1.
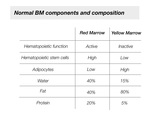
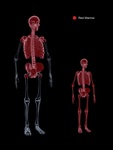
Normal BM components and composition
BM consists of hematopoietic stem cells,
adipose cells,
and stroma[1].
Normal BM is composed of both red and yellow marrow,
which contains different levels of predominant components[2].
Red marrow is considered hematopoietically active.
It contains a high level of hematopoietic stem cells.
It is composed of 40% water,
40% fat,
and 20% protein[3].
Yellow marrow is considered hematopoietically inactive.
It is composed of a high number of adipocytes and low level of hematopoietic stem cells.
It contains 80% fat,
15% water,
and 5 % protein[3].Fig. 1
2.
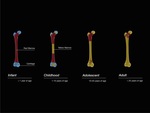
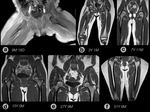
Physiologic BM conversion
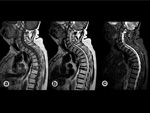
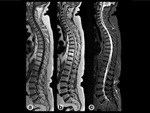
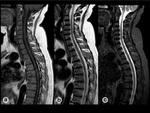
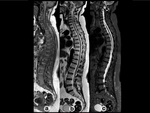
Neonates show almost entirely red marrow.
Over time,
yellow marrow conversion process takes place with a characteristic sequence as shown in Fig. 2, Fig. 3,
and Fig. 4.
Adult pattern is reached approximately at 25 years of age when red marrow persists in the axial skeleton and proximal metaphyses of long bones.
Axial skeleton BM conversion occurs gradually during adulthood with variable patterns[4].Fig. 5
3. Normal MRI signal
Due to the different fat and water amount,
yellow and red marrow display different MRI signal.
As a matter of fact,
water and fat have distinct chemical structures which explain their different magnetic properties.
3.1. T1-weighted Fast Spin Echo (FSE)
T1-relaxation time is a measure of how quickly the signal recovers to its initial value after the radiofrequency pulse has been applied.Fig. 6 Each tissue possesses different T1 relaxation time: fat value is shorter than those of water.Fig. 7
Due to the different fat amount,
yellow and red marrow display distinct T1-weighted FSE signal.
Yellow marrow appears hyperintense; red marrow appears slightly hyperintense.Fig. 8
Comparing BM signal intensity to muscle and intervertebral disc signal intensity is crucial: both normal yellow and red marrow display higher signal intensity than muscle and intervertebral disc[2].
3.2. T2-weighted Fast Spin Echo (FSE)
T2-relaxation time is a measure of how quickly spinning dipoles diphase after the radiofrequency pulse has been applied.
It refers to the progressive decay of the vector magnetization of transverse component following the radiofrequency pulse.Fig. 9
T2-weighted FSE is characterized by low contrast between yellow and red marrow.
The conjunction use of a fat suppression technique improves signal intensity contrast.Fig. 8
3.3. Short Tau Inversion Recovery (STIR)
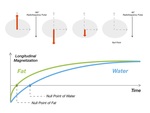
Fat signal suppression is based on tissues differences in T1-relaxation time value.
Because fat and water recover the longitudinal magnetization with different velocity,
they have a different null point.
When a 90° radiofrequency pulse is applied at the null point of fat,
the fat signal only is suppressed[5].Fig. 10
Due to the different water amount,
yellow and red marrow show distinct STIR signal.
Red marrow appears hyper-/iso-intense and yellow marrow appears hypo-/iso-intense.Fig. 8
The advantage is that STIR is insensitive to magnetic field inhomogeneities.
The disadvantage is that fat suppression is nonspecific because radiofrequency pulse suppresses all substances with a similar null point[5].
3.4.
Spectral Fat Saturation
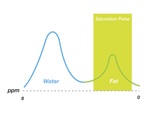
Fat saturation technique exploits the chemical shift.
Chemical shift consists of different precessional frequencies of fat and water[5].
During fat saturation acquisition,
a radiofrequency pulse with the same fat resonance frequency is applied to excite it.
Immediately after the radiofrequency pulse,
a spoiling gradient pulse is applied to cause the fat signal decay to zero[7].Fig. 11
Spectral fat saturation techniques provide fat suppression without disturbance of non-adipose tissues signal.
Furthermore,
it can be used after the administration of contrast media.
Unfortunately,
inhomogeneities of the static magnetic field do not allow a homogeneous fat suppression[5].
3.5.
Dixon
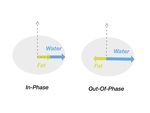
Because of fat and water different precessional frequencies,
tissues are periodically out of phase with each other.
In-phase images are acquired when fat and water protons are in phase.
Out-of-phase images are acquired when fat and water protons are out of phase.Fig. 12 The fat signal is suppressed at post-processing and not during the acquisition.Fig. 13
Acquisition time is faster than other techniques and it is independent by local magnetic field inhomogeneity.
Compared to STIR,
Dixon technique provides a higher signal-to-noise ratio.
Dixon has the disadvantage to be sensitive to metal artifacts and main magnetic field inhomogeneities[8].
T2-weighted Dixon SE fat images have been proposed as an alternative protocol to T1-weighted SE images in bone marrow metastases detection[9].
3.6.
Diffusion-weighted MR Imaging (DWI-MRI)
DWI-MRI is a technique that measures the Brownian motion of water molecules,
which is decreased in highly cellular tissues such as malignancies.
Tissues with diffusion restriction appear hyperintense in isotropic diffusion map with high b-values and hypointense in apparent diffusion coefficient map.
Its use in BM evaluation is controversial because of the large variability results in the previous studies[10].
3.7.
Contrast-enhanced imaging
Administration of gadolinium-based contrast agents does not give additional information in distinguish lesions,
so it is not routinely used[11].
A new class of contrast media,
the ultra small superparamagnetic iron oxide particles (USPIO),
was recently described but,
currently,
they are not approved by the Food and Drug Administration.
USPIO is phagocytosed by macrophages in the normal BM causing a hypointense signal in T2w images; moreover,
USPIO particles are not taken up in neoplastic lesions,
which appear relatively hiperintense[12].
4.
MRI aspect of BM variants
BM is usually characterized by normal heterogeneity that may be confused with malignant lesions.
4.1.
Yellow Marrow Islands
Variation of bone marrow conversion which consists of focal areas of normal yellow marrow.
MRI signal is the same of normal yellow marrow.
4.2.
Red Marrow Islands
Focal areas of normal red marrow which show poorly defined margins and symmetrical distribution.
T1w signal intensity is slightly higher than muscle and intervertebral disc signal whit no increase in fat-suppressed images.
4.3.
Diffuse hematopoietic marrow hyperplasia
In adult age,
yellow marrow can reconvert to red marrow in benign conditions following the reverse sequence of physiologic conversion[13].
T1w signal is slightly higher than the muscle signal.
Furthermore,
compared to pathologic marrow infiltration,
diffuse hematopoietic marrow hyperplasia has a symmetric distribution.
4.4.
Premature BM conversion
In healthy patients,
it must be considered as a normal variation.
Nevertheless,
it is necessary to exclude hormonal disorders[11].
5.
MRI findings of BM disorders
BM disorders may be benign or malignant.Fig. 14
5.1.
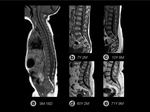
BM reconversion
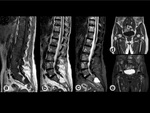
BM reconversion consists of yellow marrow substitution with red marrow following the reverse sequence of physiologic conversion.
Reconversion occurs in case of increased demand for hematopoiesis. The previous described diffuse hematopoietic marrow hyperplasia arouses with the same mechanism under benign stimuli.
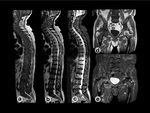
Signal intensity in T1w is slightly higher than that of muscle.Fig. 15, Fig. 16,
and Fig. 17.
5.2.
BM infiltrative disorders
In BM infiltrative disorders the hematopoietic cells develop and reproduce excessively.
Multiple myeloma,
the most common primary bone tumor,
is characterized by multiple focal lesions which are hypointense in T1w images; the T2w signal is variable.
It can be indistinguishable from metastases.Fig. 18
Leukemia causes diffuse BM infiltration from malignant cells,
that appears hypointense in T1w images and variable signal in T2w images.
Because of the diffuse distribution,
the signal alteration can be missed if it is not compared to normal muscle and intervertebral disc signal[14].
5.3.
BM replacement disorders
BM is replaced by benign or malignant cells that do not arise from normally existing marrow elements.
Osteomyelitis is a benign disease in which BM is replaced by inflammatory cells.
It appears hypointense in T1w images,
hyperintense in T2w and STIR images.
Penumbra sign can be found in T1w images when an abscess cavity in present: hypointensity surrounded by a stronger hypointense rim caused by reactive new bone formation or edema[14].
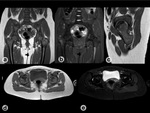
Metastases are the most common bone marrow malignant lesions.
All metastatic lesions generally have T1w hypointense signal,
with the exception of lesions from lung cancer that sometimes show hyperintense signal[15]. T2w signal is variable: lesions from stomach cancer are iso-/hypointense; colorectal cancer and HCC are hyperintense; lung and breast cancer do not have a definite tendency[15].Fig. 19 The most difficult question to answer is the differentiation between pathologic and stress fracture.
Usually,
when there are well defined T1w hypointense signal around the fracture,
endosteal scalloping,
and adjacent muscle signal abnormality,
the fracture is pathologic[16].
Other features in favor of a pathologic fracture at the level of the spine are the diffuse involvement of a vertebral body,
the involvement of the pedicle or posterior elements,
and multiple other metastatic lesions[17].Fig. 20
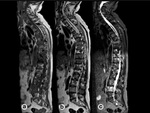
Lymphoma shows similar appearance as metastatic lesions.
It can be focal or diffuse and its signal is hypointense in both T1w and T2w images.
BM replacement is more frequent in non-Hodgkin lymphoma than in Hodgkin disease; its involvement is used to assess prognosis and therapy[18].Fig. 21 and Fig. 22.
5.3.
BM depletion disorders
BM loses areas of normal red marrow and it is totally replaced by yellow marrow.
Radiotherapy is responsible for different signals according to therapy timing.Fig. 23 BM regeneration timing is variable and depends on patient years of age and radiation dose; in any case,
it occurs within 12 months[18].Fig. 24,Fig. 25,Fig. 26,
and Fig. 27.
Chemotherapy induces different MR signal according to therapy timing.Fig. 28 After chemotherapy,
BM depletion results in red marrow replacement by yellow marrow[18].Fig. 29 and Fig. 30.
Aplastic anemia is a rare disorder characterized by anemia,
pancytopenia and BM hypocellularity.
It can be inherited (Fanconi anemia),
acquired (toxins,
medications,
infection,
chemotherapy,
and radiotherapy) and idiopathic.
BM hyperintensity in both T1w and T2w images is due to BM replacement by yellow marrow.
5.4.
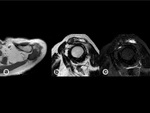
BM ischemia
BM ischemia is due to microvascular occlusion,
intraosseous pressure,
chemotherapy,
and steroids.
Ischemia causes cell death and subsequent inflammatory and reparative response: BM signal is hypointense in T1w images and hyperintense in T2w images.
Double line sign is typical on T2w images: a curvilinear hypointense line,
which corresponds to the necrotic bone,
surrounded by a hyperintense band,
which is the inflammatory and reparative tissue[14].Fig. 17
5.5.
BM edema
BM edema is unspecific: it can be caused by trauma,
infection,
inflammatory diseases,
ischemia,
nearby neoplasia or it can be secondary to systemic diseases such as hyperparathyroidism or renal osteodystrophy.
BM edema appears hypointense in T1w images and hyperintense in T2w and STIR images[14].Fig. 20
5.6.
Storage diseases
Gaucher’s disease and iron storage pathologies are the most common.
Gauche’s disease is characterized by decreased levels of glucocerebrosidase,
which results in glucocerebrosides accumulation within histiocytes.
BM involvement consists of cellular necrosis,
fibrous proliferation and loss of spongy trabeculae.
Signal intensity is low in T1w images and high in T2w images[4].
Iron storage in BM occurs in erythrocytes destruction (i.e.
thalassemia),
iron overload (i.e.
transfusion therapy),
abnormal iron absorption (hemochromatosis).
BM is hypointense in both T1w and T2w images[4].