Keywords:
Breast, MR, Diagnostic procedure
Authors:
P. Jagmohan1, C. Grippo2, C. Sodano3, P. Clauser4, P. Kapetas3, T. H. Helbich3, P. A. T. Baltzer3; 1Singapore/SG, 2Rome/IT, 3Vienna/AT, 4Vienna, Vienna/AT
DOI:
10.26044/ecr2019/C-2750
Conclusion
It is well established that the time-signal intensity curve (TIC) from dynamic contrast-enhanced magnetic resonance imaging (DCE- MRI) reflects the hemodynamic features of a specific lesion.[5]
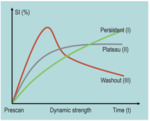
The enhancement kinetics are an important aid in characterizing breast lesions and improving delineation between benign and malignant lesions. The shape of the time-signal intensity curve is classified according to ACR BIRADS lexicon as persistent enhancing "Type 1",
plateau "Type 2",
or washout "Type 3" (Fig.
3).
Several studies have reported that time-signal intensity curves have a very high sensitivity but variable specificity for the diagnosis of breast cancer.
However,
in general a Type 1 persistent enhancing curve is correlated with benign lesions while a Type 3 wash-out curve has been shown to be a strong independent predictor of malignancy.
Kuhl et al.
reported cancer in 87% of lesions with any washout while in a study by Schnall et al.
malignancy was identified in 76% of lesions showing washout kinetics.
[5][6]
While DCE-MRI has gained widespread use for breast imaging,
there is no widely accepted protocol for obtaining images.
Although the ACR breast MRI accreditation program has now established minimum standards for technical parameters,
the guidelines allow for differing imaging protocols.
A prior study evaluated the effects of post-contrast timing on delayed-phase lesion kinetics assessment and the ability to discriminate between malignant from benign lesions.
They compared delayed-phase kinetic parameters including percentages of persistent,
plateau,
and washout,
and categorizations of predominant and worst curve type at two different delayed time – points and found no significant differences in diagnostic accuracy between the two timings.
[7]
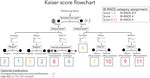
In our study we investigated the effect of initial post contrast timing (early vs peak enhancement) on the Kaiser score,
a diagnostic flow chart which characterizes breast lesions on MRI based on five diagnostic criteria and provides a clinical decision rule.[8]
No uniform method for interpretation of the kinetic curve have been described.
Different methods designed to assess dynamic enhancement curves have shown comparable results.
The Kaiser score recommends a visual assessment of the curve types as it is faster and less biased by motion and/or partial volume artefacts.
According to the score,
the shape of the signal-intensity time curve is assessed by comparing either early or peak and delayed enhancement time points with the curve type as described above.
These preliminary results highlight that the diagnostic performance of the Kaiser score is significantly influenced by how the initial enhancement timepoint and enhancement curve types are determined.
Using the peak enhancement of the first two timepoints as the initial enhancement reference is preferable as it provides superior specificity.