Atypical locations of the disease included: brain,
orbit,
neck,
mediastinum,
intraperitoneal cavity,
pelvis,
adrenal gland,
psoas,
quadriceps muscles,
and breast. Diagnosis was confirmed by hydatic serology,
US,
CT,
MRI and histopathological examination of the specimen for operated patients.
Cysts may be single or multiple,
uni- or multiloculated and thin- or thick walled.
More specific signs include visualization or calcification of the cyst wall,
the presence of daughter cysts and membrane detachment (2).
CT and MR imaging,
alone or in combination,
are helpful in the diagnosis of hydatid disease.
Although CT is superior in detecting calcification of the cyst wall or septa,
MRI is better in detecting multiplicity and defining the anatomic relationship of the lesion with the adjacent structures and helps in surgical planning (5,
6).
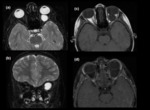
Brain:
Hydatid disease affects rarely the central nervous system (1% of cases) and is more common in children (4,
5).
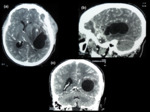
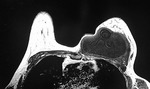
Intracranial hydatid cysts are commonly solitary (Figure 1) and multiple cysts are rare.
Intracranial hydatid cysts may also be classified as primary or secondary depending on whether other organs haven't / have been involved (4).
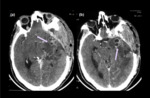
The secondary multiple cysts result from spontaneous,
traumatic or surgical rupture of the primary intracranial cyst (Figure 2).
Patients with intracranial hydatid cysts usually present with focal neurological deficit and features of raised intracranial pressure.
The typical intracranial hydatid cysts present as a well defined solitary oval or cystic mass in the middle cerebral artery territory in parietal lobes,
although they can be seen in any location including skull vault,
extradural,
intraventricular,
meningeal,
posterior fossa and brainstem (4).
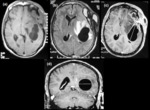
CT and MR imaging demonstrate attenuation or signal intensity similar to that of cerebrospinal fluid (Figure 1,
3).
Although the lesion may cause extrinsic compression of the ventricular system with subsequent hydrocephalus,
there is no associated edema as is typically seen in abscesses and cystic tumors (5).
The lesion does not enhance after intravenous administration of contrast material,
and calcification is extremely rare.
When present,
edema and post contrast enhancement indicate ongoing inflammation.
Presence of significant edema may indicate the rupture of the cyst and may be present in postoperative cases (Figure 2).
Such cases are difficult to differentiate from other cystic lesions with enhancement and peripheral edema such as abscesses,
large granulomas or cystic gliomas (7).
Kohli et al.
(8) performed in vivo MR spectroscopy (MRS) studies in a patient with intracranial hydatid cyst and found,
besides lactate,
alanine and acetate,
a large resonance for pyruvate.
The MRS pattern appeared different from the other cystic lesions of the brain and they have suggested MRS as an adjunct to imaging in the differential diagnosis of intracranial hydatids.
Orbit:
Orbital involvement occurs for 0.3% of all hydatid cysts and it is more prevalent among young patients (5,
9).
Typically,
an orbital hydatid cyst is unilateral and occurs with or without hydatid cysts located elsewhere in the body.
It tends to involve the retrobulbar tissues either within the muscle cone or outside in the superolateral or superomedial angle.
The most frequent clinical findings are proptosis,
chemosis,
lid edema,
visual impairment,
and restriction of extraocular motility (10).
Radiological findings play an important role in preoperative differential diagnosis.
Orbital ultrasonography is a useful test when a "double wall sign" has been observed (10).
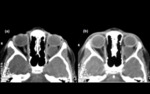
CT of the orbital hydatid cyst demonstrates a hypodense,
unilocular,
well- defined homogenous mass with a hyperdense rim (Figure 4).
MRI demonstrates a cystic lesion with a low signal intensity on T1-weighted images and high signal intensity on T2- weighted images,
without rim enhancement after contrast medium administration (Figure 5) (11).
Neck:
Hydatid disease in the neck is quite rare,
even in areas where the disease is endemic,
with only a few cases reported in the literature (12).
The diagnosis of cervical Echinococcus infection mainly depends on the clinical history of the patient,
diagnostic radiological findings and serologic tests.
Cervical hydatid cysts are usually slow-growing,
fluctuant,
painless masses.
Histopathological evaluation of the excised specimen and fine needle aspiration cytology usually leads to the diagnosis.
Since puncture of the cyst may lead to an anaphylactic reaction due to spillage of hydatid fluid,
the use of fine needle aspiration is controversial at present (12).
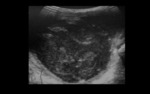
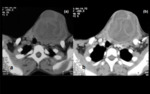
Imaging modalities like Ultrasound,
CT and MRI help to determine the cystic avascular nature of the lesion (Figure 6,
7).
Daughter cysts,
vesicles and internal septa can also be demonstrated (13).
Mediastinum:
Primary mediastinal hydatid cysts are quite rare.
Symptoms of mediastinal hydatid cysts depend on their size and location and whether or not they exert any compression on the neighboring structures.
The most serious complications include leakage of the hydatid material to the neighboring vessel,
causing embolization and/or anaphylaxis with possibly fatal consequences (14).
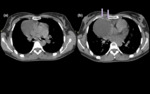
Chest radiograph,
Ultrasound,
CT and MRI facilitate diagnosis.
Chest radiograph oriented the diagnosis by showing a mediastinal water tone,
often rounded or oval (16).
Thoracic ultrasound allows confirmation of the diagnosis when the lesion is accessible and also reveals the fluid character of the opacity and,
in many cases,
the proligerous membrane,
pathognomonic of hydatid cysts (15).
CT often accurately defines the relationship of the lesion to the adjacent structures.
The most common CT finding of a mediastinal hydatid cyst is a homogenous mass with fluid (Figure 8).
The presence of peripheral calcifications supports diagnosis (14).
MR imaging,
with its superior soft tissue resolution,
can also provide us with a clear delineation of the cyst.
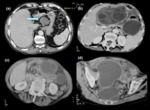
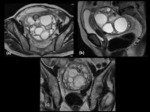
Intraperitoneal and pelvis:
Peritoneal hydatidosis is almost always secondary to hepatic disease,
although some unusual cases of primary peritoneal hydatidosis have been described (2)with an overall frequency of 13% (17).
Peritoneal involvement is usually undetected unless cysts are large enough to cause symptoms.
Most of the cases of peritoneal hydatid disease are secondary to previous surgery for liver hydatidosis.
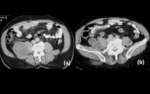
Accurate and rapid diagnosis of peritoneal hydatid disease is possible because of the availability of modern imaging techniques,
and the surgical procedures are decided on radiological findings (Figure 9,
10).
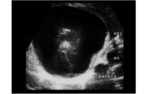
Ultrasound and CT scan are the radiological methods of choice for assessing the number of hydatid cysts in the abdomen and assessing the changes in size,
number and density of lesions in response to drug therapy (18).
Ultrasound is particularly useful for detection of cystic membrane,
septa,
and to look for hydatid sand.
CT scan best demonstrates cyst wall calcification and cyst infection and enables better delineation of extent of disease (Figure 9).
Thickening,
calcification of wall,
reduction in size and number of cysts are taken as therapeutic response on follow up (17).
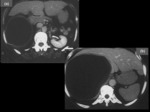
Adrenal Gland:
Hydatid cyst of the adrenal gland is rare as this entity has been reported in only 7% of all adrenal cysts and constitutes less than 1% of all cases (19).
Adrenal hydatid cysts usually form in association with generalized echinococcosis.
Most adrenal cysts are asymptomatic,
they are usually found as incidental findings on imaging studies or incidentally during surgery.
When symptoms are present,
most are related to local visceral compression.
Rarely,
endocrine abnormalities like arterial hypertension are seen in adrenal hydatidosis (4).
Hydatid cyst identification in the adrenal gland is based mainly on ultrasound and CT scan (Figure 11,
12).
MRI shows the characteristic low signal intensity rim of the hydatid cyst on T2- weighted images.
Both MR and CT images are able to show the exact anatomic extent,
size,
volume and position of the mass,
the number of cysts,
the relationship to other organs and possible complications (9).
The presence of calcifications in the adrenal mass very much supports a diagnosis of hydatidosis.
However,
the definitive diagnosis is made by macroscopic and microscopic examination of the cyst.
Muscle:
Primary muscular hydatid cysts are rare,
accounting for 3% of all patients with hydatidosis (4,
9).
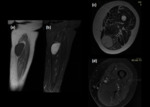
Primary hydatic cysts of the lower extremity muscles are usually solitary and unilocular or multilocular (Figure 13).
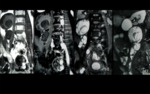
Psoas muscle is an unusual location for hydatid cyst accounting for only 1 to 3% of cases and can be unilateral or bilateral (21).
Hydatid of psoas muscle can be isolated (Figure 14,
15) or associated with hydatid disease elsewhere in body.
Ultrasound is a useful tool for orienting the diagnosis of any tumefaction of the soft tissues,
showing the size,
localization and type of the cyst (22).
CT is especially valuable for surgical planning.
On CT scan they appear as a well-defined cystic lesion with daughter cysts that may contain wall calcification,
septae or debris without the enhancement on intravenous contrast (Figure 14) (20).MRI is the examination of choice in case of suspicion of hydatid disease of muscle,
due to its ability to adequately demonstrate most features of hydatid disease,
with the exception of calcifications (9).
The classic MRI findings include a multivesicular cyst,
a low-intensity rim ("rim sign") on T2- weighted images or a detached membrane (Figure 13,
15).
The most pathognomonic sign is that of daughter cysts within larger cysts (22).
Breast:
Hydatid cyst of the breast is very rare even for patients living in endemic areas and accounts for only 0.27% of all cases.
It is very challenging to differentiate it from other tumoral lesions of the breast.
However,
it should be included in differential diagnosis of breast lumps.
Typically,
the patient presents with painless breast lump,
which increases slowly in size without regional lymph node involvement.
It might mimic fibroadenoma,
phyllodes tumors,
chronic abscesses,
or even carcinoma. Preoperative diagnosis can be made by fine needle aspiration cytology where scoleces,
hooklets or laminated membrane can be identified. It is a safe procedure,
as no complications were mentioned in the literature. The disease can be diagnosed by radiologic or serologic means,
both of which are not definitive.
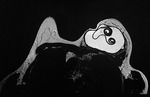
Mammogram may show a circumscribed mass,
the characteristic ring-shaped structures inside the mass in over penetrated view strongly suggests breast hydatid cyst.
The ultrasound and Magnetic Resonance Imaging (Figure 16,
17) are helpful diagnostic tools.
Hemagglutination tests may be helpful in diagnosis. The treatment of a hydatid cyst of the breast is complete excision.
Albendazole may decrease the recurrence rate of hydatid cyst disease (23).