Keywords:
Tissue characterisation, Metastases, Cancer, Biopsy, Ultrasound, MR, Mammography, Oncology, Lymph nodes, Breast
Authors:
F. traficante, M. Costantini, C. D. arru, E. FERRA, G. Demurtas, L. Saba; Cagliari/IT
DOI:
10.26044/ecr2019/C-1889
Results
From 1225 breast MR examinations performed in the study period (3 years from September 2015 to September 2018),
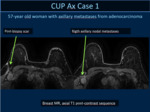
21 women with axillary nodal metastases from carcinoma and occult breast cancer were identified.
All these women underwent breast conventional imaging (mammography and ultrasonography) resulting negatives and lymph nodes biopsy diagnosing axillary nodal metastases from carcinoma.
Mean age of patients was 57,7 (range: 33-71).
Most of the patients came to our attention for the presence of an axillary mass.
Only two patients had symptoms related to the presence of skeletal metastases.
In both these patients the CT total body scan reaveled pathological lymph nodes in the axillary region.
All patient underwent axillary lymph nodes biopsy diagnosing metastases of adenocarcinoma or undifferentiated carcinoma.
As routine practice a careful review of first level breast imaging was performed.
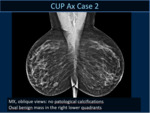
In no case a mammographic or sonographic alteration was detected.
As indicated ,
all patients underwent breast MR.
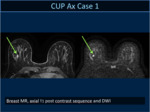
Breast MR detected suspicious enhancement in 15 of 21 cases .
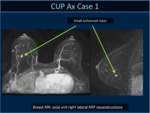
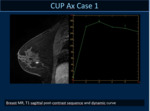
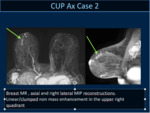
In 5 cases a small circumscribed mass was detected whereas in 10 cases linear/segmental non mass enhancement was observed.
Only 1 case (a small circumscribed mass) was assigned to BI-RADS 3 class.
All other lesions were assigned to BI-RADS 4 or 5 classes.
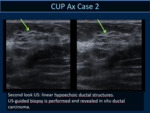
Second look US allows to the identification of an ultrasound alteration in 11 cases in which US-guided biopsy was performed.
Histological examination revealed a breast cancer in 9 cases and a benign lesion in 2 cases.
Pathological/radiological correlation was discordant in 1 benign case in which MR-guided biopsy was consequently indicated.
Totally 5 MR-guided biopsies were performed.
Enhancement areas revealed a cancer in 14/15 of cases.
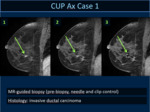
(Case 1:Fig.2,3,4,5,6).
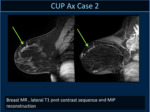
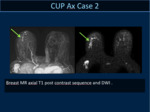
(Case 2:Fig 7,8,9,10,11).