We evaluated a great number of fractures cases,
correlating them with anamnestic data about preexisting disease and clinical evolution,
and have observed differences between the biomechanics of vertebral atraumatic fractures.
We also notice that these differences can be demonstrated by imaging methods,
with distinct grades of accuracy,
even though all conditions lead to destruction of the vertebral bodies.
As described in the literature,
in pathological neoplastic fractures the trabecular bone is replaced by tumor cells with partial destruction of the vertebral body.
The timing of the fracture depends on the size and location of the tumor,
the extent of bone destruction,
and the bone mineralization status of the patient.
In osteoporosis cases,
there is a skeletal system disease determining bone loss,
both quantity and quality of bone tissue.
The main causes of osteoporosis are women with estrogen deficiency,
elderly men,
corticosteroid therapy cases,
chemotherapy treatment,
radiotherapy,
among others.
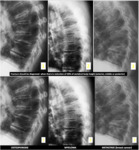
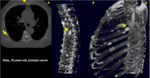
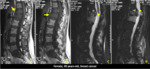
Plain radiography shows some difficulties in distinguishing whether the fracture represents a consequence of osteoporosis,
a metastatic lesion or some other primary bone neoplasm,
especially in acute and subacute stage,
in which neither bone radiographs nor scintigraphy is capable to do (Figure 1).
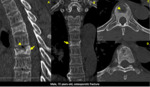
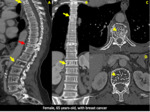
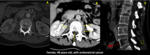
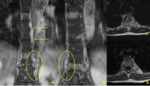
Computed tomography is the most used method in trauma and is the best suitable imaging technique for the evaluation of bone structure and fragments,
establishing the degree of cortical bone destruction.
Sometimes is even possible to make the etiological diagnosis by the typical findings of some lesions (Figures 2-5).
Magnetic resonance imaging is the method that provides more data for the distinction between osteoporotic and pathological fracture.
There are several potential signs,
but none of them are individually specific.
Morphological changes and intensity of signal are the main criteria and the combination of them increases specificity,
sensitivity and accuracy (close to 100%,
93% and 95% respectively).
Vertebral osteoporosis results in varying degrees of cortical and trabecular bone thinning,
but the hematopoietic tissue remains relatively constant.
When the bone substance has been lost or weakened,
the vertebral fat content increases and spontaneous pathological fractures may occur.
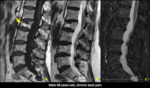
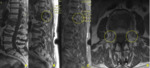
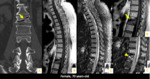
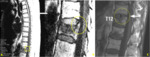
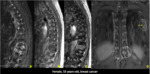
These phenomena have specific findings on MRI that favor benignity in acute or subacute osteoporotic fracture (Figures 6-12):
1 - Yellow marrow foci preserved;
2 - Preserved pedicles and posterior elements;
3 - Linear low signal T1WI representing the fracture line;
4 - Gas and / or liquid in a "slot";
5 - High signal range below the end plate in T2WI;
6 - No expansion of vertebral body,
no soft tissue mass;
7 - Triangular fragment in the posterior and superior wall of vertebral body;
8 - Other vertebral fractures are mainly old.
In metastatic compression fractures there is total or partial replacement of the normal bone marrow of the vertebral body.
The infiltration takes place initially through hematopoietic tissue and gradually leads to destruction of trabeculae and cortex resulting on structural bone weakening.
The fractures occur when vertebral body is infiltrated and most of hematopoietic and adipose tissue are replaced in irregular and infiltrative pattern.
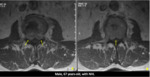
These changes can be correlated with MRI,
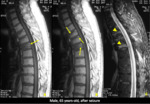
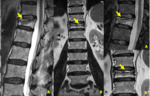
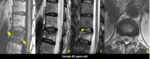
being the main findings that characterize metastases or other primary neoplastic conditions (Figures 13-17):
1 - Replacement of the normal signal of the vertebra;
2 - Altered pedicle;
3 - Convex posterior vertebral border;
4 - Epidural mass;
5 - Focal paravertebral mass;
6 - Other metastases;
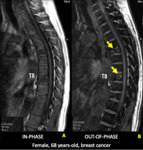
7 - Increased signal in out-of-phase images;
8 - Restricted DWI – High signal on DWI and low signal on ADC.
Abbreviations:
T1WI: T1 weighted imaging
T2WI: T2 weighted imaging
DWI: Diffusion weighted imaging
ADC: Apparent diffusion coefficient