INTRINSIC GROUP
Spinal epidural hematoma is an infrequent but very serious cause of acute neurologic deficit due to spinal cord compression that needs an early diagnosis and rapid surgical treatment [5].
Most cases are “spontaneous.” [6].
Traumatic situations occurs between 0.5% to 1.7% of all spinal injuries [5].
Besides trauma other non-spontaneous causes include coagulopathy,
pregnancy,
disc herniation,
tumor,
and arteriovenous fistula or malformation [7].
They tend to occur more frequently in the cervicothoracic region in the dorsal epidural space [1].
MRI is the gold standard in recognizing the real cause of cord compression.
The mosaic appearance is due to the different intensity areas caused by the hemoglobin degradation products is a pathognomonic sign of disease [8].
Case 1:
An 81-year-old female patient,
with a chronic myeloproliferative neoplasm,
was admitted in the context of a pulmonary embolism.
During the hospital stay,
and under anticoagulation therapy,
she had an accidental fall.
Twenty-four hours later,
bilateral distal limb mild paresis and bladder dysfunction signs and symptoms developed.
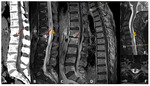
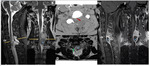
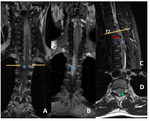
To rule out a post-traumatic complication an urgent spinal CT scan and a MRI confirmed the epidural hematoma (Fig.
2).
The patient underwent spinal decompression surgery with little symptom improvement.
- Infective: Pyogenic epidural abscess
Or spinal epidural empyema is an uncommon infection of the spinal extradural spaces with abscess formation.
There are two types: primary,
after the trauma,
iatrogenic manipulation or direct introduction of pathogens into the epidural space; and secondary: in case of hematogenous dissemination of microorganisms present outside the epidural space [3].
Patients with diabetes mellitus,
intravenous drug abuse,
chronic renal failure,
excessive alcohol ingestion,
immunodeficiency,
and local steroid injections are at greater risk factors for developing these infections.
S.
aureus is the most common agent [1].
Surgical drainage and prolonged antibiotic therapy remain the ideal treatment [3].
Case 2:
A 45-year-old male patient,
with history of non-treated C hepatitis and active intravenous drug abuse was admitted in the emergency room with severe lower back pain,
fever and a right groin mass.
There was a history of femoral vein self-puncture 8 days prior.
Four months before this event,
he was hospitalized and treated for bacterial endocarditis.
The initial examinations (chest,
abdominal,
pelvic and spine CT) were normal.
During the hospital stay,
he developed respiratory distress due sepsis and was admitted in the intensive care unit.
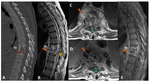
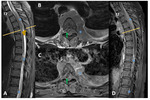
One month after the admission he underwent a second spine CT scan that revealed L1-L2 spondylodiscitis with epidural empyema (Fig.
3).
EXTRINSIC GROUP
- Degenerative: herniated disk
Many degenerative spine changes,
such as herniated disc,
may cause mass effect on the epidural space.
Disk herniation is a displacement of intervertebral disk material beyond its normal confines,
resulting from a perforation of the annulus fibrosis and posterior longitudinal ligament [9].
It can cause compression of the anterior epidural space/ thecal sac,
with lateral or medial irritation of nerve root or cauda equina [4].
Most sequestrated and extruded fragments show peripheral contrast enhancement,
attributed to an inflammatory response with granulation tissue [4].
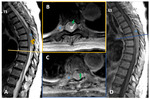
Case 3:
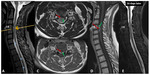
A 54-year-old female patient with secondary progressive multiple sclerosis with sudden onset high degree of disability with the need of a wheelchair to move.
A brain and spine MRI were performed,
with no new demyelinating lesions,
but showing a cervical disk herniation with granulation tissue causing cord compression with edema.
She was hospitalized in the Neurosurgery department and with a conservative approach,
she clinically improved (Fig.
4).
- Infective: Pott’s spine /Tuberculosis (TB)
Pott’s disease or Pott’s spine refers to a tuberculous infection of the spine and adjacent soft tissue.
While it is uncommon in the western world,
there has been an increasing number of cases HIV-related,
presented as multidrug-resistant tuberculosis with rapid progression and a higher mortality rate [1].
Spinal tuberculosis accounts for 2% of all cases of TB,
15% of extrapulmonary TB,
and 50% of all cases of skeletal TB [10].
The diagnosis remains difficult because it is an indolent disease [1].
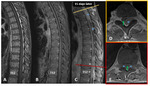
Case 4:
A 64-year-old male patient with an HIV infection under irregular medical treatment,
was admitted in the emergency room with a one-month history of fever,
night sweats,
persistent cough and weigh loss.
Recently he had developed mid-back pain and was unable to walk due to limb paresis.
He also complained of urinary incontinence.
An emergent spine CT scan followed by a MRI suggested spinal tuberculosis. A CT-guided percutaneous biopsy of the paravertebral lesion confirmed the diagnosis (Fig.5).
- Benign neoplastic: Neurofibroma
Neurofibromas are commonly associated with neurofibromatosis type 1 (NF1),
particularly when multiple,
but can also occur sporadically [1].
NF1 is a common autosomal dominant disorder in which affected individuals develop both benign and malignant tumors [11].
Neurofibromas develop as discrete focal cutaneous/subcutaneous tumors or more diffuse plexiform neurofibromas that grow along the length of nerves frequently involving multiple nerve fascicles,
branches and plexuses [11].
Plexiform neurofibromas associated with NF1 show malignant degeneration in 3% to 5% of cases [1].
They can cause local pain,
radiculopathy and spinal cord compression.
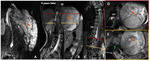
Case 5:
A 11-year-old girl with the diagnosis of NF1 with associated left giant spinal and paraspinal thoracolumbar plexiform neurofibroma and progressive scoliosis - partially corrected with surgery,
was admitted in the emergency room because walking abnormalities due to left limb pain.
She also complained of back pain and urinary retention.
At physical examination there was a paraparesis with left-limb plegia.
A spinal cord compression was suspected,
confirmed with the spine MRI that elucidate neurofibroma growth causing marked cord compression and edema,
compatible with malignant transformation – neurofibrosarcoma confirmed on histopathology (Fig.
6).
- Benign neoplastic: Schwannoma
Schwannomas are benign,
encapsulated nerve sheath tumors composed of proliferating Schwann cells.
They are usually solitary lesions and are most commonly sporadic [1].
Multiple schwannomas occur with neurofibromatosis type 2 (NF2).
Together with neurofibroma,
they represent the most common primary neoplasia in the spine as well as in the intradural extramedullary space [12].
They are more frequent in adults and if presented in a young child,
investigation for NF2 is mandatory.
On imaging schwannomas and neurofibromas are mostly indistinguishable.
Although most of these tumors (both schwannomas and neurofibromas) are entirely intradural,
they can also be entirely extradural [1].
Case 6:
A 26-year-old female patient,
with an irrelevant past medical history,
attended the emergency room with a neck and left upper limb pain.
The CT scan revealed an intra spinal canal lesion.
The MRI confirmed the presence of an expansive lesion.
The tumor was surgically removed,
with the histopathology result of schwannoma (Fig.
7).
- Malignant neoplastic: Multiple Myeloma
Multiple myeloma is characterized by multifocal malignant proliferation of monoclonal plasma cells within the bone marrow.
It accounts for approximately 1% of all malignant diseases and represents about 10% of hematologic malignancies [13].
It is multicentric disease,
with the most common localization being the spine [14].
The bone marrow involvement causes cortical disruption and invasion of the surrounding tissue.
Bone pain,
pathologic fractures and a spinal cord compression are the most common findings.
Case 7:
A 53-year-old female patient with a known multiple myeloma,
presented with progressive paraplegia and a recent onset of severe back pain.
An emergent spine MRI was requested confirming disease progression and spinal cord compression (Fig.
8).
- Malignant neoplastic: metastases
Spine is the most common osseous site for metastases [15] and third most common after lung and liver metastases.
Breast,
prostate,
thyroid,
kidney,
and lung cancers are common primary tumors found.
[3].
Pain is the most frequent symptom and,
in both osteolytic or osteoblastic metastases an epidural component may cause radiculopathy and cord compression [1].
Posterior elements,
especially the pedicles,
may be involved by this disease [3].
Case 8:
An 83-year-old female patient with a medical history of breast cancer treated 14 years ago,
was admitted in the emergency room for a pneumonia.
During her hospital stay,
she developed progressive paraparesis and urinary retention.
The MRI revealed spinal osteolytic lesions and spinal cord compression (Fig.9).
- Malignant neoplastic: lymphoma
Lymphoma is the most common malignancy of the epidural space [1].
Plasmablastic lymphoma is a rare aggressive variant of diffuse large B-cell lymphoma,
the most common subtype of non-Hodgkin lymphoma [16].
It was initially proposed as a novel entity in 1997 in a series of HIV-positive patients [17].
It has very rarely been described as presenting with a paravertebral mass or in association with cord compression [17,
18,
19].
Treatment for cord compression includes laminectomy,
chemotherapy,
and radiotherapy [17].
Case 9:
A 33-year-old male patient was admitted into hematologic department because of worsen of lower back pain and paraparesis.
He had been diagnosed with a plasmablastic lymphoma 4 months prior to this event.
He also had an HIV infection known in the last 10 years but only under medical treatment in the last 8 months.
Two weeks before this hospitalization,
the spine MRI revealed disease progression with resulting cord compression (Fig.
10).
- Malignant neoplastic: Mesenchymal chondrosarcoma
Chondrosarcoma is the third most common primary malignant bone tumor,
encompassing 10% to 25% of all primary bone sarcomas [1].
Mesenchymal chondrosarcomas are rare malignancies of the bone and soft tissues and represent 10% of all primary chondrosarcomas [20].
They are more aggressive,
occurring in younger patients,
with lower survival rates and have a high propensity to metastasize to the lungs,
lymph nodes,
and other bones [21,22].
Extra skeletal mesenchymal chondrosarcoma is relatively frequent in association with the meninges,
but rarely in the spinal region [20].
Case 10:
A 13-year-old girl was admitted in the emergency due to 2-month history of progressive walk abnormalities.
She also presented signs and symptoms of bladder and bowel dysfunction.
The spine MRI showed an extradural thoracic solid lesion,
involving the right intervertebral foramina from T1 to T5.
Because of the rapid-clinical deterioration a hematologic disease was consider.
She underwent spinal decompression surgery and the histopathology report confirmed a mesenchymal chondrosarcoma (Fig.11).