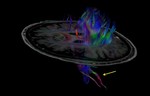
DATscan is a valuable tool for evaluating patients with parkinsonian symptoms.
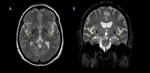
Normal DATscan shows two symmetric crescent shaped regions (comma).
DATscan is normal in essential tremor or drug induced parkinsonian symptoms,
because these disorders are not related to nigro-striatal dopamine transporter loss.
PD and Pps have DAT degeneration,
which results in an abnormal DATscan .
However,
extensive overlapping in DATscan findings does not allow discrimination between PD and Pps [7].
Structural magnetic resonance imaging plays a crucial role in the diagnostic workup of neurodegenerative disorders.
MRI can rule out mimic conditions and can also detect typical features that support the clinical diagnosis.
Advances in MRI have enabled the mapping of structural and functional aspects of PD and Pps,
and have offered valuable clues,
aiding the differential diagnosis of these disorders [8].
This poster summarizes the most useful MRI findings in Parkinson’s disease and Parkinson Plus Syndromes,
focusing on conventional and advanced MRI techniques.
Parkinson’s disease
PD is the second most common neurodegenerative disorder after Alzheimer's disease and the most common cause of parkinsonism.
The definitive diagnosis of idiopathic PD requires the demonstration of intraneuronal Lewy body inclusions in the pars compacta of substantia nigra.
A diagnosis of probable PD can be formulated in vivo based on clinical evaluation when the typical triad of clinical symptoms and signs is present (bradykinesia,
tremor at rest and rigidity).
The high accuracy of clinical diagnosis of PD questions the use of radiotracer neuroimaging [7].
However,
MRI is useful in the diagnostic workup of PD,
in order to exclude the presence of causes of secondary parkinsonism,
and to differentiate PD from Pps [8].
Conventional MRI is often disappointing in the diagnosis of PD.
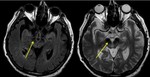
Narrowing of the pars compacta,
with delineated borders of red nucleus and substantia nigra on T2 images may support the diagnosis of PD (Fig 1).
Loss of normal signal of the substantia nigra may be seen on T1WI.
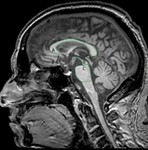
Mild midbrain volume loss with “butterfly” configuration can be observed in some advanced cares.
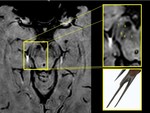
The swallow tail sign describes the normal axial imaging appearance of nigrosome-1 within the substantia nigra on high resolution SWI images (Fig 2).
Nigrosome-1,
is located in the caudal and posterolateral part of the substantia nigra pars compacta.
It is the largest dopamine-containing cluster and is mostly affected by PD.
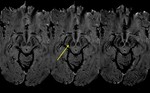
Absence of the swallow tail sign is reported to have a diagnostic accuracy of greater than 90% for PD (Fig 3).
[9]
Multiple system atrophy (MSA)
MSA is divided in three subtypes (MSA-P,
MSA-C,
MSA-A) which have some overlap both clinically and radiologically.
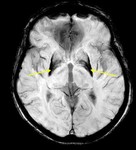
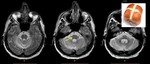
Small putamina with low signal intensity on T2*/SWI sequences due to high iron deposition is noticed in MSA-P patients (Fig 4).
Signal intensity is lower in the posterior putamen comparing with the posterior part of the globus pallidus.
Nonetheless,
iron deposition in the putamen continues in the elderly,
thus putaminal hypointensity may be a normal finding in individuals older than 80 years of age.
A T2/FLAIR hyperintense lateral rim is seen in patients with MSA-P,
on 1.5T (Fig 5),
however a thin,
smooth,
slit-like hyperintense line along the lateral putamina may be a normal finding on 3T.
MSA-C is characterized by pontine,
medulla,
and cerebellar atrophy (Fig 6).
Enlargement of the fourth ventricle may be seen.
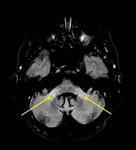
Middle cerebellar peduncles are small with a concave appearance and they may appear hyperintense on T2/FLAIR images (Fig 7).
T2/FLAIR sequences demonstrate a cruciform hyperintensity in the pons termed the "hot cross bun" sign (Fig 8).
Surface measurements in MSA-C confirm the pontine atrophy.
Elevated ADC is noticed in the pons,
middle cerebellar peduncles,
cerebellar white matter and dentate nuclei.
Decreased number of fiber bundles and reduced fractional anisotropy (FA) in the degenerated transverse pontocerebellar fibers are demonstrated by DTI (Fig 9).
Tractography may also reveal corticospinal tract involvement.
There are no specific MR findings for MSA-A [1,10].
Progressive Supranuclear Palsy (PSP)
PSP is the most common Pps.
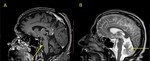
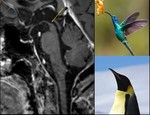
Sagittal T1 and T2 weighted images show midbrain atrophy with a concave upper surface (the "penguin" or "hummingbird" sign) (Fig 10).
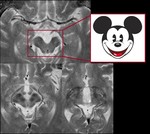
The quadrigeminal plate is thinned and the adjacent cisterns are enlarged (“mickey-mouse sign”) (Fig 11).
Moreover,
the superior cerebellar peduncles are thin and the third ventricle is enlarged [11].
Surface measurements in PSP patients reveal severe midbrain atrophy (Fig 12).
Pontine atrophy may be seen to a lesser extent.
Midbrain to pons area ration of less than 0.22 is an accurate finding in PSP,
which helps in the differential diagnosis from PD and MSA [12].
Reduced fractional anisotropy (FA) and increased ADC values are noticed in the midbrain and in the putamina.
Corticobasal Degeneration
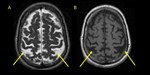
CBD is characterized by moderate but asymmetric frontoparietal atrophy.
Central,
precentral and postcentral gyri are most severely involved (Fig 13).
Atrophy is more pronounced contralateral to the side that is more severely affected clinically.
Striatum and midbrain tegmentum may also be affected.
T2 /FLAIR hyperintensity may be seen in the subcortical white matter of the perirolandic subcortical white matter.
MRI surface measurements in CBD patients reveal corpus callosum atrophy and mild midbrain atrophy.[1,12,13]