The authors reviewed the data obtained from the drug and alcohol service at Liverpool Heart and Chest Hospital in the Northwest of England between January and May 2018.
The database included 116 consecutive patients.
Of these,
a full drug history was available for 54 patients and these included for descriptive statistical analysis.
The authors found that 22 patients (40%) used multiple drugs.
The most common combination was Heroin and Crack Cocaine- 26% of all patients.
This was followed by Heroin and Cannabis- 9% of all patients.
3 patients (5%) used all three drugs.
24% used Heroin only,
22% Cannabis only and 13% cocaine only.
Overall the most commonly used drug was heroin- used by 64% of all users.
Cocaine
Trachea
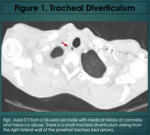
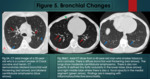
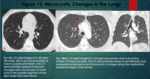
Chemical by-products produced during smoking of freebase cocaine leads to thermal injury in the airways and may cause stenosis in the airways,
particularly in the trachea (1,2,
5).
Tracheal diverticula have also been reported (19).
(Figure 1).
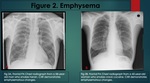
Emphysema
High intra-alveolar pressures generated during smoking,
along with toxicity from combustion products and direct toxicity from the drug all contribute to the formation of emphysema.
Furthermore,
these patients often smoke cigarettes which also increases the risk of emphysema.
This predominantly affects the upper lobes (3,
5).
(Figure 2,
4,
6).
Barotrauma
High pressures are produced in the alveoli during inhalation of cocaine.
This is further amplified by the Valsalva manoeuvre that users often produce during the smoking process.
Coughing,
which is precipitated by smoke inhalation,
also increases the intra-alveolar pressures.
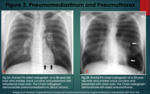
High intra-alveolar pressures cause alveolar rupture and this is manifested as pneumothorax,
pnemomediastinum,
and pneumopericardium (6). (Figure 3).
Bronchiolitis obliterans with organising pneumonia and bronchiolitis
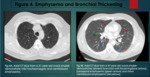
Smoking of Crack or free base cocaine also leads to submucosal fibrosis of the airways and metaplasia of the bronchial epithelium.
There is hypertrophy of the bronchial wall smooth muscles and fibroblastic plugs plugging the terminal bronchioles and the alveoli.
This results in bronchiolitis obliterans and organized pneumonia.
It manifests as diffuse alveolar opacities with peribronchovascular interstitial thickening,
fibrosis and traction bronchiectasis (3,8).
(Figure 4,
5).
Crack Lung
Crack lung is an acute respiratory syndrome which is triggered by a prolonged inflammatory response in the lungs due to inhalation of crack or freebase cocaine.
There is infiltration of the alveoli with immune cells such as eosinophils,
neutrophils and macrophages.
The inflammation leads to alveolar haemorrhage.
Patients presents with pyrexia,
hypoxia,
respiratory failure and haemoptysis.
On radiography and CT there are diffuse alveolar and parenchymal opacities affecting all zones of both lungs (3,8).
Atelectasis
Apart from emphysematous changes described above,
localized opacities the pulmonary parenchyma are common.
This may be due to mucosal oedema or constriction of the bronchioles causing areas or lines of atelectasis (3).
Talcosis and Interstitial Lung Disease
Talc is often used as a filler or diluting agents in oral medications.
When these are dissolved and injected intravenously the small particles embed in the pulmonary vascular bed causing a foreign body granulomatous reaction which ultimately causes fibrosis.
This is usually seen in heroin addicts who inject the drug intravenously (9).
When Cocaine adulterated with talc is inhaled the talc particles embed in the alveoli and also cause a granulomatous reaction.
This ultimately causes fibrosis.
Unfortunately,
the interstitial fibrosis continues to progress even after discontinuation of drug use and causes increased morbidity and mortality (3).
CT demonstrates diffuse interstitial opacities with micronodules which later increase in size.
There is also ground glass change and pan-acinar emphysema which affects the lower lobes (when intravenous drugs used) (11).
Cocaine Induced Eosinophilic Lung Disease
Eosinophilic lung disease manifests on CT as perihilar and interstitial opacification.
In more advanced disease there is patchy consolidation with a peripheral predominance.
Pulmonary Hypertension
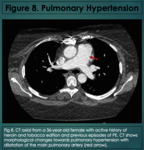
The mechanism of the development of pulmonary hypertension in cocaine smokers remains unclear.
Post mortem examination has demonstrated hypertrophy of the smooth muscles of the pulmonary arteries in approximately 20% of patients who died from cocaine use (8).
Furthermore,
vasoconstriction of the pulmonary vasculature by cocaine further increases pulmonary arterial pressures.
This vasoconstriction can be severe enough to cause pulmonary infarction.
Embolization from impurities such as talc can also cause pulmonary infarction.
(Figure 8).
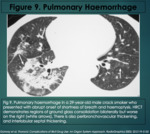
Pulmonary Haemorrhage
Cocaine is a very potent vasoconstrictor,
causing hypertension leading to endothelial damage.
Furthermore,
it causes dysfunction of the endothelium and platelets and impaired haemostasis (7).
In the lungs this may cause rupture of the submucosal vessels in the walls of the airways causing pulmonary haemorrhage (3).
Clinically this manifests as haemoptysis and less often may be life threatening.
Radiography and CT will demonstrate multifocal regions of hyperdensity in the lungs.
In CT this may also manifest as ground glass change along with interlobular septal thickening (3).
(Figure 9).
Pulmonary Oedema
Pulmonary oedema is a common finding in patients who smoke cocaine.
The aetiology in these patients can be due to both cardiogenic and non-cardiogenic causes.
Cardiogenic causes include drug induced myocardial ischemia,
dysrhythmias,
or cardiomyopathy.
Non cardiogenic cause is due to drug induced endothelial dysfunction resulting in increased permeability of the capillaries (3).
CT demonstrates thickening of the interlobular septa with peribronchovascular oedema.
With increasing,
severity alveolar oedema develops which is seen as parenchymal opacities.
Bilateral perihilar opacities are a common feature.
Patients may or may not have cardiomegaly (3).
Pneumonia
Crack cocaine causes dysfunction of the alveolar macrophages resulting in increased risk of pneumonia.
Furthermore,
as the drug induces changes to the consciousness status,
these patients are at an increased risk of aspiration pneumonia.
Chronic aspiration causes scarring and bronchiectasis.
The depended portion of the lungs (more commonly the right lung) are involved.
These changes are readily identified on chest radiographs or CT. This patient population is also at an increased risk of HIV and social conditions such as poor housing/cramped living conditions increases their risk of developing tuberculosis.
Cannabis
Trachea:
High intrathoracic pressure are produced during the smoking of cannabis which can lead to development of tracheal diverticula (19).
(Figure 1).
Marijuana Lung
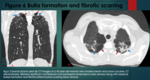
Marijuana lung describes the development of apical emphysema and large bullae.
This has been reported in case series and case reports.
However,
there is a paucity of evidence to link cannabis smoking with development of emphysema (12,13,14,15).
(Figure 6).
It is hypothesised that emphysema likely develops as a result of alveolar inflammation triggered by cannabis as well as Valsalva like breath holding techniques causing barotrauma during marijuana smoking.
These bullae may rupture spontaneously which leads to pneumothorax or pneumomediastinum (12).
(Figure 3).
Interstitial lung disease
Cannabis is often adulterated by adding talc.
This can cause pneumoconiosis.
Similar to tobacco smoking,
cannabis can also cause eosinophilic pneumonia.
Pneumonia
Marijuana smoking may cause a loss of epithelial cilia in the bronchi which may prevent clearing of microorganisms.
Furthermore,
it may also cause and suppression of macrophage activity in the alveoli.
This increases the risk of developing pneumonia (15).
Lung Cancer
The smoking of Marijuana produces similar carcinogens as tobacco smoking.
Bronchial biopsies from cannabis smokers have demonstrated development of premalignant changes.
However,
there is no robust data to suggest a link between marijuana smoking and the development of lung cancer (15).
This may be due to the short follow up period in epidemiological studies.
Heroin
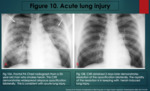
Non-Cardiogenic Pulmonary Oedema
Heroin can cause a severe and sudden onset of non-cardiogenic pulmonary oedema.
This is rapidly reversible.
As Heroin induced non-cardiogenic oedema is frequently seen in overdose fatalities its presence should alert the astute clinician and radiologist to the increased risk of mortality with this condition and the need for close monitoring.
In the early stages,
the chest radiograph demonstrates increased perihilar lung markings and bronchial thickening bilaterally.
This is followed by alveolar oedema with peri-hilar bat wing shaped opacification bilaterally.
This may be unilateral in some cases.
CT demonstrates peribronchial thickening and widespread ground glass opacifications.
Radiological changes resolve within a few days of treatment.
(Figure 10).
Pneumonitis/Alveolitis
Acute alveolitis has been described in post-mortem studies of patients who have died from Heroin and methadone related causes.
This is particularly seen in patients administering the drug intravenously.
It is hypothesized that Heroin induces an acute inflammatory reaction in the alveoli causing capillary dilatation.
Cells such as macrophages/neutrophils/eosinophils and fluid leak into the alveoli causing inflammation (16).
This inflammation can cause haemorrhagic form of the alveolitis.
Chest radiographs and CT demonstrate widespread numerous small areas of patchy or ground glass opacification in both lungs.
Fine reticulation may also be seen.
Fibrosis may develop in which is seen as honeycombing/reticular pattern.
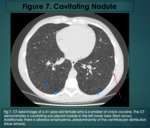
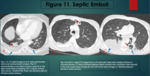
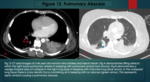
Septic Emboli
Infected DVT secondary to intravenous drug use can travel to the right atrium/ventricle and then cause embolization in the pulmonary arterial tree. abscess formation also occurs.
These patients are clinically septic and blood cultures are often positive and empyema is a feared complication.
Chest radiography and CT demonstrate multiple regions of opacification.
These are mainly seen in the lower lobes and can be unilateral or bilateral.
Cavitating lesions may also be seen.
Pleural effusions are also noted. On CT a feeding vessel may be seen with the lung abscess.
(Figure 11,
12).
Pneumonia
Heroin is a depressant of the central nervous system and hence causes reduced consciousness.
This is increases the risk of aspiration pneumonia.
Chest radiographs and CT demonstrate airspace opacification in a gravity dependent pattern.
In patients that are horizontal the most frequently involved regions are the superior segments of the lower lobes and the posterior segment of the upper lobes.
If the patient is erect the basal segments along with the middle lobe on the right and lingual on the left are more frequently involved.
COPD
Heroin smoking has been associated with early development of COPD,
particularly with emphysematous changes.
These changes are best assessed on HRCT which demonstrate an upper lobe predominant emphysematous change (17,
18).
A histopathological study of 10 cannabis smokers (some of who also smoked cocaine) demonstrated that these patients develop cysts,
blebs,
and bullae (20).