The Discovery Process ( Fig. 4 ) has four components:
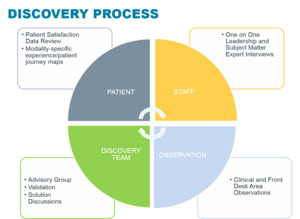
Fig. 4: The 'Discovery' Process
References: Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.
1.
Staff Discovery through One on One Leadership and Subject Matter Expert interviews.
Subject Matter Expert interviews
- Shaped as open dialogue to learn from staff about role,
patients,
process
- “Describe the role you play in caring for our patients.”
- “What are your patients like?”
- “What would make your job easier?”
Open door drop in times for any staff member
- Unguided staff driven insights augmented formal interviews
Interviews with Senior Leadership
- Management interviews reinforced themes
- “What is the biggest opportunity you see?”
- “What is your priority for the year ahead?”
Validation of themes with Discovery Team
Staff appreciated the opportunity to engage in process across both formal and informal channels
2.
Observation of Clinical and Front Desk Areas
- Ongoing process throughout the project at key milestones
- Multiple clinical and front desk area observations to augment interview themes
- Isolation of areas of opportunity
- Additional observations to inform pilot recommendations
3.
Discovery Team acting as an advisory group for validation of findings and recommending solutions.
- Comprised of employees from all role groups (administrative,
clinical,
operational)
- Participation in on-site advisory group to collaborate with and empower stakeholders to extend patient-centric culture
- Validation or refinement of preliminary findings at each project milestone
- Participation in solution discussions
4.
Patient Discovery through analysis of quantitative and qualitative patient feedback data that also helped in summarizing modality-specific patient experience maps.
It is well established that most feedback comments from patients in radiology are based on staff behavior,
communication and wait times [5].
Today,
patient-centered radiology embraces every aspect of the patient interaction with imaging services [8].
Review of patient satisfaction data revealed room for improvement in the scheduling,
registration,
waiting,
and pre-procedure preparation steps to help patients better understand what to expect,
respect their time and improve their perception of wait time.
In addition,
during post-procedure steps there were additional opportunities to set clear expectations around the results process.
Patient Journey Maps
Patient jouney maps enable digging deeper into each step in the patient's journey to gain a better understanding of the importance of each moment and develop more patient insight.
They serve as an organizational toolkit and visual guide,
and help implement patient-centered care [9].
Utilizing our patient experience program model,
we summarized Customer Journey Phases ( Fig. 5 ) and detailed Modality-Specific Patient Journey Maps ( Fig. 6 and Fig. 7 ) through subject matter expert interviews,
direct observation and patient satisfaction data.
We conducted regular brainstorming sessions and analyzed the global patient experience,
the exam specific experiences,
and captured employees’ concerns.
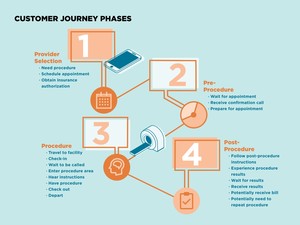
Fig. 5: Overview of the Patient Journey Phases
References: ©"Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.''
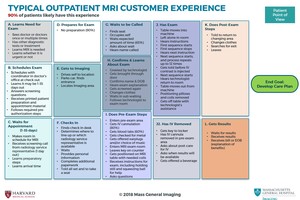
Fig. 6: Typical MRI Customer Experience
References: Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.
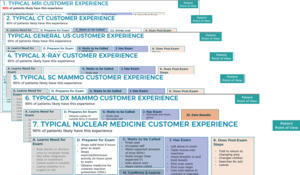
Fig. 7: Diagnostic Customer Experience Maps for MRI, CT, USG, X-Ray, Mammography, Nuclear Medicine
References: Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.
These maps aligned everyone to the patient's perspective [10] and demonstrated what we asked of the patient across their journey.
For each exam we mapped the typical patient experience – the one that 80-90% of patients experience.
We also developed an alternative map for the nuances.
We concluded that the end-to-end experience a patient has,
from learning they need an exam to getting the results,
is the 'imaging experience' for the patient,
and this entire experience is substantially more complex and varied than the exam itself ( Fig. 8 ).
The actual exam takes up a fraction of time that a patient gives to the imaging experience.
Many more minutes are given,
and more emotions are expended,
during the various other phases than during the exam.
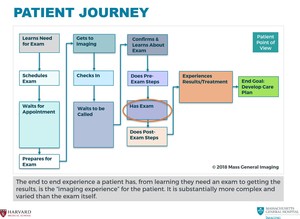
Fig. 8: Patient Journey diagram illustrates how the exam forms only a small part of the entire patient experience.
References: Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.
OPPORTUNITIES
Comparing the findings from the discovery process against the ideal state patient perspective,
we identified best practices and uncovered five areas of opportunity.
- Lack of Information - From learning of the need for exam until the results are in,
patients are not provided with enough information about the exam itself,
the preparation,
the wait time,
or accessing results to feel informed,
empowered or in control.
They have limited access to medical information if they choose to seek it out.
- Unnecessary Emotional Tensions - New patients,
and those under stress,
likely experience more negative or heated emotions like uncertainty,
worry,
frustration,
anxiety in the early stages of the experience (up until being called in for the exam) making it hard to consider the overall experience satisfying even if the exam experience itself is great.
- Inconsistent Connections - While efforts have been made to emotionally connect with patients during the exam itself and let them know they are being taken care of,
interactions from scheduling to receiving results,
critical parts of the patients’ experience,
can feel formulaic and impersonal.
Varied tones across the experience can add to inconsistency.
- Gaps in the Imaging Experience - The patients’ experience in radiology starts the moment they learn they need an exam and ends once they have their results.
Currently the active and intentional imaging patient experience is not end-to-end as we engage in the experience starting 24-48 hours before the exam and ending at departure.
- Private not always perceived as Private - Due to the layout of the waiting room and exam entry space,
patients must discuss private information with the front desk and technologist,
before and after an exam,
in close proximity to waiting patients.
Exam explanations and related discussions may also take place while in empty but common space like hallways and changing rooms.
RECOMMENDATIONS
Over a period of 15 months starting June 2017,
we worked together to formulate recommendations ( Fig. 9 ),
test our hypotheses and develop site specific implementation plans.
The recommended pilots ( Fig. 10 ) were as follows:

Fig. 9: Brainstorming Sessions with the Discovery Team helped generate a variety of ideas to help enhance the imaging patient experience across five opportunity areas.
References: Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.
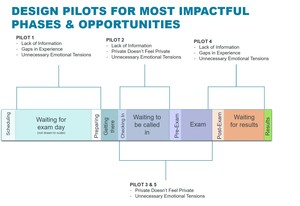
Fig. 10: Recommended Pilots encompassing different areas of opportunity.
References: Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.
Pilot 1 - Integrate Earlier
Close the information gap by connecting with patients within 1-2 days of exam scheduling.
Provide thorough overview of exam,
assist with preparation for their upcoming experience,
hear concerns,
and triage safety or medical questions.
Target Benefits : Patient feels recognized,
informed,
and prepared.
There is less angst in waiting room,
less anxiety in exam,
less questions day of,
and easier anticipation of translator needs eventually leading to efficient and successful exams.
Pilot 2 - Front desk as Hosts
Create a calming and informative check-in and waiting room experience for patients by focusing on 3 areas of opportunity:
- Set patient expectations for experience steps and timeline
- Calm the reception space and reduce visual and audio clutter
- Enhance front desk role to take ownership of the room and experience in it
Target Benefits : Patient feels welcome,
and learns what to expect with an improved waiting room comfort,
reduced wait time frustration,
and reduction in negative emotions created by audio and visual noise.
There is improved employee satisfaction due to better connection with patients.
Patients feel they are seen and attended to,
along woth an improvement in perception of privacy.
Pilot 3 - CT Prep Suite
To address perception of delays and discomfort,
for CT patients and all other patients,
associated with oral contrast.
Create a dedicated CT/Barium space that allows for privacy,
limits non-contrast patients’ exposure,
and reinforces the start of the exam.
Target benefits : Reduce perception of delay and patients feel more cared for.
They are less embarrassed and uncomfortable in the waiting room.
Waiting room comfort and cleanliness improve,
and exam related anxiety may decline.
Pilot 4 - Strong Closing
Exam technologist always closes the exam with a genuine and engaging conversation that covers: where to change,
how to exit,
exam after care,
results delivery,
patient portal,
and confirms that all concerns are addressed; may include a handout as well.
Target benefits : Patient feels cared for and leaves fully informed without having to ask possibly uncomfortable questions.
Fewer calls about results,
halo effect of positive exit extends to patient satisfaction survey,
reduce negative emotions for patients,
technologist gets more interactions and better sense of concerns.
Pilot 5 - Make Private Private
Create physical and procedural changes that improve privacy and the perception of privacy in 3 ways:
- Ensure privacy at check-in
- Enable patients to concentrate on exam explanations
- Reduce noise transfer
Target benefits : Staff develops more rigorous privacy practices in public spaces,
patients feel more cared for,
patients are less embarrassed and uncomfortable in the waiting room,
patients reveal more concerns,
waiting room privacy improves,
exam related anxiety may decline.
The summary of findings and recommendations are elaborated in Fig. 11.

Fig. 11: Pilot Summary elaborating Final Recommendations
References: Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.
EMPLOYEE ENGAGEMENT = ENHANCED PATIENT EXPERIENCE
The degree of engagement in employees towards their jobs directly influences the experience individual patients have,
and engaging stakeholders from varied organizational levels is crucial for effective healthcare quality improvement [11]. Staff engagement at our institution led to tangible increase in patient experience scores ( Fig. 12 ).
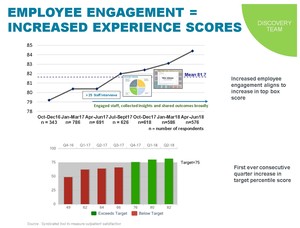
Fig. 12: Employee Engagement through the Discovery Process increased Patient Experience Scores
References: Mass General Imaging, Massachusetts General Hospital, Boston, USA 2018.