The thyroid ultrasound examination should be performed with a high frequency linear transducer,
usually between 10 and 14 MHz.
Multifrequency transducers allows a range of frequencies that can consequently determine a higher technical quality examination.
Lower frequency linear transducers (7 to 10 MHz),
as well as convex transducers,
are useful for evaluation of large glands (e.g.
goiter),
evaluation of large nodules, and to assessment of a thyroid that extends to the chest.
The device must be properly preset for thyroid assessment.
Color Doppler evaluation will require an initial adjustment that allows mapping arteries with systolic peak velocity about 15 cm/s.
Color Doppler gain must be adjusted as high as possible just before determining excessive noise artifacts. Wall filter should be as low as possible.
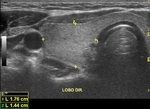
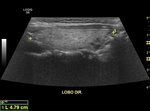
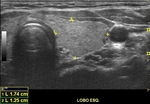
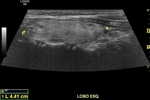
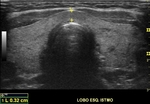
A normal ultrasound examination should include documentation of the left and right lobes,
and isthmus,
in two orthogonal planes (longitudinal and transverse).
Caliper positioning for measurements should be included in the documented images.
To be considered appropriate,
the images should include the entire extent of the gland.
The measurements and the glandular volume should be described in the report (normal standard: 5-15 cc).
It may be considered part of the exam the assessment of cervical ganglion chains searching for lymph node enlargements and micropoliadenopathy,
which may be associated with diffuse thyroid disease or tumors.
In the presence of suspicious nodules,
investigation of cervical lymph node involvement should be actively performed.
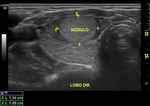
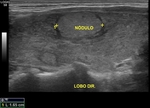
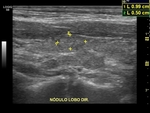
Focal lesions,
such solid or mixed nodules should be documented in at least two planes,
with measures of the three axes.
Dimensions,
composition,
contours,
echogenicity,
shape,
texture,
as well as the presence of sign of the peripheral halo or microcalcifications (when present) shall be documented.
Colloid cysts can be documented with less stringency,
due to their characteristic pattern,
always being careful not to confuse them with small mixed nodules.
Nodules with suspicious features of malignancy are: markedly hypoechogenic nodules, nodules with irregular and/or poorly defined contours,
nodules with microcalcifications in its interior and nodules with anteroposterior diameter greater than the transverse diameter.
The bigger the nodule,
more suspicious it becomes.
Patients with diffuse thyroid disease should have each thyroid lobe documented in at least two orthogonal planes,
demonstrating the contours,
texture,
echogenicity,
and any changes in glandular volume.
After B-mode evaluation,
we begin the Doppler evaluation which should contemplate three fundamental steps:
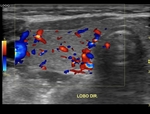
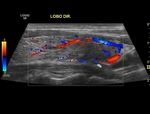
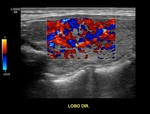
- STEP 1: Performing a color Doppler mapping: We must document left lobe and right lobe in orthogonal planes,
with color box activated.
The color box should wide enough to cover preferably the entire parenchyma or at least most part of the parenchyma. Pulse repetition frequency (PRF),
gain,
and wall filter settings should follow the recommended standardization.
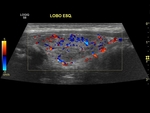
Normal parenchyma on Doppler can be defined when there is a mapping of the peripheral vessels and characterization of up to three internal vessels in each lobe.
A thyroid gland with vascular mapping notably above this pattern can be considered HYPERVASCULARIZED. Especialy if its associated with signs of diffuse thyroid disease.
Mappings markedly below this reference (too few or no flow characterization) are considered HYPOVASCULARIZED.
It is usually associated with signs of long term chronic diffuse thyroid disease, and reduction of glandular volume.
It is noteworthy that the marked increase in thyroid vascularization as known as "thyroid hell" is mostly but not exclusively associated with Graves' disease.
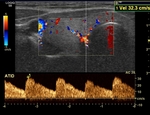
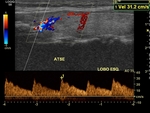
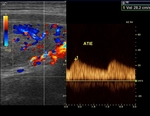
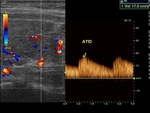
- STEP 2: Evaluation of the thyroid arteries: For this analysis,
we must search for the lower thyroid arteries (left and right),
or the superior thyroid arteries (left and right).
The lower thyroid artery can be assessed by longitudinal or transverse scan,
along the inner margin of each lobe,
on its lower or middle third, next to the trachea.
The superior thyroid artery can be assessed in a longitudinal scan,
near the upper pole of the thyroid.
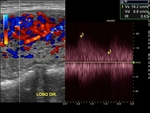
The sample of each thyroid artery for Doppler spectral analysis should be taken as close as possible to its entrance into the glandular parenchyma,
avoiding intra-parenchymal portion or its intraglandular branches.
Angular correction is mandatory for Doppler recording,
once we will estimate the systolic peak velocity.
There is great variability of the normal parameter of systolic peak velocity in the literature.
Values equal or lower than 30 cm/s can be considered normal.
Values above this reference are frequently seen in untreated thyroiditis, in patients refractory to instituted treatment,
or in patients treated with underdosed medications.
In patients adherent to treatement with adequate doses,
the systolic peak velocity of thyroid arteries usually reduces to normal or next to normal values.
Systolic peak velocities above 50 cm/s are more frequently associated with Graves' disease.
It is important to emphasize that the vascular mapping of the parenchyma does not show such an evident alteration of its expression even after the institution of adequate clinical therapy. The color Doppler mapping will change with the natural course of the disease,
eventually evolving to hypovascularization in the long term.
- STEP 3: To be performed only when the patient has thyroid nodules.
There is evidence that color Doppler patterns and elevated resistance index of arteries of the nodules can be associated with higher risk of malignancy besides the previously mentioned B mode sonographic characteristics.
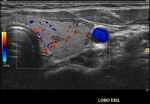
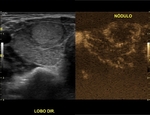
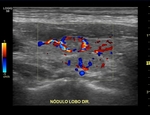
Chammas et al have described five distinct patterns of vascular characterization of thyroid nodules. A nodule should be mapped with color Doppler,
without compression by the transducer,
in the search for its vascular pattern,
classifying according to the list below:
- Chammas I: no detectable flow
- Chammas II: exclusively peripheral flow
- Chammas III: central and peripheral flow balanced or with peripheral predominance
- Chammas IV: central and peripheral flow,
predominating central flow
- Chammas V: exclusively central flow
Particularly the patterns Chammas IV and V were significantly associated with higher risk of malignancy.
These patterns are also associated with higher risk of malignancy in nodules with inconclusive cytologic patterns such as follicular neoplasms.
Patterns Chammas I and II in thyroid follicular neoplasms has high negative predictive values for malignancy.
Besides B mode documented images,
we recommend to document each nodule in at least two planes with color Doppler mapping,
using a color box large enough to encompass the entire nodule.
These images will demonstrate the absence or presence of flow,
and their distribution pattern.
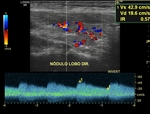
High resistance index (RI > 0,70) in thyroid nodules arteries has been associated with increased risk of malignancy.
In order to minimize large variability of the resistance index in different arteries of the same nodule it is recommended to take three samples for each nodule (three central samples in the Chammas V pattern,
three peripheral samples in the Chammas II,
and three samples including the peripheral and central flow in nodules with patterns Chammas III or IV).
The mean of the two higher resistance index is calculated for each nodule.
The table 1 is a purpose to associate B mode characteristics,
color Doppler patterns and resistance index discriminating if the nodule is of low risk or increased risk by a multiparametric analysis.
| ECHOGENICITY |
VASCULAR PATTERN |
UP TO 1.0 CM |
1.1 - 2.0 CM |
2.1 - 3.0 CM |
| Hypoechoic |
IV / V |
Any RI |
Any RI |
Any RI or vascular pattern |
| Hypoechoic |
II / III |
RI > 0.68 |
RI > 0.50 |
Any RI or vascular pattern |
| Nonhypoechoic |
IV / V |
RI > 0.82 |
RI > 0.65 |
RI > 0.46
|
| Nonhypoechoic |
II / III |
Low risk |
RI > 0.96 |
RI > 0.78
|
TABLE 1: Echogenicity,
vascular pattern,
width and RI (resistance index) of nodules at high risk for suspicious or malignant cytology
It is important to emphasize that all parameters should be analyzed together.
Suspected nodules present multiple risk variables,
with specific color Doppler patterns and higher resistance indices than benign nodules with the same Doppler characteristics.
The reviewed articles reinforce that color and spectral Doppler analysis DOES NOT SUBSTITUTE cytological or histological evaluation.
In fact,
the importance of the duplex-Doppler method lies on the fact that it helps screening nodules that deserve cytological evaluation potentially avoiding unnecessary punctures and reducing costs and burden of further investigation.
In patients with multiple nodules it allows to select which ones present risk that justify diagnostic puncture.
Doppler analysis can also help decision making of surgical removal or only surveillance of nodules with inconclusive cytological results.
In the presence of colloid pattern cysts,
we must assess the finding with the color mapping box in order to asses if there is no flow in its interior or in its periphery witch should rule out the possibility of a mixed nodule with a small peripheral solid component.
This hypothesis should be remembered whenever we suspect a colloid cyst,
and the color Doppler mapping may demonstrate peripheral vascularization foci,
helping in the differential diagnosis of these mixed nodules.
Regarding to the report,
we recommend that standards follow the guidelines of each country's legal society.
However,
we must remember to describe the pattern of color Doppler mapping and the systolic peak velocities in the thyroid arteries.
In patients with nodules,
we reccomend to inform the flow pattern with Chammas classification.
We also reccomend to estimate and report the mean resistance index for each nodule,
specially ins vascularized nodules where the B-mode characteristics are dubious.
It is desirable to report if a nodule has Dopplervelocimetric criteria and B-mode criteria of increased risk of malignancy.
We are convinced that the use of the parameters recommended by TIRADS are a big step in the standardization of the report,
as well as in the homogenization of the investigation algorithm.
We believe that color Doppler can be associated with TIRADS as an additional tool in assessing thyroid nodules risk.