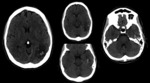
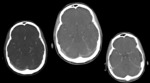
Unenhanced CT is often the most common initial imaging technique required by clinician for patients with new onset symptoms.
In unhenanced CT there are a few findings that can suggests CVST as the classical “cord-sign”,
the cordlike hyperattenuation within a dural sinus,
most commonly seen in the transverse sinus,
detectable in sinus or veins filled with thrombus as foci of hyperattenuation [5].
Evidence of venous infarcts,
with hemorrhagic components and significantly greater oedema than arterial infarction can support diagnostic hypothesis of CVST,
especially if infarcts are multiple and cross arterial boundaries [6].
Unfortunately unenhanced CT scans might even show subtle findings or appear normal.
Contrast enhanced CT (CECT) might help the diagnostic process of CVST with the detection of the “empty delta sign”,
a triangular area of enhancement or high attenuation with a relatively low-attenuating center on multiple contiguous transverse CT images,
obtained in the region of the superior sagittal sinus.
There are numerous hypotheses formulated to explain the pathophysiology of this sign: recanalization of the thrombus within the sinus,
blood-brain barrier breakdown,
organization of the clot,
dilatation of collateral peridural and dural venous channels but still there is not universal acceptance [7].
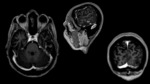
Magnetic resonance imaging (MRI),
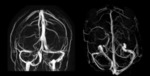
especially with MR venography,
constitutes a valid alternative or may be complementary to CT scan [8].
MR imaging may involve intravenous administration of contrast medium or non-invasive technique,
using 2D/3D TOF (time of flight) as well as 2D and 3D PC (phase contrast) techniques.
On conventional MRI sequences,
patent dural sinuses are often seen as a flow void,
in particular this is well visible when the imaging plane is orthogonal to the blood flow direction.
Although
reducing the effect of the flow void,
images acquired in a plane parallel to the dural sinus may offer a better depiction of the complete extent of the thrombosis within the sinus.
CVST remains a challenging diagnosis because thrombus and normal venous flow might have similar signal intensity,
depending on time since its formation.
In the acute phase thrombus appears isointense to surrounding brain tissue in T1-weighted images,
while in T2-weighted images it exhibits hypointense signal due to the presence of deoxyhemoglobin,
which may be misinterpreted as normal blood flow within the sinus.
In the subacute phase there is a change in signal intensity,
due to deoxyhemoglobin conversion to methemoglobin,
which explains why the thrombus becomes hyperintense first in T1-weighted and then in T2-weighted images.
This picture,
which may last from 5 to 30 days,
starts the chronic phase,
where a persistent thrombus is isointense in T1-weighted and hyperintense in T2-weighted images,
with a potential heterogeneous signal intensity due to a recanalization of the thrombus [9].
False-negative interpretations of CVST imaging in many cases are not related to misinterpretation of findings that clearly indicate abnormal flow,
on the other hand misinterpretations are often due to lack of specific attention to the appearance of the dural sinuses.
First reason is that the dural sinuses are frequently located on the edges of the image rather than in central portion and that images of the superior sagittal sinus are at the end of the series of the images reviewed by radiologists.
Moreover there are few mimics that can make the diagnosis of CVST still particularly challenging for radiologists both in CT and MRI [10].
On unenhanced CT scan a mimic of thrombosis is hyperdense blood in a patent dural sinus.
This finding may be seen in children,
particularly neonates,
in patients suffering from polycythemia or dehydration with a hemoconcentration of the blood.
Hyperdense blood may be difficult to differentiate from true dural venous thrombosis,
but symmetry of involvement,
homogeneity of the hyperdensity,
and involvement of virtually all venous structures including dural sinuses,
should support radiologists to exclude CVST hypothesis [6].
Even subdural hematoma may sometimes mimic CVST,
but it is worth remembering that the abnormal signal of the subdural hematoma is located more medial than the expected location of the transverse sinus [6].
More rare conditions are retained contrast material from previous radiologic examinations due to severely slow flow,
and slow flow related to ligation of the internal jugular vein: an accurate anamnesis and a contrast-enhanced study should be performed to clarify these findings [6].
Contrast enhanced CT scan and MR venography are definitively less susceptible to misinterpretations,
but among the causes of false-positive CVST,
we can include normal variant structures located within a dural sinus,
such as fenestrations and arachnoid granulations.
Fibrotic bands,
intrasinus septa or fenestrated dural sinus may manifest as false-positive linear filling defects mimicking for example an “empty delta sign” on CECT and are visualized more frequently on contrast-enhanced MR venography than on TOF MR venography [11].
Arachnoid granulations,
also known as Pacchioni granulations,
are isodense to CSF,
typically occuring next to the entrance of a superficial draining cortical vein into a sinus.
The arachnoid granulations are usually round and they increase in size and number with age,
visible in approximately two-thirds of patients,
most frequently with the transverse and superior sagittal sinuses.
On images showing the short axis of a dural sinus,
arachnoid granulations can be mistaken for thrombus,
especially if giant and in case they fill most of the lumen diameter,
but on images showing the long axis of the dural sinus they can easily be distinguished by their round shape.
Variations in the size of the dural sinuses is another anatomic cause of false-positive findings for CVST on MR venography [11].
An asymmetric appearance due to hypoplasia or aplasia of one of the transverse sinuses is described in literature in up to 25% of healthy patients on time-of-flight (TOF) venography and this condition might be often associated with persistent occipital sinus and mastoid emissary veins.
The occipital venous network in normal conditions tends to involve with age and more than 50% of the occipital sinuses were seen in children less than 25 months of age.
Persistence of occipital sinus has been reported to be present in 10% of normal brains on MR venography and its main anatomical variants are duplication,
rudimentary or absent ipsilateral lateral sinus and an occipital sinus draining only into the bulb of the left lateral sinus.
In case there is a drainage by the occipital sinus into the sigmoid one,
the occipital sinus may be termed the oblique occipital sinus [12].
Artifacts related to flow and to specific MR venography techniques can also cause signal loss mimicking CVST.
In TOF venography,
flow parallel to the plane of acquisition can produce signal loss due to saturation of signal from inflowing protons,
causing artifactual intravascular signal voids.
These can become most apparent in vertically oriented structures,
such as the distal sigmoid sinus and internal jugular veins,
since acquisitions in TOF venography are most commonly performed in the coronal plane [10].
Lastly on the suspicion of CVST,
the acquisition of TOF MR venography can produce a false negative finding: thrombus with methemoglobin may show hyperintensity on unenhanced T1-weighted images so its signal can simulate flow within the dural sinus.
If in doubt,
phase contrast venography can be performed to clarify this finding [10].