Results and discussion:
All posterior fossa cystic lesions observed in our pediatric patients can by divided into congenital and acquired abnormalities.
Congenital cystic lesions include: arachnoid cyst (16 cases),
Dandy-Walker malformation (2 cases) and Dandy Walker variants (8 cases),
mega cisterna magna (46 cases),
Blake's pouch cyst (7 cases) and Joubert syndrome (2 cases).
Acquired cystic lesions include both neoplasm associated cysts - pilocytic astrocytoma (8 cases),
medulloblastoma with cystic foci (2 cases),
as well as other,
mainly iatrogenic causes - infectious/postinfectious and postoperative changes (4 cases).
Congenital cystic lesions:
* Arachnoid cysts (ACs) (Fig.1): Arachnoid cysts are the most common of all congenital intracranial cysts.
The symptoms are rather rare and dependent on size and location in reference to the ventricular system.
They account for approximately 1% of all space-occupying intracranial lesions and are identified in 1-2% of patients.
They can be seen at any age but nearly 75% is found in children and young adults [1-2].
Most of them are located supratentorially,
although 10-15% of ACs are found in the posterior fossa,
especially in the cerebellopontine angle cistern or in the retrocerebellar region [1-2].
They are mainly solitary findings that vary in size - ranging from small incidental findings to large cysts.
Arachnoid cysts are well-marginated with no internal septations and contain clear fluid.
Most incidentally discovered ACs are stable findings.
Enlargement is strongly associated with younger age – under 4 years [1-2].
Uncomplicated ACs behave like cerebro-spinal fluid on CT and MR.
In children MRI plays an important role in the precise localisation and determination of its relationship to the ventricular system.
FLAIR,
DWI and 3D heavily T2-weighted sequences (CISS,
FIESTA,
DRIVE) are the best sequences to visualize these well-marginated cysts filled with cerebro-spinal fluid.
They cause moderate focal mass effect only displacing the brain and do not enhance after contrast administration [1-2].
* Dandy–Walker continuum: The Dandy-Walker continuum (DWC) is a spectrum of congenital cerebellar malformations that may present as cystic structures or cystic-like regions in the posterior fossa.
The continuum includes Dandy-Walker Malformation (DWM),
Dandy-Walker Variants including Vermian Hypoplasia,
Blake’s Pouch Cyst (BPC),
and Mega Cisterna Magna (MCM).
The whole group covers the majority of congenital cerebellar malformation,
where the most common is DWM with an estimated prevalence of 1:5.000 live births.
The group may be isolated or may occur as part of chromosomal anomalies.
The symptoms may be present,
mainly in DWM due to increased intracranial pressure secondary to hydrocephalus.
Despite the extensive cerebellar abnormalities,
cerebellar signs are relatively uncommon.
Early death is common in classic DWM [1-2].
In children MRI plays a pivotal role,
especially in the precise characterization and determination of its relationship to the adjacent structures and no radiation exposure.
CT and transfontanellar ultrasound do not deliver sufficient information.
The fetal ultrasound as well as transfontanellar ultrasound may play only a screening role.
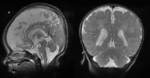
- Dandy-Walker malformation (Fig.2) is a generalized disorder that consists of a large posterior fossa with a high-inserting venous sinus confluence,
large posterior fossa cyst extending dorsally from the fourth ventricle,
representing its dilatation,
and varying degrees of vermian and cerebellar hemispheric hypoplasia as well as vermian superior rotation.
The fourth ventricle choroid plexus is absent.
Generalized obstructive hydrocephalus is present in over 80% of neonates at birth.
Other CNS abnormalities are present in 70% of DWM.
The most common finding is callosal agenesis or dysgenesis.
A dorsal interhemispheric cyst may be present.
Gray matter abnormalities (e.g.,
heterotopias,
clefts,
and pachy- and polymicrogyria) are quite common associated abnormalities (to 50% of cases) [1-2].
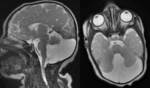
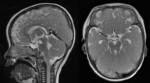
- Dandy-Walker variant including vermian hypoplasia (Fig.3) is characterized by the superior rotation of the vermis,
and variable cerebellar hypoplasia.
The overall posterior fossa volume is normal or less enlarged than in the classic Dandy-Walker malformation [1-2].
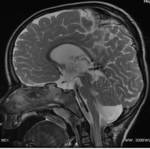
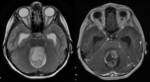
- Blake’s pouch cyst (Fig.4) is an ependyma-lined protrusion (diverticulum) of the fourth ventricle through the foramen of Magendie into the retrovermian cistern.
It is caused by lack of fenestration of the Blake pouch,
resulting in absence of communication between the fourth ventricle and the subarachnoid space and leading to hydrocephalus.
The posterior fossa is normal in size,
the fourth ventricle choroid plexus is present but displaced into the superior cyst wall.
The vermis is normal in size but rotated superiorly.
The consistent presence of hydrocephalus allows the differentiation of BPC from mega cisterna magna.
[1-2].
- Mega cisterna magna (Fig.5) represents only a focal enlargement of the subarachnoid space.
There is no mass effect on the cerebellar hemispheres or vermis and the vermis is normal.
Cerebellar veins and elements of the falx cerebelli can be displaced [1-2].
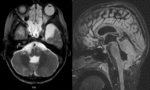
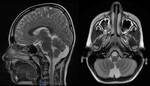
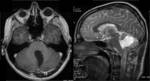
* Joubert Syndrom (JS) (Fig.6) incidences 1:80,000-100,000 live births [1].
The classic clinical presentation is a child with a developmental delay,
ataxia,
and oculomotor and respiratory abnormalities.
Anomalies of the kidneys,
eyes,
bones,
liver,
and bile ducts are common in the JS spectrum [1-2].
JS is characterized grossly by a dysmorphic vermis with sagittal clefting,
enlarged superior cerebellar peduncles,
and an elongated rounded fastigium of the fourth ventricle.
The anteroposterior diameter of the midbrain may be reduced [1-2].
MR is the cornerstone in establishing a diagnosis of JS.
The diagnostic criterion visible on axial scans is the "molar tooth" sign that consists of elongated,
thickened,
and horizontally oriented superior cerebellar peduncles,
a deep interpeduncular fossa and vermian hypoplasia.
The fourth ventricle,
cisterna magna and posterior fossa may appear enlarged [1-2].
DTI shows characteristic image - the fibers of the superior cerebellar peduncles do not decussate in the mesencephalon and the corticospinal tracts fail to cross in the caudal medulla [1].
Acquired cystic lesions:
Neoplasm associated cysts:
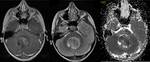
* Pilocytic Astrocytoma (PA) (Fig.7) as a slow-growing WHO grade I tumor is the most common pediatric CNS glioma and one of the most common pediatric cerebellar tumors representing 60% of all astrocytomas in children.
Additionally,
it may be associated with neurofibromatosis type 1 (NF1) [1,3].
Morphologically,
the tumor is a well-delineated cerebellar cyst with a mural nodule.
A solid,
more infiltrative appearance is also present but in the cerebellum dominates cystic presentation.
In MRI the mural nodule is iso-/hypointense on T1-weighted and iso-/hyperintense on T2-weighted images.
Strong but heterogeneous enhancement of the nodule in a cystic PA is typical.
Enhancement of the cyst wall itself varies from none to moderate [1,3].
* Medulloblastoma (MB) (Fig.8) is the most common malignant CNS neoplasm of childhood and the second most common overall pediatric brain tumor (after astrocytoma).
As a molecular compound group,
MBs together account for approximately 20% of childhood CNS neoplasms [1,4].
The classic form of MB accounts for 70% of all medulloblastomas and presents as a midline mass located within the fourth ventricle that focally infiltrates the dorsal brainstem and vermis.
Posteroinferior extension into the cisterna magna is common.
Classic MB tends to compress the fourth ventricle and cause obstructive hydrocephalus.
In one-third of children younger than 3 years,
the diagnosis is made due to life-threatening signs of intracranial hypertension.
Overall survival is good with surgical resection and adjuvant chemotherapy [1,4].
MRI is crucial for proper pre- and postoperative evaluation of MB.
Classic MB has relatively defined margins on imaging studies.
Despite this appearance,
40-50% of MBs show CSF dissemination at the time of initial diagnosis,
therefore preoperative contrast-enhanced MR of the entire neuraxis is recommended.
Almost all classic forms of MBs are hypointense relative to gray matter on T1-weighted and hyperintense on T2-weighted images.
Small scattered foci of necrosis and hemorrhage may be present while near 40% of classic forms contain cystic foci.
Peritumoral edema is present in one-third of cases.
Two-thirds of classic MBs show marked enhancement,
whereas one-third shows only subtle,
marginal,
or linear enhancement.
Because of their dense cellularity,
classic MBs often show moderate restriction on DWI [1,4].
Other acquired cystic/cystic like formations:
* Postinfectious and postoperative changes: Acute cerebellitis caused by either infectious,
post-infectious or post-vaccination agents is observed more commonly in children.
Neuroimaging is usually normal and recovery often occurs over weeks,
except in severe cases,
in which there are features of raised intracranial pressure,
hydrocephalus and brain herniation.
Such advanced forms of inflammation may resolve with cyst formation [5].
If only the suspicion of acute cerebellitis is made,
the MR examination is necessary [1].
Congenital,
fetal infections with Cytomegalovirus may cause a wide spectrum of changes,
also within the posterior fossa - periventricular pseudocysts formation,
cerebellar and cisterna magna abnormalities.
Initially,
they may be diagnosed using sonography while MRI is a method of choice for detailed evaluation of all lesions,
especially in the posterior fossa.
CT may be helpful in the visualization of calcifications [6].
Similarly,
the postoperative changes may present wide range of changes including the cyst-like structures and cerebro-spinal fluid spaces surrounded by glial tissue (Fig.9).
Postoperative changes are described usually in the follow-up examinations after tumor excision [1].