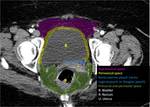
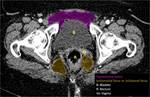
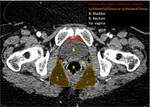
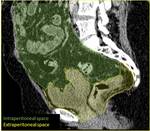
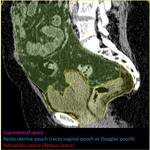
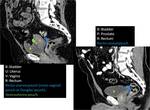
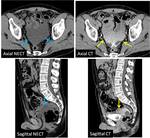
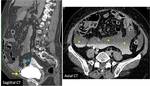
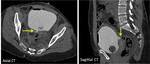
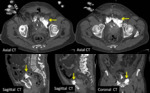
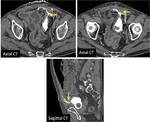
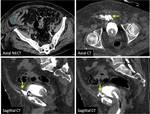
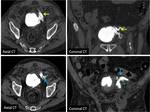
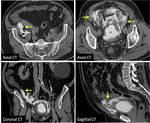
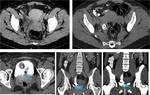
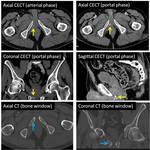
The radiologist should be familiarized with anatomical spaces and structures in order to make a good approach to bladder injuries (Fig 1,
2,
3,
4,
5 and 6).
There are several classifications for bladder injuries.
We have chosen those which we consider more useful.
Classifications:
Bladder injuries are usually classified by AAS scale [6] based on surgical findings:
- Type 1: bladder contusion.
- Type 2: extraperitoneal laceration <2 cm.
- Type 3: extraperitoneal laceration > 2 cm and intraperitoneal laceration <2 cm.
- Type 4: Intraperitoneal laceration >2 cm.
- Type 5: Combined lesion.
Imaging-based classification [3,
8]:
- Type 1: bladder contusion à conservative management with Foley catheter.
- Type 2: intraperitoneal rupture à surgical repair.
- Type 3: interstitial bladder injury à conservative management with Foley catheter.
- Type 4: extraperitoneal rupture à surgical treatment in complicated cases or after conservative management without adequate response.
Type 4a: simple extraperitoneal rupture
Type 4b: complex extraperitoneal rupture.
- Type 5: combined bladder injury à surgical repair.
Societe Internationale D´Urologie classifies bladder injuries in four types without taking into account the length of the bladder wall laceration: type 1,
contusion,
type 2,
intraperitoneal rupture,
type 3,
extraperitoneal rupture and type 4 combined lesion [4,
6].
Bladder contusion:
It is a mucosal injury with hematoma within the bladder wall with no findings in imaging studies [3,
5,
6,
8],
sometimes focal wall thickening can be detected [8].
Its management is conservative [3,
5].
Intraperitoneal rupture (Fig.
7 and 8):
Represents 10-30% of cases [1,
3,
4,
5,
6,
8] and they are typically associated with blunt rupture [2].
Management is mainly surgical [1,
2,
3,
5,
8] although in some cases of small iatrogenic lesions can be managed with only drainage if there are no clinical complications [2].
It occurs when bladder dome injury happens that is the weakest part of the bladder [1,
3,
4,
6,
8] and there is a communication between bladder and peritoneal cavity so extravasated contrast solution may be seen in paracolic gutters,
around bowel loops and in rectovesical and rectouterine pouch [1,
3,
4,
8].
Extravasated contrast will be seen less concentrated than in extraperitoneal injuries [1].
Interstitial injury:
Rare type.
It may be seen as a partial thickness of the wall without disruption of it [8].
Extraperitoneal rupture (fig.
9,
10,
11,
12,
13 and 14):
The most frequent type being the 80-90% of cases [1,
3,
4,
5,
6,
8],
60% of them are related with pelvic fracture [2,
6,
8].
They can be classified in [1,
2,
6]:
· Simple (extravasated contrast solution is limited to perivesical space [1,
3,
4,
8],
molar tooth sign [1,
6],
and are managed with urethral catheter drainage [2,
3,
5,
11]).
· Complex (extravasated contrast solution extends further,
to abdominal wall,
perineum or scrotum [1,
3,
4,
6,
8,
11] and dissect fascial planes and spaces.
They are usually associated with other fractures or organ lesions and early surgical repair is mandatory [2]).
Combined injury:
Represent 5-12% of cases [2,
3,
4,
5,
6,
8] and is managed with surgical repair [3,
5].
CT findings are a combination of those findings of extraperitoneal and intraperitoneal types.
Clinically it presents with gross hematuria or microhematuria,
suprapubic tenderness,
peritonitis (predominating in intraperitoneal bladder injury) and difficulty voiding [2].
Diagnosis should be made with clinical suspicion although definitive diagnosis requires exploratory laparotomy or by imaging.
CT cystography has replaced conventional cystography as it allows multiplanar reconstructions to identify the site of rupture [1,
5,
9] differentiating between intraperitoneal or extraperitoneal rupture and a complete study of the abdominopelvic region in patients with abdominal trauma [1].
Indications for CT cystography:
Clinical suspicion before CT:
o Absolute: gross hematuria with pelvic fracture [6,
12].
o Relative:
- Gross hematuria without pelvic fracture [6,
8,
12].
- Microhematuria with pelvic fracture [6,
12].
- Isolated high level microhaematuria (> 25 RBC/HPC) [6,
7,
8,
12].
- Pelvic fracture,
other than acetabular fracture [7].
o Others:
- Clinical suspicion: suprapubic pain,
voiding difficulties [6] and decreased urine output [13].
- Clinically detected blood in the meatus [5].
- Severe pelvic trauma [3].
After abdominal CT:
o Unexplained ascites [1,
5,
8].
o Ascites in association with pelvic fracture [1,
8].
o Pelvic hematoma [1,
7].
o Abnormal location of a Foley catheter [1].
o A defect in an enhancing bladder wall [1].
o Perivesical unusual gas collection [1,
13].
CT cystography is not mandatory in patients with microhematuria (<25 RBC/HPC) without pelvic fracture,
with isolated acetabular fracture associated or with no pelvic fluid [7].
Technique:
It is important an adequate technique to avoid misdiagnosis:
1º Non- enhanced CT (NECT) of pelvis region.
2º Routine abdominopelvic contrast-enhanced (CECT) (before or after CT cystography)[6].
3º Asses urethral integrity before inserting a Foley catheter [4]
4º Retrograde passive filling of the bladder via Foley catheter using low-gravidity drip infusion at 50-150 cm [5,7,9] with at least 350-400 ml of dilute water-soluble contrast media to prevent artifacts [1,
3,
6].
The dilution ratio of 1:10 is often used [14].
5º Clamp the catheter in order to maintain bladder distention [1].
6º CT of the pelvic region.
It is important to stand out that antegrade filling of the bladder with excreted intravenous contrast is not enough to bladder injuries diagnosis [2,
6,
8].
Post-drainage CT is not mandatory [3,
6,
7,
8,
13].
The absence of pelvis ascites almost discards bladder rupture [6,
13].
Contrast extravasation in spontaneous bladder rupture is only seen in 74% of the patients so other indirect signs may be helpful to diagnose it like unexplained pneumoperitoneum (without gastrointestinal pathology,
recent surgical history or pneumomediastinum) or ascites so accuracy increases to 95% [13].
Differential diagnosis:
- Injury to genitourinary tract [1] (Fig.
15).
- Traumatic rupture of pelvic viscera [1] (Fig.
16).