Presentation/Acuity
Symptoms of acute onset ovarian/adnexal torsion include moderate to severe pelvic or lower abdominal pain,
often of sudden onset,
which may be sharp,
dull,
or colicky in quality.
The pain may radiate to the flank,
back,
or groin.
Patients may also exhibit nausea and vomiting.
After hemorrhage occurs,
patients may also present with vaginal bleeding.
Later,
fever and peritoneal signs may indicate the presence of necrosis.
Laboratory values of anemia and leukocytosis may indicate severe hemorrhage and necrosis,
respectively.
The presentation of acute isolated tubal torsion is similar to other types of torsion,
with sudden onset of abdominal pain and nausea with possible vomiting.
Unilateral abdominal pain is well correlated with the side of pathology [7].
Symptoms may vary with age.
In premenarchal patients,
pain may be more diffuse in quality.
Longer duration of symptoms before presentation in these patients may be responsible for higher rates of fever and restlessness [15].
In infants,
presenting symptoms are more likely to include feeding intolerance,
abdominal distension,
irritability,
and vomiting [16].
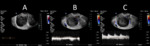
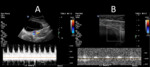
Symptoms of torsion may be intermittent or wax and wane in cases where partial or intermittent adnexal flow is preserved.
These cases may present with imaging findings of torsion but normal flow on Doppler ultrasound,
and should not be mistakenly interpreted as normal (Figure 3).
In cases of torsion that do not resolve spontaneously and go untreated the infarcted adnexal components will undergo necrosis.
Patients may present with ongoing vague abdominal pain,
but will often recall a recent period of more severe pain when questioned.
Imaging
Ultrasound is the initial imaging modality for the assessment of adnexal torsion.
With the exception of isolated tubal torsion,
the primary sonographic finding in acute adnexal torsion is ovarian enlargement,
which occurs due to obstructed venous outflow.
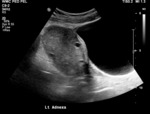
Common additional findings include a twisted pedicle (“whirlpool sign”),
peripheral displacement of follicles (due to edema and/or hemorrhage) (Figure 4),
pelvic free fluid,
abnormal ovarian location (especially in the the midline) (Figure 5),
and an underlying cyst or lesion (Figure 6).
The patient will likely experience pain in reaction to transducer pressure.
In cases of chronic (missed) torsion,
the infarcted ovary may appear hemorrhagic or cystic.
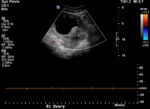
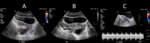
On the Doppler portion of ultrasound examination,
the most common finding in acute torsion is absent venous flow.
The presence of venous flow does not exclude torsion,
as slow flow may continue during acute torsion or normal flow may be present in cases of intermittent torsion.
Arterial flow is commonly present even during acute torsion,
though its absence is a poor prognostic indicator (Figure 7).
The presence of both ovarian and uterine vasculature further complicates Doppler assessment,
as the uterine vessels typically remain patent and may be confused for ovarian vessels by the examiner.
When performing or interpreting an ultrasound examination for torsion,
the possibility of isolated tubal torsion should be considered.
Tubal flow should be assessed in cases where any pathology or abnormal appearance in this region is noted (Figure 8).
Despite the superior sensitivity and specificity of ultrasound,
adnexal torsion is often first imaged on CT as part of examinations for non-specific indications of generalized pelvic or lower abdominal pain.
The emergency radiologist must always assess the ovaries and consider this diagnosis,
and if necessary recommend ultrasound for confirmation.
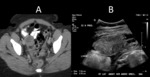
On CT,
common signs are similar to ultrasound but not as well visualized.
Unique findings on CT include decreased or absent enhancement,
compared to the contralateral side,
in acute cases and periadnexal fat stranding.
In certain cases,
hemorrhagic products may also be better appreciated on CT.
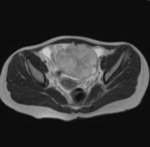
MRI has no practical use in the diagnosis of torsion,
however is often necessary for further assessment of cysts or lesions identified on the initial modality (Figure 9).
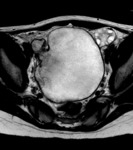
MRI may also be useful in distinguishing hemorrhage from other pathology (Figure 10).
Additional Clinical Considerations
It is important for the radiologist to realize that clinicians referring to “torsion” are usually focused on the possibility of acute torsion of the ovary,
and may not have considered other stages of acuity,
adnexal anatomy,
or underlying pathology.
Additionally,
clinicians often assume that the presence or absence of Doppler flow is the determining factor in the radiologic diagnosis of torsion.
The radiologist should carefully choose wording,
both verbal communication and the final report,
to acknowledge the breadth of possible adnexal torsion presentations.
Positive findings should include a level of acuity,
the exact anatomy that is torsed,
and comment on the presence or absence of lesions.
On otherwise suspicious ultrasound examinations with normal flow,
the fact that torsion is not excluded on the basis of flow should be explicitly communicated.