IMAGING TECHNIQUES
- Ultrasonography (US),
can be used as an initial imaging modality for the evaluation of abdominal pain or palpable abdominal masses.
Is less useful for evaluating the entire abdomen and pelvis,
because has a limited depth of penetration.
- Multidetector Computed Tomography (MDCT),
is the most widely used cross-sectional imaging modality for the abdomen and pelvis,
being the method of choice in the evaluation of the peritoneal cavity and the retroperitoneal anatomy.
Plays an integral role in the characterization of the retroperitoneal masses,
can be used to define tissue components,
establish the involvement of adjacent structures,
guides a biopsy and judge the operability.
MDCT offers multiplanar reconstructions,
necessary to study the anatomic site of origin of a mass and its relationship to adjacent organs and vasculature.
- Magnetic Resonance Imaging (MRI),
is increasingly used to depict retroperitoneal disease.
Disadvantages include motion artefacts caused by respiration and peristalsis.
Also,
the spatial resolution is lower than that of MDCT.
MRI has superior contrast resolution than MDCT and helps to define the characteristics of fluid collections.
Another advantage it is the lack of ionizing radiation,
so important in the younger patients,
particularly those who need repeated imaging.
PATHOLOGY
RETROPERITONEAL TUMOURS:
Form by a various and heterogeneous group that includes: tumours with an origin in the retroperitoneum but outside the organs (primary),
from retroperitoneal organs or from distance organs (secondary).
The imaging findings of most retroperitoneal tumours are nonspecific.
MDCT can help to identify certain radiological signs that define the attachment or not of a mass to an organ:
1.
Determine if is retroperitoneal or not: observing the displacement of normal structures.
2.
Identify the organ of origin: this sign is positives when existing a secondary tumour.
- The beak (claw) sign: when a mass deforms the edge of an adjacent organ into a "beak" shape,
it is likely that the mass arises from that organ.
- The embedded organ sign: when there is intimate contact between the mass and the organ of origin,
a desmoplastic reaction and sometimes ulcerations are observed (positive sign).
On the contrary,
a mouldable organ,
compressed by a mass,
is deformed into a crescent shape (negative sign).
- The phantom or invisible organ sign: if an organ cannot be seen,
it is probably the origin of the mass.
There may be false positive,
as in the case of large sarcomas that invade the adrenal gland.
- Prominent feeding artery sign: the hypervascular masses in most cases are supplied by feeding prominent arteries that can be visualized at MDCT and it helps to understand the origin of the mass.
3.
Identify patterns of growth and dissemination:
- Lesions surrounding normal structures and vessels without invading or compressing them,
and affecting more than one compartment: lymphangiomas and lymphomas.
- Lesions that are located along the sympathetic chain: paragangliomas or ganglioneuromas.
4.
Assess the enhancement pattern:
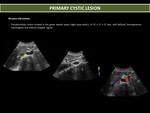
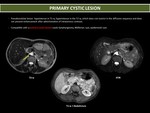
- Absence of enhancement: cysts,
haematomas,
and lipomas.
- Early enhancement and rapid washing: paragangliomas and Castleman's disease.
- Early enhancement and delayed or imperceptible washing: most tumours (benignant or malignant),
such as neurilemomas and paragangliomas.
- Late enhancement: neurogenic tumours,
desmoids,
leiomyomas,
leiomyosarcoma and lymphoma.
5.
Identify characteristic tumour components: fat,
myxoid stroma,
necrosis,
cystic degeneration,
calcifications.
1.
PRIMARY RETROPERITONEAL TUMOURS:
It is a very rare and heterogeneous group of lesions that arise within the retroperitoneum space but outside the organs,
accounting for 0.1-0.2 % of all malignancies.
The majority of they are malignant.
1.1 MESODERMAL TUMOURS:
Most retroperitoneal tumours have a mesodermal origin and the sarcomas represent the 90% of the mesodermal retroperitoneum primary malignancies,
being the most frequent liposarcoma and leiomyosarcoma.
The retroperitoneum is one of the most common locations for soft-tissue sarcomas.
When a mass is discovered in this space and cannot be shown to originate from a visceral organ,
sarcoma should be considered at the top of the differential diagnosis.
The incidence is higher in the fifth and sixth decades of life.
Most of the time are clinically silent until they have a very large size.
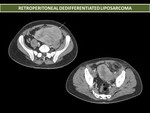
· Liposarcoma is the most common sarcoma in adults and the more frequent in the retroperitoneum.
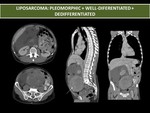
It can be separated into four types,
distinctly different histologically and genetically,
and does not have the same biologic behaviour.
Well-differentiated liposarcoma is the most common histologic type (40%–45%),
does not metastasize,
but it may progress into a dedifferentiated liposarcoma.
In MDCT is a well-defined,
round-oval,
mass with fat attenuation.
At MRI,
the signal intensity of the fat resembles the signal intensity of the subcutaneous fat,
showing high signal intensity on T1 and T2 weighted and lost of signal intensity on fat-suppressed sequences.
May have some non-fat components with soft-tissue attenuation like thin or irregular septa,
nodular soft-tissue components,
and thin blood vessels.
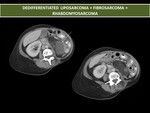
Dedifferentiated liposarcomas have the capability to metastasize.
Are solid soft-tissue masses,
heterogeneous,
with regions of well-defined fat and myxoid areas.
May show calcification and ossification.
Myxoid liposarcoma is the second more frequent type (30%–40%).
Present an abundant myxoid matrix with high-water content that is hypodense on MDCT,
hypointense on T1-weighted MRI,
and hyperintense on T2-weighted,
showing enhancement,
important to distinguish it from a cystic mass.
Pleomorphic liposarcoma is the rarest type,
with less than 5% of cases.
Is a poorly defined soft-tissue mass with no typical features on the imaging tests and lack of fatty elements.
In general,
a biopsy is necessary for all masses that are not clearly liposarcoma,
because the imaging features in the rest of sarcomas are not specific.
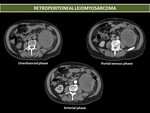
· Leiomyosarcoma has female predominance,
is the second most common retroperitoneal sarcoma,
with tumour cells resembling differentiated smooth muscle cells.
Many of these tumours arise in the smooth muscle tissues,
others from the IVC or another veins.
On MDCT appears as a large solid mass,
characteristically heterogeneous because of the enhancement of solid portions,
and the nonenhancing areas of degeneration,
necrosis,
and haemorrhage.
This tumour does not have fatty elements.
At MRI,
there are no specific findings.
Respect to skeletal muscle is iso-hypointense on T1-weighted,
heterogeneously hyperintense on T2-weighted,
and with heterogeneously enhancing.
When it is arising from the IVC or major veins may manifest as an intraluminal mass,
an extraluminal mass,
or both.
1.2 NEUROGENIC TUMOURS:
Represent 10-20% of primary retroperitoneal tumours and occur in younger patients.
· Paraganglioma or extra-adrenal pheochromocytoma (with origin in paraganglionic cells),
it is more frequent in the third-fourth decades of life with no sex predilection.
On imaging,
appears as a paraaortic well-defined lobular and heterogeneous mass,
with areas of haemorrhage and necrosis and an intense enhancement.
The biopsy is not recommended with the risk of death by hypertensive pressure and haemorrhage.
· Ganglioneuroblastoma or Neuroblastoma (with origin in the sympathetic nerves or ganglionic system).
Neuroblastoma is a malignant tumour,
rare in adults,
but very common in children.
The most common locations are the adrenals,
the retroperitoneum and the kidneys.
On imaging,
it appears as a larger mass with irregularly shaped that is covered by a thin capsule.
Enhancement is low and heterogeneous.
Ganglioneuroblastoma is a tumour with elements of benign ganglioneuroma and malignant neuroblastoma.
It is a paediatric tumour (2-4-year age group),
with no sex predilection.
The mass could be solid or cystic with solid components.
2.
SECONDARY RETROPERITONEAL TUMORS:
2.1 LYMPHOMA:
Is the most common malignant retroperitoneal tumour (30%) and can be Hodgkin or non-Hodgkin type.
On imaging,
it appears as a well-defined homogeneous mass,
with mild homogeneous enhancement,
since they lack degeneration or necrosis.
Typically,
the tumour spreads between normal structures without compressed them and tends to surround adjacent vessels with the "floating aorta sign".
RETROPERITONEAL FIBROSIS:
A proliferation of fibrous tissue that surrounds the aorta,
the IVC and the anterolateral region of the ureters.
More common in men of 40-60 years.
The majority are idiopathic,
and others are by drugs or metastases with desmoplastic reaction.
In MDCT present like soft tissue density that surrounds the vessels with no displacement of the ureters or the aorta,
and not bone destruction.
In MRI it is isointense with respect to muscle in T1-w,
in acute phases it is hyperintense in T2-w with important enhancement and in late phases,
it is hypointense and hypocaptant.
RETROPERITONEAL HAEMORRHAGE:
It is produced by trauma,
aortic aneurysm rupture,
anticoagulant therapy,
blood dyscrasia and tumours that bleed spontaneously (hypernephroma is the most frequent,
angiomyolipoma,
myelolipoma,
pheochromocytoma or metastases).
CT is the method of choice in acute haemorrhage (<2 weeks),
observing hyperdense areas.
The finding of areas of similar density to the contrast in the interior of the collections is a sign of active bleeding.
In some cases,
can be mass-like,
but the fluid tends to spread along the fascial planes of the retroperitoneal compartments.
MRI is useful in subacute and chronic hematomas because CT can confuse them with a tumour.