Despite it is challenging and sometimes confusing,
AVNH diagnosis relies on imaging.
The most used approach consists of starting the study of the patient with plain radiographs and,
when considered,
requesting more imaging techniques,
like MRI,
computerized tomography or bone scan. Lets review some of them before deepening in the staging process.
Simple X-rays
Because of their availability and low cost,
plain radiographs are the most appropriate initial test in the management of hip pain,
and thus imaging evaluation of AVNH should begin with radiography.
Both frontal and frog-leg lateral projections should be obtained[1,3,5].
Although radiography is insensitive for early changes of AVNH,
which typically require months to occur,
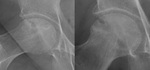
the imaging features are often characteristic (fig.2).
The prototypical radiographic appearance is of patchy areas of lucency and sclerosis.
The sclerotic margin surrounding the lesions corresponds to the host bone response to wall off the areas of necrosis [3].
Plain radiographs may also show early areas of articular collapse,
typically involving the anterolateral and anterior femoral head [3,5].
The necrotic process will develop a bone sinking which creates the crescentic subchondral lucency,
or ”crescent sign”,
representing the collapse of the subchondral bone (fig.3).
If not stopped,
this process will lead to progressive articular collapse and secondary osteoarthritis[3,6].
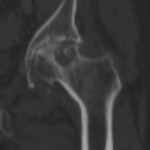
Computerized tomography
Computerized tomography (CT) is considered the most sensitive test for detecting subchondral fractures of the femoral head [1].It is also an important tool in surgical planning for rotational arthroplasty[3].
However,
CT is not recommended for early detection of AVNH because of its lesser sensitivity compared to scintigraphy or MRI [1,2,5].
CT results also helpful in visualizing small areas of collapse which can´t be seen on plain films or MRI [1,3,5].
Probably,
the greatest disadvantage of CT is the use of radiation (fig.4).
Magnetic resonance imaging
MRI is considered the best choice in AVNH diagnosis,
with the highest sensitivity and specificity compared to plain radiographs,
computed tomography,
or scintigraphy [1,2,4,7].
It is considered the most useful screening tool for early diagnosis,
and also for quantitative evaluation of the disease extent,
as well as staging of the disease [1].
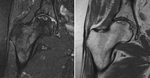
There are certain features considered diagnostic of the disease: a band-shaped lesion with low signal intensity rim surrounding the necrosis on T1-weighted images (fig.5),
and a low signal intensity outer rim with a high signal intensity inner rim (“double-line” sign) on a T2-weighted image [1].
The high-signal-intensity line seen on T2-weighted MR images appears to represent fluid accumulating in the subchondral fracture,
which may indicate a breach in the overlying articular cartilage [5].
There are also two imaging findings that increase the risk of development AVNH,
which are a thick physeal scar and an early conversion to yellow marrow[3].
When diagnosing or staging AVNH the use of contrast-enhanced MRI is usually not necessary,
although some studies in animals have demonstrated an increase in sensitivity for detecting osteonecrosis in the femoral head.
AVNH postcontrast MRI shows typically a lack of enhancement of the necrotic tissue [3].
Different MRI techniques,
such as diffusion sequences,
T2 mapping,
or apparent diffusion coefficient (ADC) mapping have also been proposed to evaluate AVNH.
For instance,
ADC values in these lesions are significantly higher than in the normal bone marrow,
but there are not significant differences among AVNH lesions at different stages,
and therefore ADC mapping shows limited value for staging the process[4].
Differential diagnosis
There are some conditions involving the femoral head that can simulate AVNH in MRI,
leading to misdiagnosis.
The two most challenging diseases are transient osteoporosis of the hip (bone marrow edema syndrome) and subchondral insufficiency fracture.
Transient bone marrow edema syndrome
Transient bone marrow edema syndrome,
also called transient osteoporosis,
is a rare condition in which an intense hip pain episode is followed by spontaneous regression without any specific treatment after some months.
This pain is typically of sudden onset,
without previous trauma,
and the characteristic MRI finding is a widespread marrow edema throughout the proximal femur,
while AVNH,
on the contrary,
shows a focal distribution[1,3].
Transient osteoporosis of the femoral head reveal osteopenia at plain radiographs and diffuse marked increased radionuclide uptake in the bone scan (without central photopenia as happens in AVNH) [3]. Transient bone marrow edema syndrome has been reported to coexist or even be a potential precursor of AVNH [1].
Subchondral insufficiency fracture
Subchondral insufficiency fracture of the femoral head presents with an acute onset of hip pain,
usually occurring in the elderly adults after minor trauma.
It is related to bone fragility in the context of osteopenia [1].
Both subchondral insufficiency fracture and AVNH present a low-signal-intensity bandlike region in the superolateral region of the femoral head,
however,
in AVNH the band usually shows a well delineated line that is concave,
curving away from the cartilage surface resembling a mirror image (while in subchondral insufficiency fracture,
the bandlike region is convex toward the articular surface) [1,3].
Staging avascular necrosis of the femoral head
Various staging systems have been developed for assessment of AVNH.
A total number of sixteen different systems have been identified,
and the list continues growing.
Of these,
four classification systems account the vast majority of the reported studies,
being the Ficat and Arlet Classification (table 1) the most frequently used system (63 %),
followed by the University of Pennsylvania system (Steinberg),
the Association Research Circulation Osseous (ARCO) system (table 2) and the Japanese Investigation Committee (JIC)[1]. Although,
there is still no consensus regarding which of them is the most effective,
some studies have found that the JIC classification exhibits the highest reliability[7]. It should be mentioned that in the staging process significative discordance on the classification of the AVNH lesions has been found between plain radiographs and MRI,
especially in intermediate stages (ARCO II vs III),
with poorer sensitivity,
specificity and predictive values for radiographies[8].
All of these staging systems share the progression from radiologically occult disease to the femoral head collapse and final development of secondary osteoarthritis.
The clinical significance of AVNH is basically dependent on the likelihood of articular collapse.
Imaging predictors of this lesion are therefore essential to identify and prescribe the correct treatment[3]. The lesion size and extend of femoral head involvement appears to be the main factor in predicting outcome in AVNH.
Assessing the size of lesions on plain radiographs may be challenging and inaccurate,
therefore the use of plain radiographs has not been widely applied for lesion size estimation.
On the other hand,
there is wide evidence that the extent of necrotic lesions in MRI is more precise and may allow us to predict the risk of femoral head collapse[2].
Another MRI features related to increased likelihood of femoral head collapse and stage include increasing volume of joint effusion,
presence of large surrounding edema,
the presence of subchondral fracture,
and the location of the lesion[1,3].
Ficat and Arlet classification
As already mentioned before,
the Ficat and Arlet classification remains the most widely used and reported system nowadays,
despite the fact that it was developed before the advent of MRI.
It has been modified multiple times,
being the four-stage version the most widely adopted.
Although various studies have demonstrated that it should not be used alone to classify AVNH because of its poor inter and intra-observer reliability[6],
we will review its staging pattern,
as it has been used as a frame for most of the other staging systems.
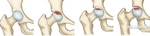
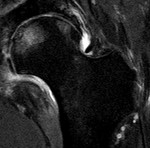
Stage I is defined by normal plain radiographic appearance of the femoral head,
with a possible increase in uptake of tracer on bone scintigraphy or increased bone marrow signal with edema on MRI (fig.6).
Stage IIA is defined by presence of diffuse sclerosis,
osteoporosis and/or cysts.
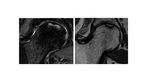
At Stage IIB,
subchondral fracture (“crescent sign”) and/or segmental flattening of femoral head should be present (fig.7).
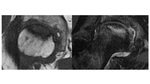
Stage III shows a broken contour of femoral head and/or bone sequestrum with a normal joint space (fig.8).
Stage IV is characterized by further collapse,
flattening,
and destruction of the femoral head,
with secondary osteoarthritic changes (fig.9)[3,6].



![Table 1: Classification of Ficat and Arlet. References: Sultan AA, Mohamed N, Samuel LT, Chughtai M, Sodhi N, Krebs VE, Stearns KL, Molloy RM, Mont MA. Classification systems of hip osteonecrosis: an updated review. Int Orthop. 2018 Jun 18. [Epub ahead of print]](https://epos.myesr.org/posterimage/esr/ecr2019/148206/media/824475?maxheight=150&maxwidth=150)
![Table 2: ARCO Classification. References: Sultan AA, Mohamed N, Samuel LT, Chughtai M, Sodhi N, Krebs VE, Stearns KL, Molloy RM, Mont MA. Classification systems of hip osteonecrosis: an updated review. Int Orthop. 2018 Jun 18. [Epub ahead of print]](https://epos.myesr.org/posterimage/esr/ecr2019/148206/media/824476?maxheight=150&maxwidth=150)
