There are several groups of pathologies that may be responsible for an exclusive or predominant involvement of the white matter.
Their imaging presentation is nonspecific
The clinical context has a strong orientative value in pathologies acquired white matter : neonatal suffering,
history of infection or vaccination,
exposure to a toxic, chemotherapy ...
The combination of clinical symptoms with MRI abnormalities is often characteristic,
leading to early diagnosis and early therapy.
I- A reminder of the anatomy of the white matter :
The white matter accounts for about 60% of the total volume of the brain.
It contains:
- Projection fibers: consist of efferent and afferent fibers uniting the cortex with the lower parts of the brain and with the spinal cord.
- Commissures: consist of white matter tracts that cross the midline,
connecting the two cerebral hemispheres.
- Association fibers: they connect cortical regions of the same hemisphere.
Myelin: is a lipid-rich substance that is layered around axons.
It improves nerve conduction and protects neurons.
II- Brain maturation and myelination
The organization of the cortex,
gyration and development of the synapses begin in the third trimester of the pregnancy.
This process will continue after birth and will be accompanied by axon myelination for a period of 10 to 15 years,
with a caudo-cranial direction.
It begins at the level of the posterior cranial fossa,
brainstem and cerebellum,
then continues on the supra tentorial structures.
III- Imaging in acquired white matter disorders in children :
Acquired abnormalities of white matter in children are common and are dominated by perianal anoxic ischemic pathology,
infectious encephalitis,
and postinfectious disease, including acute disseminated encephalomyelitis (ADEM).
In addition,
the white matter may be the site of non-specific lesions (edema,
gliosis ...)
MRI allows to appreciate the myelination,
to specify the extent of the lesions and to bring prognostic elements.
MRI sequences and findings:
1- The most important MRI sequences for studying te white matter are: T1,
T2,
FLAIR and Spectroscopy.
- During the first year of life,
the Flair sequence is of little relevance,
given the low myelination of the brain at this age.
- During the first 6 months of life,
T1 sequences are the most sensitive.
Non-myelinated white matter is hypointense relative to gray matter.
Gradually,
it becomes iso then hyperintense to gray matter.
- From 6 months to 2 years,
T2 sequences become more sensitive.
Non-myelinated white matter is hyperintense compared to gray matter.
Gradually,
she becomes iso then hypointense.
- The last zones to remain in relative hypersignal until 3 to 4 years are periventricular white matter.
2- Sequences after contrast may be necessary,
thus making it possible to provide arguments for the etiological diagnosis.
IV- Acquired white matter disorders in childen :
1- neonatal hypoxic ischemic encephalopathy:
The clinical context (prematurity,
IUGR,
acute or chronic fetal distress,
obstructed labor,
etc.) helps to guide the diagnosis.
In the acute phase,
diffusion and MRI spectroscopy sequences make it possible to specify the extent of the lesions and to provide prognostic elements.
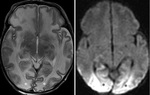
Nodular lesions disseminated hyperintensel T1,
hypointense T2,
hyper DWI,
coresponding to a coagulative necrosis.
Spectroscopy can show a peak of lactates that is a pejorative prognostic element.
Secondly,
if the diagnosis was not made,
periventricular ischemic-hemorrhagic lesions are most often associated with moderate ventricular dilation.
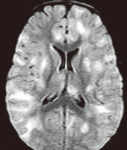
Leucomalacia is the consequence of ischemic lesions affecting the white matter. The evolution of this leucomalacia is towards the gliosis (hyperintesities T2 and Flair),
or towards the cystisation.
Lesions of the basal ganglia are possible
2- Infectious pathologies: TORCH
Abnormalities of white matter may also be observed in the neonatal period and in the small infant at the stage of sequelae of a maternal-fetal infection (Cytomegalovirus,
Toxoplasmosis,
Herpes virus..).
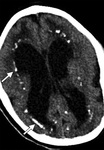
Imaging shows white matter anomalies associated with other morphological abnormalities: microcephaly,
calcifications (CT++),
ventricular dilatation,
gyration disorders..
3- Post-infectious pathologies : ADEM
MRI is the key of diagnosis,
objectifying typically multiple lesions and disseminated,
predominant in the white matter.
The involvement of basal ganglia can be noted in 50% of cases.
The CSF study makes it possible to exclude differential diagnoses,
such as infectious meningoencephalitis,
which justifies urgent and specific treatment.
4- Multiple sclerosis:
In MRI,
lesions are the same as in adults and remain completely aspecific.
These are typically hyperintense T2 and Flair lesions of periventricular white matter with a long axis perpendicular to that of the corpus callosum.