The radiologist is commonly confronted with bone lesions in children,
with up to 42% of all bone lesions, occuring in the first two decades of life.
Bone lesions include true bone tumors and tumor-like lesions.
Fortunately,
More than half of all childhood bone tumors are benign.
The most common pediatric benign bone tumors include osteochondroma,
non-ossifying fibroma (NOF), Eosinophilic Granuloma (EG), simple bone cyst (SBC),
and aneurysmal bone cyst(ABC).
The most common malignant pediatric bone tumors include Osteosarcoma (15% ) and Ewing sarcoma.
Although cross-sectional imaging such as CT or MRI can be useful,
plain film continues to be the primary and the most important imaging modality in the initial workup of a bone tumor.
If a lesion is clearly benign radiographically,
cross-sectional imaging should not be necessary.
The bone biopsy with anatomopathological examination is not systematic,
but must be carried out in the slightest doubt.
Differentiating between benign and malignant bone tumors is not always straightforward; however,
it is possible to distinguish between them by evaluating characteristics such as:
- Lesion margin: It’s a tumor biologic activity marker,
accurately described by the Lodwick's well-established grading system and the alternative Modified Lodwick-Madewell Grading System(Fig. 1). Sharply demarcated margins (1A and 1B) are described as those with a sharp border that indicates a tumor slowly growing,
which suggests benignity. Conversely,
grade II margins are poorly defined or indistinct,
more suggestive of an aggressive process with fast-growing pace such as Ewing sarcoma or osteosarcoma,
but can also be seen in osteomyelitis.
- Pattern of bone destruction: Malignant tumors demonstrate rapid growth and infiltration causing more aggressive bone destruction.
Moth-eaten and permeative bone destruction[grade IIb] are described in malignant bone tumors such as Ewing sarcoma and osteosarcoma,
but can be seen with osteomyelitis.(Fig. 1)
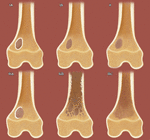
- Periosteal reaction: Periosteal reaction results when cortical bone reacts to one of many possible insults.
The appearance of periosteal reaction is determined by the intensity,
aggressiveness,
and duration of the underlying insult. Smooth,
uninterrupted periosteal reaction is seen in non-aggressive,
benign tumors ( Fig. 2 a,b).
In contrast,
irregular or interrupted periosteal reaction is seen in aggressive or malignant tumors ( Fig. 2 c).
“Sunburst” or the hair-on-end subtype and “onion-skin” or multi-lamellated periosteal reaction are commonly described in malignant tumors( Fig. 2 e,f,g).
Codman triangle ,
where a portion of periosteum is lifted off of the cortex by tumor at a leading edge,
is also associated with malignancy especially,
osteosarcomas.( Fig. 2i)
Moreover,
the periosteum in children is more active and less adherent to the cortex than in adults.
Thus,
periosteal reaction can occur earlier and appear more aggressive in children than in adults.
- Associated soft-tissue mass is uncommon in benign tumors.
The rare exceptions are ABC and GCT.
It is frequently seen with both osteosarcoma and Ewing sarcoma,
but it is much more in Ewing sarcoma,
which may aid in differentiating between them.
- Peritumoral oedema can be misleading,
as it can be seen in both benign and malignant lesions du to pathologic fractures.
In most cases,
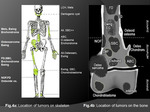
the differential diagnosis of a bone lesion can be narrowed based on knowledge of the age of the patient ( Fig. 3) and the location of the lesion [within the Skeleton and within a bone] (Fig. 4 a,b).
In addition,
matrix type can help narrow the differential diagnosis.
It depends on the material produced by the mesenchymal cells of the tumor.
The most common types are chondroid and Osteoid matrix.