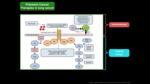
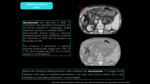
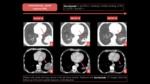
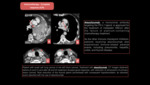
Precision therapy includes in lung cancer: targeted therapy and immunotherapy. Fig. 1
This therapy is different from conventional chemotherapy:
Traditional cytotoxic chemotherapies: destroy rapidly growing cells,
and act on the mechanism of cell division
Targeted drugs: are intended to interfere with specific aberrant molecular mechanisms involved in the development of tumors,
for example,
associated with tumor antiangiogenesis
Immunotherapy: uses immune system responses to treat cancer
Targeted drugs
The advantage of target drugs is to act more accurately and with fewer side effects
In general,
these drugs are classified into:
Immunotherapy
- Immunotherapy treatment response takes time.
- Inaccurate interpretation of response may lead to premature termination of therapy and removal from drug trial.
- Strategies for activating anti-tumor immunity.
- Include vaccines,
oncolytic viruses,
the transfer of activated T cells and NK ex vivo,
or administration of antibodies or recombinant proteins that stimulate or block so-called immune checkpoints.
- Immune Checkpoints are physiological inhibitory mechanisms in the immune system,
essential for the maintenance of "self-tolerance",
avoiding autoimmunity.
- Tumors have ability to activate immune checkpoints,
which is one of the most important mechanisms of immune resistance,
particularly inactivating T cells.
- CTLA4 and PD1 are receptors normally present in T cells which act inhibiting T cell activation.
These are mechanisms of tumor escape.
- Blocking these receptors with antibodies would prevent their binding to ligants,
preventing T cell inactivation and amplifying the antitumor action.
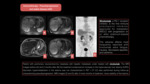
Immunotherapy - Immune response criteria
Need for new response criteria
- irRC 2009 (immune-related response criteria)
- irRECIST 2013 (immune-related RECIST)
- iRECIST mar/2017 (immune RECIST)Fig. 6
They all account for new patterns of response observed in immunotherapies
Immune response criteria - Seymour el al.
Lancet Oncol 2017;18,e143–e152
Key points
- New overall response called iUPD - immune unconfirmed progressive disease
- Resetting the bar if Progressive Disease (PD) is followed in the next time point by tumor shrinkage
Time point (TP) response
First RECIST 1.1 progressive disease (PD) is “unconfirmed” for iRECIST – iUPD.
Must be confirmed at the next assessment,
in 4 to 8 weeks.
After iUPD,
it’s possible to have:
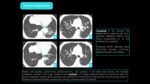
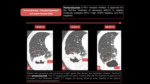
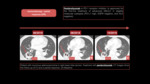
Immunotherapy- Particular effects: Abscopal effect
The abscopal effect refers to the ability of localized radiation to trigger systemic anti-tumor effects.
The abscopal effect has been connected to mechanisms involving the immune system.
However,
the effect is rare because at the time of treatment,
established immune-tolerance mechanisms may hamper the development of sufficiently robust abscopal responses.
Today,
the growing consensus is that combining radiotherapy with immunotherapy provides an opportunity to boost abscopal response rates,
extending the use of radiotherapy to treatment of both local and metastatic disease.