Keywords:
Oncology, Pelvis, Abdomen, MR, MR-Diffusion/Perfusion, Computer Applications-Detection, diagnosis, Staging, Treatment effects, Neoplasia, Outcomes, Biological effects
Authors:
F. Landolfi, F. Coi, I. Martini, M. F. Osti, E. Pilozzi, M. Ferri, A. Laghi, E. Iannicelli; Rome/IT
DOI:
10.26044/ecr2019/C-2321
Results
-
At pathological evaluation,
tumor response was as follows:
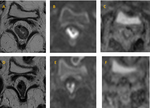
-TRG 1: 18/66 patients (27,3%) (Fig.3)
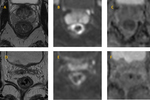
-TRG 2: 11/66 patients (16,7%) (Fig.4)
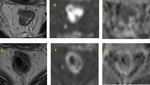
-TRG 3: 15/66 patients (22,7%) (Fig.5)
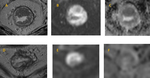
-TRG 4: 19/66 patients (28,8%) (Fig.6)
-TRG 5: 3/66 patients (4,5%) (Fig.7)
Histopathologic good responders and poor-responders included 29 patients (44%) and 23 patients (56%),
respectively.
Non-CR patients were 48/66,
accounting for 72,7%.
Table 3 shows patients distribution.
-
The correlation between MR-TRG and TRG resulted validated and significant with a ρ = 0.766 and a p value <0.001,
indicative of direct linear correlation.
By qualitative analysis,
good responders were correctly identified in 76% of cases,
poor responders in 95%.
CR were identified in 56% of cases.
-
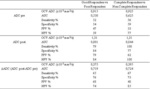
Before neoadjuvant CRT,
the mean ADC values of good- responders group (0,928 ± 0,151x10-3 mm2/s) were higher than those of poor-responders group (0.898 ±0.129 x10-3 mm2/s),
although the difference was not statistically significant (p = 0.454).
When a pre-CRT ADC value of 0,915 x10-3 mm2/s was used as cut-off value for discriminating between good and poor responders,
the following diagnostic predictive values were observed: sensitivity,
52%; specificity,
54%; PPV,
47%; and NPV,
59%.
The prediction of the favorable responders showed poor accuracy (Az = 0.530).
-
After neoadjuvant CRT,
the mean ADC values of good-responders (1,399 ± 0,197 x10-3 mm2/s) were significantly higher than those of poor-responders (1,193 ± 0,220 x10-3 mm2/s) with a p value of 0,003.
When a post-CRT ADC value of 1.31 x10-3 mm2/s was used as cut-off value for discriminating between good and poor responders,
the following diagnostic predictive values were observed: sensitivity,
79%; specificity,
84%; PPV,
79%; and NPV,
84%.
The prediction of the favorable responders showed good accuracy (Az = 0.801).
-
The mean ΔADC in good responders and in poor-responders was 0.470 ± 0.246 x10-3 mm2/s and 0.295 ± 0.189 x10-3 mm2/s respectively.
The DADC resulted significantly higher in good-responders than in poor-responders (p = 0,007).
When a DADC value of 0.375 x10-3 mm2/s was used as cut-off value to evaluate the treatment response,
the following diagnostic predictive values were observed: sensitivity,
65%; specificity,
76%; PPV,
68%; and NPV,
74%.
The prediction of the favorable responders showed good accuracy (Az = 0.719)
-
Before neoadjuvant CRT,
the mean ADC values of CR group (0,963 ± 0,153x10-3 mm2/s) were higher than those of NON-CR group (0.875 ±0.122 x10-3 mm2/s),
although the difference was not statistically significant (p = 0.102).
When a pre-CRT ADC value of 0,925 x10-3 mm2/s was used as cut-off value for discriminating between CR and NON-CR patients,
the following diagnostic predictive values were observed: sensitivity,
56%; specificity,
59%; PPV,
33%; and NPV,
77%.
The prediction of the favorable responders showed poor accuracy (Az = 0.625).
-
After neoadjuvant CRT,
the mean ADC values of CR (1,453 ± 0,181 x10-3 mm2/s) were significantly higher than those of NON-CR (1,179 ± 0,121 x10-3 mm2/s) with a p value of 0,0009.
When a post-CRT ADC value of 1.31 x10-3 mm2/s was used as cut-off value for discriminating between CR and NON-CR patients,
the following diagnostic predictive values were observed: sensitivity,
100%; specificity,
77%; PPV,
62%; and NPV,
100%.
The prediction of the favorable responders showed good accuracy (Az = 0.844).
-
The mean ΔADC in CR and in NON-CR was 0.490 ± 0.233 x10-3 mm2/s and 0.303 ± 0.167 x10-3 mm2/s respectively.
The DADC resulted higher in CR than in NON-CR group although the difference was not statistically significant (p = 0,021).
When a DADC value of 0.395 x10-3 mm2/s was used as cut-off value to evaluate the treatment response,
the following diagnostic predictive values were observed: sensitivity,
67%; specificity,
73%; PPV,
48%; and NPV,
85%.
The prediction of the favorable responders showed good accuracy (Az = 0.724)
Table 4 and 5 summarize ADC values in good- and poor-responders and in CR and NON-CR patients,
and ROC curve analysis respectively.