IMAGING TECHNIQUES
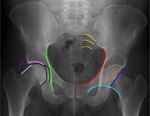
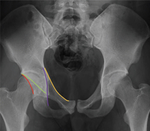
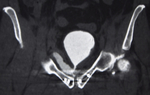
Hip X-ray :
Performed in the emergency room with the patient in supine position.
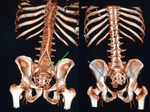
The detection of pelvic ring fractures is one of the priorities in the traumatized patient [Fig.
1],
as they are often related to complications that severely affect mortality.
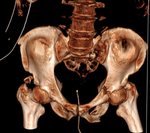
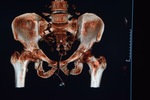
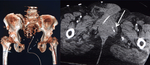
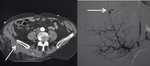
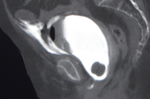
Contrast enhanced-CT:
CT allows an accurate overall assessment of the thoracic-abdominal and pelvic traumatic lesions.
It also highlights occult lesions (not detectable with other imaging techniques),
performing a full rachis screening,
showing vascular lesions and bleeding in progress and a precise grading of the lesions [Fig.
2].
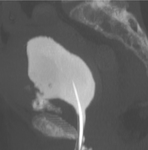
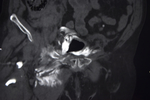
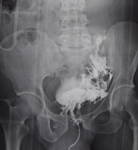
Cysto-CT:
Main indications for cysto-CT:
- macro-haematuria associated with fracture of the pelvis,
in the absence of renal lesions;
- evaluation of possible bladder lesion and the site of the rupture;
- evaluation of the pathways of the extravasation,
the extent and type of urine-hematic collection can be: intraperitoneal,
extraperitoneal,
combined.
[4]
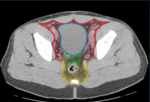
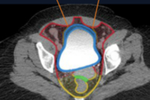
Accurate identification of the site of bladder lesions is important as intraperitoneal and combined injuries require surgical intervention,
while for extraperitoneal ruptures a drainage catheter is sufficient [Figure 3-5].
Urethrography:
The exam should be performed in haemodynamically stable patients: in particular the evaluation and treatment of lesions in pelvic vessels and viscera take precedence over the execution of urethrography.
The standard technique in males consists in positioning through the external meatus of a 6-8 F Foley catheter with a 5 ml inflatable balloon,
20-30 ml of diluted water-soluble iodinated contrast medium are injected under fluoroscopic guidance,
slowly and continuously,
until an opacification of the bladder meatus is visualized.
In women,
the investigation is more complex and can be used a hysterosalpingography catheter.
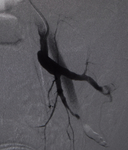
Angiography:
Digital subtraction angiography identifies therapeutic targets and anatomical variants.
Generally a femoral access is used.
The rationale for arterial embolization is to achieve hemostasis by reducing the arterial flow or by causing an obstruction of the artery responsible for bleeding without causing ischemic necrosis of downstream tissues.
An excessively proximal embolization can be ineffective in terms of haemostasis,
while too distally can cause ischemic necrosis.
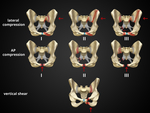
YOUNG AND BURGESS CLASSIFICATION OF HIP FRACTURES
The fractures are classified on the basis of predominant force vectors: [Fig.
6]
- Lateral compression (50-70% of cases);
- Vertical cutting force (14% of cases);
- Combined mechanisms.
[6-7]
Lateral compression
It occurs after side impacts in road accidents or falls,
both by direct trauma of the pelvis and by indirect transmission through the femoro-acetabular joint.
An internal rotation of the hemi-pelvis occurs towards the midline ("closed book" fracture): the front portion of the ring is broken at the ileopubic and ischio-pubic branches,
with frequent compression of the bony heads.
The distance between the sacrum and the lateral wall of the pelvis is reduced.
TYPE 1: compressive fracture of the pubic branches associated with a fracture of the anterior aspect of the sacral wing.
The ligaments remain intact.
They generally occur in elderly patients with osteopenia or osteoporosis with a low-energy trauma.
They are stable fractures that usually do not require surgery.
TYPE 2: Fracture with decomposition of the pubic branches associated with fracture of the iliac bone with displacement of the bony heads with possible associated extension to the adjacent sacroiliac joint.
In younger patients,
with a more solid bone trabeculation,
an opening of the sacro-iliac joint occurs by breaking the posterior sacroiliac ligament instead of the iliac fracture.
They are rotationally unstable but vertically stable.
TYPE 3: "closed book" fracture on the impact side and "open book" fracture (contralateral).
[Fig.
7]
They occur in cases of high-energy trauma.
The force that determines internal rotation from the pelvis on one side is also transmitted contralateral,
where extrarotation of the hemi-pelvis occurs.
Since the sacro-spiny and sacrotuberous ligaments are also damaged,
they are unstable both rotationally and vertically.
The overall volume of the pelvis is reduced and generally no bleeding occurs.
Any damage to the viscera or vascular structures can be determined by bone fragments on the bladder or iliac artery.
Trauma of the bladder may also occur due to increased intrapelvic pressure,
resulting in intraperitoneal rupture.
The involvement of nerve structures occurs in particular at the level of the sacral roots in the context of compressive fractures of the sacrum.
Antero-posterior compression
The forces involved are directed along the sagittal axis,
antero-posteriorly.
They are typical of both motor vehicle accidents,
motorcycles and falls.
They produce an extrarotation of a semi-pelvis or both,
with a fulcrum of rotation on the sacro-iliac joint ("open book”).
The pubic symphysis may be dislodged or surrounded by vertical fractures on the pubic branches.
TYPE 1: Dislocation of the pubic symphysis with diastase of less than 2.5 cm.
The sacroiliac articulations open slightly,
but the sacroiliac ligaments remain intact.
Fairly rare type,
they are both rotational and vertical stable.
TYPE 2: Dislocation of the pubic symphysis with diastase greater than 2.5 cm.
Diastase of the anterior side of the sacro-iliac joints.
Only the posterior sacroiliac ligaments remain intact,
so they are rotationalally stable and vertically unstable fractures.
The fracture of the transverse process of L5 is an independent factor of instability due to the loss of the function of the corresponding ileo-lumbar ligament.
TYPE 3: Opening of the pubic symphysis associated with complete dislocation of the sacroiliac joint due to rupture of the ligaments.
They are globally unstable fracture for the complete separation of the lower limb from the trunk.
They are often associated with arterial and / or venous bleeding hemorrhages (most often affected arteries the upper glutea and the internal pudenda).
Vertical shear
They are caused by high-energy trauma with a cranio-caudal direction,
as happens in falls from above with landing on an extended leg.
In the presence of compact bone,
lesions of the ligaments frequently occur,
with dislocation of the pubic symphysis and sacroiliac.
In patients with osteopenia or osteoporosis,
vertical fractures of the anterior pubic branches preferentially occur and sacral fractures posteriorly.
The characteristic sign of these fractures to be found in the hip X-ray is the cranial-caudal dislocation of an iliac crest with respect to the contralateral.
A sign of instability is given by the lack of pairing of the lower margins of a sacroiliac joint,
that determines global instability.
A vertical displacement of the articular heads of the symphysis is not necessarily a sign of instability.
In fractures with a vertical cutting force,
lesions to the viscera are often associated,
which makes the cysto-CT indicated.
In the presence of hematuria and hip fracture,
without spreading at the cysto-CT,
urethrography is indicated.
[Fig.
8]
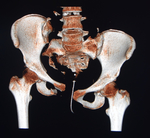
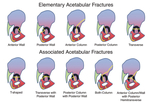
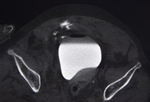
ACETABULAR FRACTURES
Acetabular fractures are usually generated when the femoral head and / or neck impact on the acetabulum.
The classification system most used [8-9] [Fig.
9-10] identifies 5 elementary fractures:
- back wall: affects the posterior wall of the acetabulum;
- front wall: affects the front wall of the acetabulum;
- anterior column: affecting the anterior portion of the acetabulum and the anterior column of the hip bone;
- posterior column: they affect the posterior portion of the acetabulum and the posterior column of the hip bone;
- trasverse: divide the acetabulum into an upper and a lower portion.
When fractures occur that divide the hip bone into three or more major fragments,
variable combinations of the 5 elementary fractures are found:
- T-shaped fracture;
- transverse fracture with involvement of the posterior wall;
- fracture of the posterior column with involvement of the posterior wall;
- fracture of both columns,
front and back;
- column fracture and anterior wall and transverse hemifracture involving the posterior column.
VASCULAR INJURIES
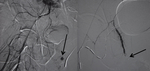
Active arterial bleeding (or blush) in both angiography and angio-CT consists of the early appearance of an iodine-contrasting extravasation area,
with no washout in the subsequent phases,
which tends to gradually fade opaque in surrounding hematoma.
[Fig.
11-13] [10-13]
Pseudoaneurysm is a region bounded in space,
but without its own walls,
in communication with an arterial vessel through its parietal discontinuity.
After administration of contrast medium,
it becomes opaque at the same time as the vessel,
progressively presenting densitometric values similar to the vessel lumen,
until complete wash out.
Other features that differentiate from a blush are the defined margins and the often round or oval shape.
[Fig.14-15]
Arterial occlusion may be the result of acute thrombosis due to intimal traumatic injury,
with possible thromboembolism.
Occlusion can also be linked to arterial spasms in full-thickness vessel lesions.
[Fig.
14]
Focal stenosis is an endoluminal irregularity with filling defects in the vessel.
Arterial dissection can be determined directly by the traumatic impact or by stretching; often occurring in patients with underlying arteriopathies.
Arteriovenous fistula is an abnormal communication between an artery and an adjacent vein.
Rare in traumas,
it manifests as a too early opacification of a pelvic vein,
with possible visualization of the fistula.
BLADDER LESIONS
The risk of bladder rupture depends largely on the degree of bowel distension at the time of impact.
Failing in recognizing these injuries results in a significant increase in mortality [14].
Sandler et al.
[15] classified:
Type 1: Bladder contusion: an incomplete lesion of the mucosa.
Although manifested with hematuria,
cysto-CT is negative.
It’s the most frequent bladder finding in polytrauma,
not considered a major injury.
Type 2: Intraperitoneal rupture (10-20% of the major bladder traumas),
usually due to a direct hit on the distended bladder [10].
The sudden increase in intravesical pressure causes the breakdown.
Cysto-CT shows the spreading of contrast material between the intestinal loops,
between the mesenteric sheets and in parieto-colic location.
Type 3: Bladder interstitial injury. Relatively rare lesion,
it’s an intramural bladder laceration with intact serous.
Cysto-CT can demonstrate the presence of contrast material that dissects the wall in the absence of extraluminal spreading.
Type 4: Extraperitoneal rupture. [Fig.
16] The most frequent (80-90% of cases),
it’s generally caused by a penetrating trauma; in contusive trauma by tearing of the wall by bone fragments.
It can be divided into “simple” [Fig.
17] (extravasation is confined to the perivescical space) and “complex” (extravasation reaches fascial planes) [Fig.
18–19].
Type 5: Combined rupture (5-12%).
URETHRA LESIONS
Relatively frequent (∼24%) [16], if not diagnosed they can cause long-term morbidity: cicatricial stenosis,
incontinence and impotence.
Urethral ruptures are more frequent in men at the junction between the prostatic and membranous urethra.
The urethra is vulnerable due to its proximity to pubic branches and pubo-prostatic ligaments.
The portion at most risk is the posterior urethra,
in particular in traffic accidents and falls [17].
At least 20% of patients have associated bladder tears.
The injuries of the anterior urethra are less frequent due to its relative mobility.
Urethral lesions are less common in females because the urethra has a shorter length,
is located more internally,
has greater elasticity and a less rigid anchorage to the pubic branches.
The two most commonly used classification systems for urethral lesions classified the lesions according to their treatment [18],
or on the basis of the anatomical location of the lesion [19-20].
Urethra lesions are classified in: contusion,
stretch injury,
partial disruption,
complete disruption [Fig.
20].