CONGENITAL LESIONS
Thyroglossal duct cyst
The most frequent pediatric midline neck mass and tipically presents as a mobile midline asymptomatic mass,
although occasionaly they may become symptomatic due to infection.
They occur along the midline upper neck,
from the base of the tongue to the isthmus of the thyroid gland,
due to failure of obliteration of the thyroglossal duct during development.
Usually this patients are diagnosed with ultrasound.
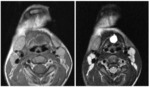
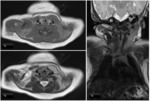
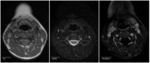
On MR they usually show simple cystic appearance (Fig.
1),
with high signal intensity on T2 and low signal intensity on T1 weighted images and thin wall with no enhancement.
Occasionaly they may have proteinaceous content with higher signal intensity on T1 weighted images.
If infected,
they may show wall thickening and enhancement.
If a soft tissue lesion is detected within the cyst it may represent ectopic thyroid tissue or papillary thyroid carcinoma wich occurs in approximately 1% of thyroglossal duct cysts.
Branchial cleft anomalies
The brachial apparatus is the embryologic precursor of the ear, muscles,
vessels,
bones,
cartilage,
and mucosa of the face,
neck and pharynx.
Abnormalities in it's development result in either a cyst (75%),
a sinus or a fistula (25%) along the anterior border of the sternocleidomastoid muscle from the tragus of the ear to the clavicle,
location depending on wich branchial arch is involved.
95% of anomalies occur on the second branchial cleft,
just below the angle of the mandible.
Usually they present as an asymptomatic mass in adolescents or young adults but they can manifest with infection or after internal hemorrhage.
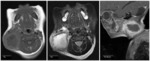
On MR they can be diagnosed by their typical location.
Signal characteristics of cysts are identical to the ones described for thyroglossal duct cysts.
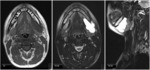
MR can help determining the path of sinus formation and if there are signs of infection as high T2 signal intensity and enhancement of the wall of the cyst and adjacent soft tissues (Fig.
2).
Lymphangioma
It can present at any age,
but 90% occur before 2 years of old,
most frequently on the head and neck,
and may be associated to chromosomal defects,
such as Turner’s syndrome and trisomy 13,
18 and 21.
Most of pediatric lymphangiomas occur in the posterior cervical triangle and are asymptomatic or present with symptoms related to mass effect due to their large size and capability to cross tissue planes.
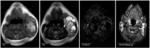
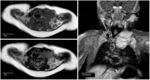
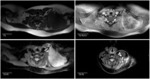
On MR it presents as a cystic multilocular mass with septa of variable thickness.
They have high signal intensity on T2-weighted images and variable signal intensity on T1 weighted images,
depending on its protein or blood content (Fig.
3).
Fluid-fluid levels are common. MR can help evaluate deep extension of the lesion when not fully appreciated on ultrasound.
Dermoid cyst
Inclusion cysts,
that contain epithelium and skin adnexa (eg. hair follicles,
sebaceous glands and sweat glands).
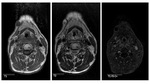
In the pediatric population they occur most frequently in the upper neck midline or near the midline of asymptomatic patients under 3 years of old.
Their MR appearance is similar to thyroglossal duct cyst and both can occur in the midline of the upper neck therefore they may be indistinguishable (Fig.
4).
BENIGN TUMOUR AND TUMOURLIKE LESIONS
Fibromatosis colli
Infantile form of fibromatosis that occurs within the sternocleidomastoid muscle and results in torticollis (73% occur on the right side).
It is a benign pseudotumour lesion,
more commonly presenting after birth trauma (e.g.
forceps delivery),
which spontaneously resolves over 4-8 months.
An ultrasound exam is enough to make this diagnose.
MR shows enlargement of the lower one-third of the sternocleidomastoid muscle with diffuse abnormal high signal intensity on T2 weighted images,
without a focal mass (Fig.
5).
Hemangioma
Benign tumour of vascular origin that can occur virtually anywhere, although the majority are found in the head and neck. They are the most common tumours of infancy (by 1 year of age there is a prevalence of 12%). Up to 50% involute by 5 years and 70% by the age of 7 years.
Diagnosis is usually made clinically.
On MR they present as well-defined lobulated lesions with intermediate signal intensity on T1 and high signal intensity on T2 weighted images.
They may show small areas of low signal intensity on T2 due to flow-voids within high-flow feeding arteries and draining veins. After injection of gadolinium contrast material there is early uniform enhancement (Fig.
6).
During involution phase they may show fat replacement with foci of high T1 signal intensity and less avid enhancement.
If perilesional edema is present,
other tumoural lesions (eg,
sarcomatous lesions and neuroblastoma) must be ruled out and biopsy may be needed.
Differential diagnosis with venous malformations may be difficult and ultrasound or CT may be useful for detection of phlebolits which are very common in venous malformations.
Ranula
Rare benign cystic lesion that can present as a pseudomass which arises from obstruction of a sublingual gland or adjacent minor salivary gland either spontaneously or as a result of trauma to the floor of mouth.
It is named simple ranula when located in the sublingual space and plunging ranula when it dissects along fascial planes from the sublingual space to the submadibular space.
Imagiologic appearence is of a cystic lesion with low signal intensity on T1 and high signal intensity on T2 weighted images (Fig.
7). MR may help establish the connection to the sublingual gland,
especially in a plunging ranula.
MALIGNANT TUMOURS
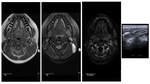
Neuroblastoma
Most arise from the adrenal glands and neck neuroblastoma lesions most frequently represent metastatic disease, although primary tumors may originate anywhere along the sympathetic chain and in up to 5% of cases they arise in the neck region having a more favorable prognosis then other primary sites.
Cervical neuroblastomas arise mainly from the superior cervical sympathetic chain behind the internal carotid artery.
It can present with Horner syndrome,
dysphagia or stridor.
MR is the best method of imaging for staging the disease.
Usually the lesions presents as an heterogeneous mass with high signal intensity on T2 weighted imaging and restricted diffusion (Fig.
8).
Gadolinium contrast administration may improve the assessment of infiltration into adjacent tissues and tumor vascularity.
For staging purposes it is important to notice if the tumour encases the carotid artery, vertebral artery,
or internal jugular vein.
It is also important to access if the tumour extends to the skull base or compresses the trachea.
Paraganglioma
Only rarely occurs in the pediatric age group and it is usually a benign tumour,
although it has malignant potential. It is more frequent when associated to familial paraganglioma syndrome,
von Hippel-Lindau syndrome or neurofibromatosis type 1.
The vast majority of paragangliomas arising in the head and neck are nonfunctional (do not secrete catecholamines).
Therefore,
late diagnosis is frequent and usually occurs due to tumour mass effects (e.g. pain),
as an incidental radiographic finding or because of family screening.
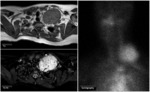
On MR they typically have a low to intermediate signal intensity on T1 weighted images and very high signal intensity on T2 and show enhancement after gadolinium contrast administration (Fig.
9).
One characteristic MR finding in paragangliomas is the presence of multiple punctate areas of signal void within the tumor,
the so-called "salt and pepper" appearance,
thought to be due to high-velocity flow in intra-tumoural vessels.
Rhabdomyosarcoma
40% of rhabdomyosarcomas occur in the head and neck region and represent the most common soft tissue sarcoma in the pediatric age group.
However,
the neck is the least common location of this region (most common are orbital and para-meningeal).
They are rapidly growing lesions which can invade and infiltrate adjacent structures.
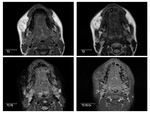
On MR they present as an heterogeneous irregular mass with high signal intensity on T2 weighted images (Fig.
10).
They usually have low to intermediate signal intensity on T1 (similar to adjacent muscle) but can show areas of high T1 signal intensity due to hemorrhage.
Rhadomyosarcoma shows avid enhancement after gadolinium contrast administration.
MR is useful to depict the tumour extension and infiltration of adjacent structures,
such as salivary glands and bone.
MR can also depict regional lymph node metastatic disease when present.
Lymphoma
In children,
lymphoma accounts for 10-15% of all cancers and most patients present with painless lymphadenopathy with or without B symptoms (fever,
night sweats and weight loss).
Non-Hodgkin lymphoma can affect the Waldeyer ring lymph nodes in younger children while Hodgkin lymphoma most frequently affects the cervical lymph nodes in older children.
Hodgkin lymphoma in particular involves cervical nodes and it is confined to this region in up to 80% of cases,
while non-Hodgkin lymphoma is frequently more widespread when it presents with cervical adenopathy.
Rarely there may be involvement of salivary glands,
most frequently associated with widespread disease and affecting the parotid glands.
While in adults CT is the most used method for staging and follow-up of the disease,
along with PET-CT,
in children MR may be useful to avoid ionizing radiation.
MR depicts enlargerd lymph nodes with low to intermediate signal intensity on T1 and intermediate to high signal intensity on T2 weighted images.
Necrosis is rare,
both before and after treatment.
As enlarged lymph nodes are common in the pediatric population,
and most frequently due to a reactive condition secondary to inflammatory processes (Fig.
11),
differential diagnosis may be difficult and biopsy may be indispensable.
Adipocytic tumours
Adipocytic tumours are relatively rare in the pediatric age group,
accounting for only 6% of all soft-tissue tumours in children.
Benign adipocytic tumours include lipoma,
lipoblastoma and lipoblastomatosis,
while liposarcomas,
which have many histologic subtypes,
show a malignant behaviour.
Lipomas comprise 66% of children’s adipocytic tumours and most frequently occur in the upper back,
neck,
proximal extremities,
and abdomen.
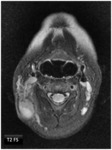
On MR they show signal intensity matching that of fat with high signal intensity on T1 and T2 weighted images and drop of signal on fat-supressed images.
They can also show low signal intensity thin septa on T1 and T2 weighted images,
which can enhance after contrast administration (Fig.
12).
Lipoblastoma and lipoblastomatosis is a rare,
rapidly growing,
benign tumour most common in children younger than 3 years of old,
comprising 30% of adypocitic tumours in children.
Although benign,
they commonly recur after surgery (9-25%).
While lipoblastoma present as a superficial encapsulated lesion,
lipoblastomatosis has no capsule and shows an infiltrative growth,
both are more frequent in the extremities and trunk but they can also develop in the head and neck regions.
Although mainly composed from fat cells,
these lesions have variable amounts of stromal tissue which on MR presents with high signal intensity on fat-saturated images,
a feature that overlaps with that of well-differentiated liposarcoma (which is extremely rare in children).
Only 4% of all liposarcomas,
across all age groups,
occur in the neck and liposarcomas anywhere are extremely rare in children.
Of all the histologic subtypes,
myxoid is the most frequent in children and can show a cystic appearance at MR imaging (Fig.
13).
Liposarcomas can present as heterogeneous circumscribed or infiltrating masses and can show no visible adipose elements,
so it’s imaging appearance is variable and,
as stated above,
they can’t be distinguished from lipoblastoma on MR imaging.