
Case 4 (Fig 7)
A 77-year-old patient with stage IV renal cell carcinoma and history of low back pain.
MRI showed abnormally increased signal intensity in sagittal STIR sequence in the D7 vertebral body and pedicles,
affecting also the inferior endplate of the D6.
The disk height was markedly reduced and there was a contrast enhancement of pre and paravertebral soft tissue and little occupation of anterior epidural space.
The radiological diagnosis was spondylodiscitis or metastasis.
The patient underwent bone biopsy and was diagnosed with metastasis of renal cell carcinoma.
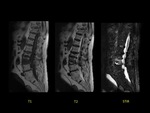
Case 5 (Fig 8)
A 73-year-old female with history of low back pain during the past 3 months despite conservative management.
MRI showed loss of height with compression and irregularity in the superior endplate of L4 with bone marrow edema.
The vertebral body height of L3 was preserved,
nevertheless,
showed the development of bone marrow edema.
The diagnosis was osteoporotic acute vertebral compression fractures.
Case 6 (Fig 9)
A 39-year-old man with history of loss of sphincter control.
MRI showed the loss of normal concavity of the vertebral body (square-shaped vertebral body) with marrow signal intensity changes in anterosuperior and anteroinferior parts of the vertebral endplates of D12,
L1-L2 and L3.
MRI demostrated high signal intensity on T1- and T2-weighted images,
related to Romanus lesion.
In addition,
MRI showed hyperintense signal of D10-11 and D11-12 disk in T2 and STIR sequences with bone marrow edema in adjacent vertebral endplates.
The diagnosis was Andersson lesion in ankylosing spondylitis.
Case 7 (Fig 10,
11)
A 60-year-old patient presented with low back pain and history of ankylosing spondylitis and "bamboo spine" with fusion of D11-12 vertebral bodies.
MRI showed abnormally increased signal intensity in sagittal STIR sequence in D11,
D12 and L1 vertebral bodies and hyperintensity in the D12-L1 disk.
In addition,
CT scan revealed sclerosis in D11-D12 and L1 vertebral bodies and destruction of D11-D12 disk.
The patient underwent bone biopsy and was diagnosed with aseptic spondylodiscitis and vertebral pseudoarthrosis.
Case 8
A 77-year-old patient presented with lumbar radiculopathy with left L4 radicular pattern.
MRI showed an inferior L3 endplate fracture and band-like pattern subchondral edema and fluid sign,
accompanied by pre and paravertebral edema.
In addition,
chronic vertebral compression fracture of L2 was demostrated.
The diagnosis was acute osteoporotic vertebral fracture of L3 and traumatic discitis.