Findings:
Case 1.
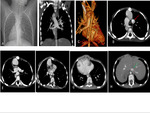
6-year old male patient with right isomerism (Ivemark syndrome),
dextrocardia,
atrioventricular (AV) canal defect,
main pulmonary artery atresia and severe pulmonary stenosis,
bilateral 3-lobed lungs,
midline liver,
asplenia,
IVC juxtaposition (status after left sided BT shunt 4 years ago and Glenn procedure 3 years ago).
Fig. 4

Fig. 4: Right isomerism (Ivemark syndrome) case. (A) Chest scanogram showing bilateral epiarterial bronchi and dextrocardia; (B and C) MPR and 3D VRD thorax reconstructions demonstrating common venous channel/vertical vein (grey arrow); (D)axial CT image showing Glenn anastomose (red arrow); (E and F) RPA and MPA hypoplasia on axial CTA images; (G) Total AV canal defect; (H) IVC anterior to abdominal aorta position (green arrow showing juxtaposition of IVC).
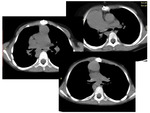
Case 2. 1-year old female patient with situs inversus,
dextrocardia,
VSD,
overriding aorta,
RVOT infundibular stenosis,
main,
right and left pulmonary arteries hypoplasia (Fallot Tetralogy).
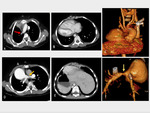
Case 3. 6-year old female patient with situs inversus,
dextrocardia,
three-lobed lung on the left and two-lobed lung on the right with bifurcated spleen (status after palliative BT shunt (in 2013) and total correction of double outlet right ventricle (DORV) +LPA patch plasty 2 years ago) Fig. 6 .

Fig. 6: Situs inversus case. Status after total DORV and pulmonary stenosis correction with LPA patch plasty. (A) Closed right sided BT shunt (red arrow); (B) dextrocardia on axial CT image; (C) 3D VRT demonstrating MPA dilatation; (E and F) axial CT image and 3D VRT reconstruction of LPA local restenosis on previous patch plasty level (yellow arrow); (G) inversion of spleen and liver on axial abdominal CT image.
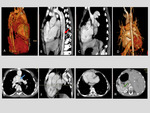
Case 4. 8 -year old female patient with F-anisosplenia form of heterotaxy with dextrocardia,
Azygos continuation,
spleen bifurcation (status post Mustard surgery 3 years ago) Fig. 5 .

Fig. 5: F-anisosplenia case with dextrocardia, bilateral two-lobed lungs and bifurcated spleen. (A, B and C) 3D VRT and Sagittal MPR showing dilated v. Azygos (Azygos continuation of IVC) (red arrow); (D) 3D VRT posterior view; (E) dilatation of main pulmonary artery (blue arrow); (F) RVOT on sagittal MPR; (G) dilatation of morphological RV; (H) bifurcated spleen and left sided liver (green arrow).
Case 5. 26-year old female patient with situs abnormality (mesocardia,
atrial and visceral situs inversion),
DORV,
congenitally corrected transposition of the great arteries (CCTGA),
subpulmonary VSD (Status post right sided BT shunt 4 years ago).
Procedure details: All pediatric patients had undergone thorax- CTA under sedation with special low-dose pediatric protocol (80-100 KV,
25-50 mA,
0.9 mm thickness and 0.45 mm increment) and one adult patient underwent Thorax CTA with standard dose modulation protocol using 256- slice CT machine.
Immobilization and continuous monitoring of pulse oximetry and heart rate were performed during sedation. ECG-gating was not applied in most of pediatric patients due to limitations.
Non-ionic contrast agent (1-1.5 mL/kg of 370 mg Iodine/ml contrast media) was injected at 0.8 -1 ml/s rate via small-ganged catheters at different sites,
real time contrast bolus tracking was used.
In complex cases on native locator image is not easy to find the right vessel for tracking Fig. 3.
In our hospital we suggest two scan series with in/out direction,
with scan delay 10-15 sec between them to avoid missing of contrast media in any vascular structure.
For detailed and accurate interpretation of situs anomalies associated with cardiovascular pathology a segmental approach with determining the position of the atria,
viscera,
right and left ventricles,
and great vessels step by step were performed by using three-dimensional volume rendering technique (VRT),
multiplanar reformations (MPR) and two-dimensional maximum intensity projection (MIP) reconstructs in sagittal,
coronal and axial views [2,12] Fig. 2.