CT characteristic features of CHRONIC PULMONARY THROMBOEMBOLISM can be classified in:
VASCULAR SIGNS: include
- direct pulmonary artery signs (result in thrombus organization)
- signs due to pulmonary hypertension (result of the sustained increase in pulmonary vascular resistance)
- signs due to systemic collateral supply (results of decrease pulmonary artery flow)
PARENQUIMAL SIGNS:
-Scars,
a mosaic perfusion pattern,
focal ground glass opacities,
air trapping and bronchial dilatation.
VASCULAR SIGNS:
- DIRECT PULMONARY ARTERY SIGNS:
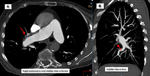
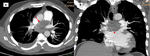
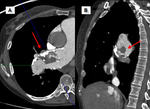
Complete oclussion: abrupt decrease in vessel diameter and absence of contrast material in the vessel segment distal to the total obstruction.
The reduction in vessel diameter is persistent and is caused by the contraction of the trombus.(Fig 1AyB)
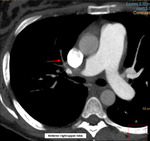
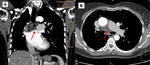
Partial filling defects: an organized thrombus may cause vessel intimal irregularities (Fig 1A), narrowing (Fig 2),
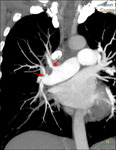
bands (Fig 3)and webs.
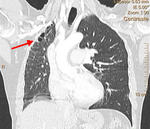
- SIGNS DUE TO PULMONARY HYPERTENSION:
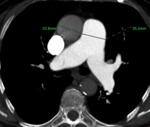
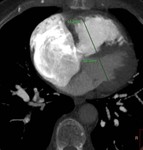
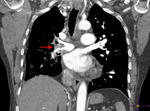
Enlargement of the main pulmonary artery: to a diameter of more than 29 mm may occur in presence of pulmonary hypertension,
regardless the cause.
The CT diameter of the main pulmonary artery is measured on scanning plane of its bifurcation,
at a right angle to its long axis and just lateral to the ascending aorta (Fig 4).
When the ratio of the diameter of the main pulmonary artery to the diameter of the aorta measured on CT scan is greater than 1:1,
there is a strong correlation with elevated pulmonary artery preassure,
specially in patients younger than 50 years.
Central pulmonary arteries in patients with CTEPH often are assymetric in size.
Rigth ventricular enlargement an hypertrophy: the increase workload borne by the right heart results in right ventricular enlargement (dilatation of the right ventricle is considered present when the ratio of the diameter of the right ventricle to that of the left ventricle is greater than 1:1).
There is bowing of the interventricular septum toward the left ventricle (Fig 5) and hypertrophy (right ventricle myocardial thickness greater than 4 mm)
Others: tricuspid valve regurgitation,
mild pericardial thickening or small pericardial effusion and enlarged lymph nodes
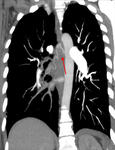
- SIGNS DUE TO SYSTEMIC COLLATERAL SUPPLY:
Bronchial artery hypervascularization: abnormal dilatation of the proximal portion of the bronchial arteries (diameter more than 2 mm) and arterial tortuosity (Fig 6).
Bronchial flow may represent almost
30 % of the systemic blood flow (normal bronchial artery blood flow is of the order of 1-2% of the cardiac output) It is a nonspecific response to stimuli such as reduced pulmonary artery flow,
hypoxemia,fibrosis,
etc.
PARENQUIMAL SIGNS:
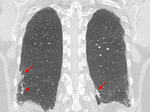
Scars: from prior pulmonary infarctions are commonly depict in areas of decrease of attenuation and may appear as parenchymal bands,
wedge-shape opacities,
peripheral nodules,
cavities or irregular peripheral linear opacities.
They often occur in multiples,
generally are found in lower lobes (Fig 7) and often accompanied by pleural thickening.
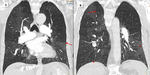
Mosaic pattern of perfusion: (Fig 8).
Is non specific and is seen more often in patients with pulmonary hypertension due to vascular disease,
and much more commonly in patients with CTEPH.
Others:
Air trapping, cylindrical bronchial airway dilatation at the level of segmental and subsegmental bronchi adjacent to severely stenosed or completely obsructed and retracted pulmonary arteries.
Both congenital and acquired conditions may cause pulmonary hypertension or obstruction of the pulmonary arteries and mimic CTEPH.
They are: pulmonary artery sarcoma,
fibrosing mediastinitis,
Takayasu arteritis,
in situ thrombosis associated with idiopathic pulmonary arterial hypertension and proximal interruption of pulmonary artery.
These conditions and radiologic features are reviewed.
PRIMARY SARCOMA OF THE PULMONARY ARTERY:
Is rare.
Only approximatly two hundred cases have been reported in the literature.
Undifferentiated sarcomas and leiomyosarcomas are the types of sarcoma that most frequently affect the pulmonary arteries.
It can be confused with CTEPH due to the similarity of signs and symptoms,
as well as the progresion to pulmonary hypertension,
however weight loss,
fever and digital clubbing should lead to the suspicious of sarcoma.
The main or proximal pulmonary arteries are most frequently involved.
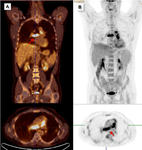
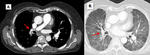
CT scans show the tumor as an intraluminal filling defect that resembles thromboembolus (Fig 9)
The image findings that may be helpful for distinguishing a pulmonary artery sarcoma from CTEPH are:
| PRIMARY SARCOMA OF THE PULMONARY ARTERY |
CHRONIC TROMBOEMBOLIC PULMONAY HYPERTENSION |
| Filling defect may distend main or proximal pulmonary arteries,
usually unilateral |
Filling defect associated with decrease arterial lumen diameter |
| Possible extension of the lesion into lung parenchyma o mediastinum |
Filling defect remain intraluminal |
| Delayed enhancement at CT angiography and magnetic resonance imaging |
No delay enhancement |
| Avidly positive uptake of fluorine 18 fluorodeosyglucose(18-FDG) at positron emission tomography integrated with CT (PET) (Fig 10) |
No uptake 18-FDG (PET) |
FIBROSING MEDIASTINITIS:
Fibrosing mediastinitis is a rare condition that results from a fibrotic reaction cause by granulomatous infection that causes narrowing of (extrinsic compression) the pulmonary arteries and veins (fig 11).
It is characterised by progressive proliferation of dense fibrous tissue within the mediastinum.
There are two types:
-focal: localised calcified mass in the mediastinal paratracheal/subcarinal regions of the pulmonary hila.
There is a previous history of histoplasmosis or tuberculosis.
-difuse: diffusely infiltrative non-calcified mass that affects multiple mediastinal compartments.
There is association with autoinmmune disorders,
retroperitoneal fibrosis,
sclerosing thyroiditis and certain drugs.
-Other appearences: unilateral or asymmetric narrowing or cut-off of the arteries (fig 12).
Ipsilateral Kerley B lines and peripheral wedge-shaped consolidation may occur in arterial or venous infarction.
TAKAYASU ARTERITIS:
The exact incidence of pulmonary arterial involvement varies between 50 an 80% and is often a late manifestation of the disease.
The most characteristisc findings are stenosis or occlusion ,
mainly segmental and subsegmental arteries (fig13 A) and less commonly the lobar or main pulmonar arteries.
CT manifestations include:
-early phase: wall thickening and enhancement due to inflammation.
-chronic phase: dystrophic mural calcification and luminal narrowing (stenosis or occlusion).
Findings of wall thickening in the aorta and aortic branches (sistemic vessel involvement) (Fig 13 B),
collateral formation in vessel not supplying the lung parenchyma and the absence of intraluminal trombi in the pulmonary arteries are diagnostic clues.
Unilateral oclussion of pulmonary artery can occur in advanced cases and late-phase Takayasu arteritis and should be considered in cases of chronic pulmonary artery obstruction of unknown origin.
IN SITU THROMBOSIS ASSOCIATED WITH IDIOPATHIC PULMONARY ARTERIAL HYPERTENSION:
In situ pulmonary artery thrombosis in patients with idiopathic pulmonary hypertension may mimic pulmonary artery occlusions caused by thrombotic material of embolic origin.
It can be distinguished from CTEPH:
| IN SITU THROMBOSIS ASSOCIATED PH |
CHRONIC THROMBOEMBOLIC PULMONARY HYPERTENSION |
|
In situ pulmonary artery thrombosis with patent lumen beyond intraarterial filling defect
(tipically central and non-occlusive)(fig 14)
|
Arteries beyond filling defects either occluded and decreased in diameter or distal beading and intra-arterial webs |
| Dilatation of bronchial arteries uncommon (14% cases) |
Dilatation of bronchial arteries in majority(73% cases) |
| Mosaic attenuation pattern rare |
Mosaic attenuation and regional variation in size of vessel common |
| Peripheral opacities tipically produced by infarctions are rare |
Peripheral opacities tipically produced by infarctions are common. |
| V/Q Scintigraphy: may be normal or may demostrated a mottled appearence characterized by sub-segmental defects.
(fig 15) |
V/Q Scintigraphy: includes >1 segmental or larger mismatched perfusion defects. |
PROXIMAL INTERRUPTION OF THE PULMONARY ARTERY:
Proximal interruption of left pulmonary artery: usually associated with a congenital cardiovascular anomaly,
most commonly tetrallogy of Fallot.
Proximal interruption of right pulmonary artery: is more common and is an isolated finding in most instances.
The pulmonary artery ends blindly at the hilium (Fig 16) and blood supplied through collateral systemic vessels,
mainly bronquial arteries.
Diagnostic clue: smooth,
abrupt tapering of the pulmonary artery,
without endoluminal changes.
In CTEPH a helpful diagnostic key is the presence of multiple BILATERAL arterial abnormalities.
Occlusion of one main pulmonary artery,
mimicking proximal interruption has been report in only 3%of cases.
Another fingings: There is volume loss in the affected segment (Fig 17) with blood supply to the lung parenchyma via systemic collaterals.