EC/DC are suspected upon physical examination.
Imaging is usually requested before surgical removal to confirm the diagnosis and evaluate the extension in depth.
Ultrasonography (US) usually shows a well-defined,
round to ovoid,
hypoechogenic mass in the subcutaneous tissue.
Larger lesions can be a little heterogeneous or present a laminated appearance,
like the layers of an onion skin,
that corresponds to the alternating layers of compacted keratin and desquamated squamous cells seen histologically.
The capsule may be echogenic and calcified sometimes.
In Colour Doppler study there is no associated vascularity.
These findings are not pathognomonic.
Computed Tomography (CT) generally shows a well-defined unenhancing nodule,
with similar density to that of water.
They have smooth and slender margins,
which may be sclerotic in EC.
These cysts may contain small calcification,
more commonly DC.
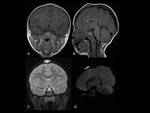
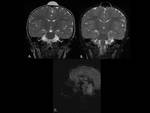
The Magnetic Resonance Imaging (MRI) appearances of EC/DC are of well-circumscribed lesions,
with a noninfiltrating rim and an accompanying sinus tract that can be often visualized on imaging.
EC may be of mixed intensity on all imaging sequences.
The layers of keratinizing material are rich in water and lipid and can appear as areas of high signal intensity on both T1- and T2-weighted images.
However,
they usually show low/intermediate intensity,
similar to muscle,
on T1-weighted imaging (T1-WI).
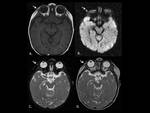
These cysts exhibit restricted diffusion on diffusion-weighted imaging (DWI).
DC have MRI characteristics similar to those of fat,
being typically hyperintense on T1-WI and presenting a variable intensity signal on T2-weighted images (T2-WI).
The signal of these lesions can be nulled on T2-Fat Sat sequences due to the fatty content.
They generally do not present restricted diffusion on DWI.
Any midline scalp lesion suspected of being a DC should undergo preoperative radiographic evaluation to exclude intracranial extension,
especially important for orbital DC with palpably indistinct margins,
as such lesions may require deep orbital dissection.
The best way to evaluate for deep extension of a midline lesion is controversial.
Both CT and MRI may be used in a complementary fashion,
with CT better evaluating bony abnormalities and MRI better defining soft tissue structures.
Some clinicians argue that CT alone is adequate; however,
false negatives have been reported.
MRI is superior for more detailed depiction of any possible intracranial connection and for the presence of a potential sinus tract.
Even though EC/DC generally do not enhance after contrast administration,
the capsule and the solid component may show enhancement in some cases.
Whereas,
the appearance of a more irregular type of enhancement is suggestive of prior rupture with a secondary inflammatory reaction.
The radiological differential diagnosis includes lipoma,
pilar cyst,
neurogenic tumours as neurofibroma,
and myxoid tumours.
Infected cysts may have heterogeneous contents and stranding in adjacent tissues so they may mimic an aggressive lesion.