Procedure details:
CT examinations
High-resolution CT of the temporal bone,
followed by image reconstruction in both the axial and coronal planes,
is required to evaluate the inner ear and its malformations.
Axial scanning is performed in planes parallel to the infraorbitomeatal line from the top of the petrous apex to the inferior tip of the mastoid bone.
Coronal reformatted images are obtained from the anterior margin of the petrous apex to the posterior margin of the mastoid.
MRI Examinations
The use of a 1.5- or 3-T MR imaging system is preferred for inner ear examinations,
and sedation is used in most children.
A thin-section gradient-echo sequence that is heavily T2 weighted is best suited for evaluation of the fluid-filled spaces of the membranous labyrinth and the eighth cranial nerve.
Volumetric acquisition is performed in the axial plane with sagittal and coronal reformatting.
Oblique sagittal reformatted images are obtained in planes per pendicular to the course of the seventh and eighth nerves in the internal auditory canal and cerebellopontine angle.
Routine axial T2-weighted imaging of the brain should be performed in all patients to exclude central nervous system causes of sensorineural hearing loss .
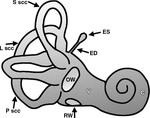
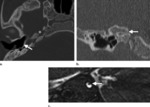
Normal Anatomy of the Inner Ear
- The inner ear consists of an osseous labyrinth that encloses a membranous labyrinth.
The osseous labyrinth consists of the vestibule,
cochlea,
semicircular canals,
vestibular aqueduct,
and cochlear aqueduct (Fig.
1).
- The vestibule is the central,
rounded portion of the osseous labyrinth.
It is continuous anteroinferiorly with the cochlea and posteriorly with the semicircular canals and the vestibular aqueduct.
The vestibular aqueduct is a tubular structure that arises from the vestibule and runs along the posteroinferior aspect of the petrous temporal bone.
It contains the endolymphatic duct and sac,
which are connected to the utricle and saccule of the vestibule.
The vestibular aqueduct is diagonally oriented in relation to the direction of the internal auditory canal (IAC).
The aqueduct,
which normally measures less than 1.5 mm in diameter,
approximates the size of the posterior semicircular canal,
which runs anterior and parallel to the aqueduct.
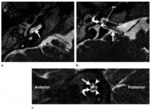
- There are three semicircular canals; these are designated as the superior,
lateral,
and posterior semicircular canals .
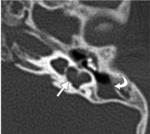
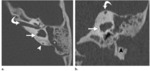
The posterior end of the superior semicircular canal joins the upper end of the posterior semicircular canal to form a common limb known as the common crus(Fig.
2).
- The cochlea consists of a canal that spirals 2½ to 2¾ times around a central column of bone (the modiolus).
The diameter of the canal decreases gradually as it proceeds toward the cochlear apex.
A delicate osseous spiral lamina that projects from the modiolus divides the cochlear canal into an upper compartment (scala vestibuli) and a lower compartment (scala tympani).
These two compartments communicate through an opening called the helicotrema,
at the cochlear apex.
The cochlear aqueduct is a thin osseous canal just inferior to the IAC and roughly parallel to it.
The cochlear aperture,
also known as the cochlear nerve canal,
is a small opening at the fundus of the IAC through which the cochlear nerve enters the cochlea(Fig.
2).
- The IAC is separated from the vestibule by the lamina cribrosa.
The IAC extends from the labyrinth to the cerebellopontine angle and contains the seventh and eighth cranial nerves .
The eighth nerve (vestibulocochlear nerve) is composed of three branches: The superior and inferior vestibular branches of the nerve occupy the posterosuperior and posteroinferior quadrants of the IAC,
respectively; the cochlear branch is located in the anteroinferior quadrant.
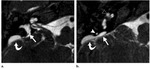
A normal cochlear branch of the eighth nerve should have approximately the same diameter as the facial nerve,
which occupies the anterosuperior part of the IAC(Fig.
3).
Image findings:
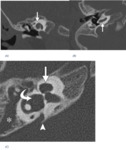
- Incomplete partition type II(mondini deformity):
• The cochlea consists of 1½ turns,
and the interscalar septum and osseous spiral lamina are absent.
• The basal cochlear turn appears normal,
but the middle and apical turns coalesce to form a cystic apex.
• The modiolous is present only at the level of the basal turn.
Type II incomplete partition is often associated with a large endolymphatic duct and sac and an enlargedvestibular aqueduct(Fig.
4,5).
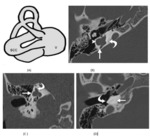
- Incomplete partition type I (cystic cochleovestibular malformation ):
•The modiolus is entirely absent.
• The cochlea has a cystic appearance; and the vestibule is often dilated,
forming a figure eight.
•.
The vestibular aqueduct is normal.
•The fact that the vestibule is distinguishable from the cochlea makes it possible to differentiate a type I incomplete partition from a common cavity(Fig.
6).
•The vestibule and semicircular canals are often malformed but may be normal .
Dense otic bone is present at the site where the cochlea normally would be and is best depicted on CT images.
•It is important to differentiate this anomaly from labyrinthitis ossificans,
in which normal-sized bone is seen anterior to the IAC,
with the bulge of the cochlear promontory produced by the basal turn of the cochlea; both features are absent in cochlear aplasia(Fig.
7).
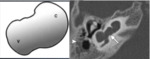
This malformation is defined by the absence of the normal differentiation between the cochlea and vestibule .
• CT and MR images show confluence of the cochlea and vestibule in a cystic cavity with no internal architecture .
•The width of the cavity is typically greater than its height,
with the average vertical diameter being 7 mm,
and the average horizontal diameter,
10 mm(Fig.
8).
• The semicircular canals are frequently malformed but occasionally normal.
- Complete labyrinthine aplasia:
•Complete absence of inner ear structures.
•A narrow,
atretic IAC is seen on high-resolution CT images.
•The eighth cranial nerve is not visualized on MR images.
•These abnormalities may be unilateral or bilateral.
In patients with unilateral complete labyrinthine aplasia,
the contralateral inner ear structures are often dysplastic.(Fig.
9).
Associations:
•Hypoplasia of the petrous bone.
• Absence of the round and oval windows.
• Flattening of the medial wall of the middle ear cavity.
•Skull base and vascular anomalies.
• Anomalous courses of the facial nerve.
- Malformations of the Vestibule and Semicircular Canals:
The malformed canals are usually short and wide but may be narrow.
In extensive malformations,
the vestibule is dilated and forms a common lumen with the lateral canal(Fig.
10). This type of abnormality,
which has been described as “lateral semicircular canal–vestibule dysplasia,” may be accompanied by a normal or malformed cochlea,
depending on the stage of inner ear development at the time of embryologic arrest.
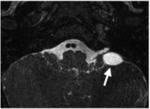
- Enlarged Vestibular Aqueduct:
An enlarged vestibular aqueduct,
or an enlarged endolymphatic duct and sac,
is the most frequent CT or MR imaging finding in patients with early-onset sensorineural hearing loss and was the most frequent inner ear malformation reported in some recent studies.
The abnormality is bilateral in as many as 90% of cases,
may be asymmetric,
and is slightly more common in females.
Although enlargement of the vestibular aqueduct most likely is the result of a developmental anomaly in the 7th week of gestation,
the vestibular aqueduct continues to develop throughout gestation and beyond; thus,
in some cases,
the malformation may actually be acquired and not congenital.The characteristic imaging feature seen at CT is enlargement of the osseous vestibular aqueduct.
At MR imaging,
the characteristic feature is enlargement of the endolymphatic duct and sac(Fig.
11).
- IAC and Cochlear Nerve Anomalies:
The normal diameter of the IAC ranges from 2 to 8 mm,
with an average of 4 mm.
An IAC with a diameter of less than 2 mm is described as stenotic.
The IAC may also be atretic or may have a bony septum that partitions it into two or more separate canals.
The morphologic characteristics and size of the IAC are not reliable indicators of the integrity of the cochlear nerve,
and normal size of the IAC and normal inner ear anatomy do not exclude a nerve deficiency; the nerve may even be absent when the IAC and labyrinth are completely normal.
Sagittal oblique images obtained in a plane perpendicular to the long axis of the IAC provide the best depiction of the four major nerves of the IAC: the facial,
cochlear,
superior vestibular,
and inferior vestibular nerves(Fig.
12).
Three types of cochlear nerve anomalies have been described.
In a type 1 cochlear nerve anomaly,
a stenotic IAC is seen with an absent eighth nerve.
In a type 2 anomaly,
a common vestibulocochlear nerve is found,
with hypoplasia or aplasia of its cochlear branch.
When this anomaly is associated with other inner ear malformations,
it is referred to as a type 2A malformation.
When the anomaly occurs in isolation (ie,
the inner ear is normal in other respects),
it is referred to as a type 2B malformation.
An increased incidence of posterior fossa abnormalities such as asymmetric dilatation of the fourth ventricle and arachnoid cysts has been observed among patients with complete labyrinthine aplasia .
Neuronal migration abnormalities in children with congenital sensorineural hearing loss also have been described.
Congenital cytomegalovirus infection contributes substantially to sensorineural hearing loss in many infant populations(Fig.
13).