Injuries to the urinary bladder are relatively uncommon due to its location deep in the pelvis,
where the urinary bladder is well protected against external forces.
Incidence is approximately 1.6% of all abdominal trauma [1].
A high level of clinical suspicion and knowledge of relevant anatomy plays crucial role in the diagnosis [2].
Most cases of the urinary bladder trauma can be managed nonoperatively and the correct classification of injury is necessary for proper management.
Anatomy:
The urinary bladder is a hollow muscular organ located at the base of the pelvis.
Anatomically it is divided to fundus,
body,
apex and neck [3].
The bladder is isolated from the anterior abdominal wall by a prevesical space named the space of Retzius.
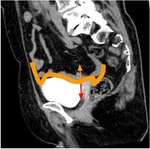
The peritoneal lining covers the bladder dome,
which is the weakest part of the bladder and the most vulnerable to damage when distended [4],
(Fig.1).
The ureteral orifices are located posteriorly and inferiorly,
and together with internal urethral orifice they define the vesical trigone,
a part sensitive to bladder distension with subsequent sensory output [5].
Mechanism of injury:
Car accidents are the most common cause of urinary bladder injury,
followed by falls from heights,
industrial trauma/pelvic crush injuries and direct hits to the lower abdomen [6].
Around 60-90% of patients with urinary bladder injuries caused by blunt force trauma have associated pelvic fractures,
and 44-68.5% of those patients have at least one other intra-abdominal organ injury.
Conversely,
pelvic fractures are associated with bladder injuries in only 3-4% of cases.
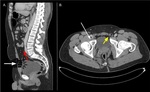
The incidence of extraperitoneal (34.2-86%) and intraperitoneal (14-50%) injuries varies among studies [7,
8].
(Fig.2)
Penetrating trauma is very rare in European countries,
but is more common in USA,
where it is usually result of either a gunshot wound or a stab wound.
In a gunshot-wound injury the pathway of projectile is unpredictable,
has high energy and causes significant damage to the affected tissues.
The injury of a stab wound has a more predictable pathway.
As opposed to blunt trauma,
penetrating trauma generally requires surgical exploration [9].
The iatrogenic injury of the urinary bladder is relatively common.
It occurs during obstetric and gynaecological procedures (e.g.
robotic radical hysterectomy 4,
38% - 4,59%),
followed by general surgical (abdominal cytoreductive surgery 4,5%) and urological interventions ( e.g.
transurethral resection of the bladder - TURB 3,5- 58%).
The main risk factors include previous surgery,
inflammation and malignancy.
Internal IBT mainly occurs during TURB.
Reported risk factors are larger tumours,
higher age,
pre-treated bladders (previous TURB,
intravesical instillations) and location at the bladder dome.
Perforations requiring intervention are rare (0.16-0.57%).
Extraperitoneal perforations are more frequent than intraperitoneal perforations [10].
Spontaneous rupture of the bladder has an exceptionally rare occurrence,
possibly caused by minor trauma with overdistended bladder,
or as a secondary effect to extreme urinary retention [11,
12] .
It has also been described as a potential complication in patients with bladder exstrophy [13]
According to the legend famous Danish astronomer and alchemist Tycho Brahe (Fig.
3.) had suffered spontaneous bladder rupture during banquet given by emperor Rudolph II in Prague,
when he had refused to leave the banquet to relieve himself because it would have been a breach of etiquette and then died several days later.
In fact his death was more likely caused by uremia or acute kidney failure [14].
Classification of urinary bladder injuries
The most important factor for further management when facing a urinary bladder rupture is to describe whether it is extra- or intraperitoneal,
or potentially a combined type.
It is common practice to use AAST classification of bladder trauma.
(table 1.)
Table 1.
|
Grade
|
Injury
|
Description of injury
|
|
I.
|
Hematoma
|
Contusion,
intramural hematoma,
partial thickness tear
|
|
II.
|
Laceration
|
Extraperitoneal bladder wall laceration under 2cm
|
|
III.
|
Laceration
|
Extraperitoneal (>2cm) or intraperitoneal (<2cm) bladder wall laceration
|
|
IV.
|
Laceration
|
Intraperitoneal bladder wall laceration >2 cm
|
|
V.
|
Laceration
|
Intra or extraperitoneal bladder wall laceration extending into the bladder neck
|
Extraperitoneal ruptures are the most common type and are often associated with pelvic fractures.
The injury can be caused by deformation of the pelvic ring or the bladder wall can be punctured by a sharp bone fragment.
The highest risk of bladder rupture is associated with patients suffering fractures of the pelvic ring with diastasis > 1 cm,
diastasis of the pubic symphysis > 1 cm and pubic rami fractures.
On the contrary,
a separated acetabular fracture has a low risk of associated urinary bladder injury [8].
Intraperitoneal ruptures are less common and are typically caused by direct blunt trauma to the abdomen,
for example by seat belts,
with distended urinary bladder.
The most vulnerable part of bladder in this scenario is the dome covered by peritoneum,
hence the intraperitoneal character of the rupture.
Injuries caused by penetrating trauma are also usually intraperitoneal [7].
Combined intra and extraperitoneal ruptures are generally rare and without an underlying fracture they are an absolute rarity [15].
Less severe types of urinary bladder injuries include contusion or interstitial rupture and the finding on imaging methods may be quite discrete,
with thickening and hematoma of bladder wall.
Diagnostic evaluation:
The typical clinical signs of urinary bladder rupture are hematuria,
inability to void,
abdominal tenderness,
abdominal distension ( think of urinary ascites),
uraemia and elevated of creatinine level (there is higher reabsorption of creatinine and urea nitrogen),
oliguria and visible penetrating injury.
If the urinary bladder rupture is suspected,
then the main diagnostic methods are CT or plain cystography,
cystoscopy,
excretory phase of CT or IVP (intravenous pyelogram),
in the last ultrasound.
Cystography is the preferred diagnostic method for non-iatrogenic bladder injury and for a suspected IBT in the post-operative setting.
Both plain and CT cystography have a comparable sensitivity (90-95%) and specificity (100%).
CT cystography is the main method in polytraumatic patients with pelvic injury.
It usually requires retrograde filling of the bladder with a minimum volume of 350 mL of dilute contrast material.
CT cystography visualizes intra and extraperitoneal free contrast fluid and adjacent injuries.
Extraperitoneal bladder injury is associated with flame-shaped areas of contrast extravasation in the perivesical soft tissues [16].
Contrast medium in the vagina is a sign of vesico-vaginal fistula.
Cystoscopy is used after intraoperative urinary bladder injuries for visualisation of perforation and location of the position of the trigone and ureteral orifices,
often after suburethral sling operations by the retropubic route.
An absence of bladder distension amid cystoscopy raises suspicion of a big laceration.
Cystoscopy is also recommended in diagnosing a foreign body [16].
Passive bladder filling in excretory phase of CT or IVP may show leak of contrast media,
but is not sufficient to exclude bladder injury if negative [17].
Can be used in unstable patients to detect free fluid in the pelvic cavity and to check distension of the urinary bladder.
When the ultrasound reveals a small contracted urinary bladder with copious free fluid anterior to the bladder wall,
there is suspicion for rupture of the urinary bladder.
The method alone is not sufficient to diagnose a urinary bladder injury [18].
Therapeutic management :
-
The most extraperitoneal ruptures can be treated conservatively,
bladder neck involvement,
bone fragments in the bladder wall,
concomitant rectal or vaginal injury or entrapment of the bladder wall will necessitate surgical intervention.
-
Intraperitoneal ruptures should always be managed by formal surgical repair because intraperitoneal urine extravasation can lead to peritonitis,
intra-abdominal sepsis and death .
Abdominal organs should be inspected for possible associated injuries and urinomas must be drained if detected.
In the absence of other intra-abdominal injuries,
laparoscopic suturing of the intraperitoneal rupture is possible [7].