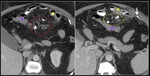
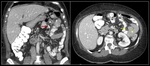
Computed tomography (CT) remains the imaging modality of choice for diagnosing IH.
The LRYGB is a procedure which modifies the gastrointestinal tract anatomy,
making its recognition troublesome sometimes and implying a considerable interobserver variability. For that reason,
holding a heightened awareness and understanding of the altered anatomy and the typical CT signs of IH are important to prevent a diagnosis delay with subsequent increase morbidity and mortality.
A) LRYGB MODIFIED ANATOMY
The LRYGB consists of creating two limbs.
The first one implies the gastric pouch, which is the lesser gastric curvature,
isolated and linked to a loop of jejunum called the Roux or alimentary limb,
creating a side-to-side gastrojejunostomy.
This limb can be placed retrocolic,
through an opening created in the transverse mesocolon,
or antecolic,
in front of it.
The other one is called biliopancreatic limb and it is composed of the excluded stomach the duodenum and the proximal jejunum (Fig. 2).
Finally,
a jejunojejunostomy is created at approximately 30cm from the Treitz’s angle,
joining the Roux limb and the biliopancreatic limb (Fig. 3).
B) INTERNAL HERNIAS CT SIGNS
Several CT findings suggesting IH have been typically described:
- Mesentery swirl sign
- Mushroom sign
- Clustered loops
- Small bowel behind the superior mesentery artery
- Small bowel obstruction
- Hurricane eye sign
- Right-sided jejuno-jejunal anastomosis
In order to illustrate these signs,
we reviewed the bariatric surgery database of the University Hospital Morales Meseguer (Murcia,
Spain) from 1997 to 2017 (503 patients),
so as to identify patients with an IH diagnosed at re-laparotomy and with a preoperative multidetector CT (8 patients).
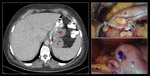
CASE 1 (Fig. 4)
LRYGB with intermittent postprandial abdominal pain and sweating in the last three months.
Normal gastroscopy and Upper GI Series.
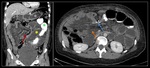
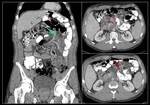
Coronal (A) and axial (B) images of MDCT with oral and intravenous contrast show dilation of the Roux limb (green asterisk) near distal jejunojejunal anastomosis, with normal caliper of the biliopancreatic (yellow asterisk) limbs. Abnormal right-sided position of the proximal aspect of biliopancreatic limb (pink arrow) and jejunojejunal intussusception (red arrow).
Surgical diagnosis: Petersen IH.
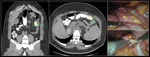
CASE 2 (Fig. 5)
LRYGB with colic intermittent postprandial abdominal pain.
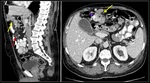
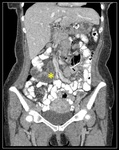
Coronal-4.8 mm maximum intensity projection (MIP) reconstruction (A) and axial (B) MDCT images with oral and intravenous contrast, show an upper-left quadrant herniation of Roux limb and its mesentery through the Petersen’s space.
Coronal MIP nicely evidences mushroom-shaped cluster of herniated small intestine loops (red dashed lines) located in the subphrenic space (green asterisk).
Surgical diagnosis: Petersen IH.
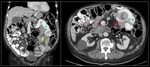
CASE 3 (Fig. 6)
LRYGB patient with acute back-irradiated abdominal pain and neutrophilia.
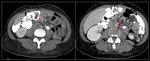
Coronal (A) and axial (B) images of abdominal CT with oral and intravenous contrast showing dilatation of the excluded stomach (purple asterisk),
the alimentary (green asterisk) and biliopancreatic (yellow asterisk) limbs,
having an abrupt change of caliper just next to the jejunojejunal anastomosis, suggesting SBO.
"Swirled" appearance of the mesentery vessels (red arrow) and herniation of some non-dilated loops to the right hemiabdomen (orange arrow) through the jejunojejunostomy (blue arrow).
Surgical diagnosis: jejunojejunal internal hernia.
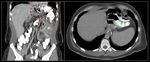
CASE 4 (Fig. 7)
LRYGB with intermittent abdominal pain and episodes with nausea and vomiting.
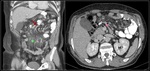
Sagittal (A) and axial (B) MDCT images with oral and intravenous contrast,
show the abnormal location of small bowel loops (yellow arrow) at the right-upper-quadrant between the transverse colon (purple asterisk) and anterior abdominal wall (white asterisk),
suggesting transmesenteric IH.
The mesentery vessels are a bit "swirled" as well (red arrow).
Surgical diagnosis: IH.
CASE 5 (Fig. 8)
LRYGB with worsening of intermittent chronic abdominal pain.
Axial images (A,
B) MDCT with oral and intravenous contrast show an anterior and right displacement of the Treitz angle (pink asterisk) and a "swirled" appearance of the adjacent mesenteric vessels (red arrow) suggesting a Petersen’s internal hernia.
The radiological diagnosis was confirmed at surgery.
CASE 6 (Fig. 9)
LRYGB with acute abdominal pain,
profuse sweating and absence of gas expulsion.
Coronal soft-tissue VR reconstruction (A) and axial (B) MDCT images with oral and intravenous contrast,
show swirled mesentery vessels (red arrow),
small bowel mesentery edema (green asterisk),
and right displacement of the Treitz angle (pink asterisk).
Surgical diagnosis: Petersen's IH.
CASE 7 (Fig. 10)
LRYGB with left acute abdominal pain and peritoneal tenderness.
Coronal (left) and axial (right) MDCT images with oral and intravenous contrast showing an ingurgitation of the small bowel mesentery vessels and edema (green arrow), as far as swirled mesentery vessels and enlarged lymph nodes (red arrow) located in the left hemiabdomen.
There is also a right displacement of the Treitz’s angle (pink asterisk).
Surgical diagnosis: Petersen's IH.
CASE 8 (Fig. 11)
LRYGB patient high clinical suspicion of IH.
Coronal image of an abdominal CT with oral and intravenous contrast showing a right displacement of the biliopancreatic loop (yellow asterisk),
with no dilation nor other signs.
Surgical diagnosis: Petersen's IH.
C) MESENTERY DEFECTS CLOSURE IN LRYGB
A recent meta-analysis concludes that an antecolic route of the Roux limb and the closure of mesenteric and/or mesocolonic defects (Fig. 12 and Fig. 13) have the lowest internal herniation incidence following LRYGB (1%; P<0,001).
However,
mesenteric defect closure (MDC) at the time of primary surgery does not eliminate the incidence of IH.
Current controversy exists regarding MDC in surgical literature.
Two ongoing randomized clinical trials are evaluating various techniques of closure (running non-absorbable suture or staple device vs leaving defects open) with adequate length and quality follow-up,
in order to reach consensus on the preferred method of closure.
We have collected from our bariatric surgery database all the patients with both primary closed and stapled Petersen’s space and jejunojejunostomy, performed in our hospital since 2015,
whom a CT scan was requested to rule out some gastrointestinal complications.
We have selected three of them in order to illustrate the location of the staples. Until now,
no IHs have been clearly demonstrated in those patients.
PATIENT 1 (Fig. 14)
Seventh post-operative day in a LRYGB patient with acute abdominal pain.
MDCT in axial,
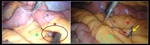
coronal and sagittal planes shows the staples at the Petersen's space (yellow asterisk: alimentary limb; purple asterisk: transverse colon),
and posterior to the jejunojejunal space (red arrowhead). Sagital-MPR (D) nicely displays the stapled-MDC tracking the space between the transverse colon and the alimentary limb (yellow arrowheads) - the Petersen's space.
PATIENT 2 (Fig. 15)
Fifth post-operative day LRYGB with fever and epigastric pain.
MDCT axial images.
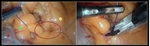
The red hollow circle surrounding staples at the root of the mesentery between transverse colon (purple asterisk) and Roux limb (yellow asterisk).
The yellow hollow circle shows mesenteric closure at jejunojejunal anastomosis.
Gastrojejunal anastomotic leak (not shown) was depicted,
which was entirely collected by surgical drainage (white arrow).
PATIENT 3 (Fig. 16)
Twelfth post-operative month LRYGB with colic abdominal pain.
Coronal MPR and axial MDCT images show staples placed at Petersen’s space (note the close relationship to the middle colic vein - red arrow) and,
at a cranial level,
metallic landmarks at jejunojejunal mesentery.
Some false-positive findings were reported in this patient.
Namely,
a grouping of non-dilated biliopancreatic loop (yellow asterisk) and a round appearance of distal mesenteric fat (hurricane eye sign) (yellow arrow) were suggested as indirect signs of IH.
At surgery,
a partially opened and empty Petersen’s space was fixed, jejunojejunal space was normal and some adhesions between the alimentary limb and distal anastomosis were released.
This patient experienced remission of complaints after the procedure.