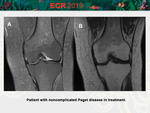
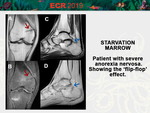
We made a retrospective analysis of 78 patients from 2016 to 2018 performed with 1.5 and 3T MR,
including pediatrics and adults,
who showed particular findings in bone marrow,
correlating the imaging characteristics and etiology.
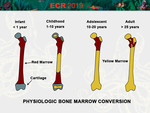
Physiological bone marrow changes
[Fig.
1].
Red to yellow marrow conversion patterns
* Skeleton: peripheral -> central
* Long bones: epiphysis -> diaphysis -> distal metaphysis -> proximal metaphysis
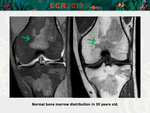
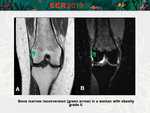
Reconversion of Yellow to Red Marrow
Characterized by the reverse sequence of events that occur during physiologic red to yellow marrow conversion: loss of the large marrow fat cells through lipolysis allows previously collapsed sinusoids to expand.
KEYPOINTS in reconversion of yellow to red marrow patterns:
*Skeleton: central -> peripheral
*Long bones: Proximal metaphysis -> distal metaphysis -> diaphysis -> epiphysis.
*Causes:
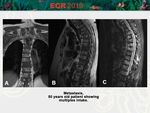
- Marrow infiltration/replacement disorders (metastases,
hematologic disorders)
- Severe anemia
- Chronic heart failure
- Hematopoietic growth factors
- Extensive irradiation (reconversion occurs in the nonirradiated skeleton)
- Long-distance running
- High-altitude living
- Heavy smoking
- Obesity
[Fig.
2-3]
In order to simplify the analysis,
we provide a resume of the classic bone marrow patterns describe in the literature:
FOCAL PATTERN
Consists of well-defined foci of abnormal signal intensity on a background of normal marrow.
HYPERINTENSE FOCAL PATTERN
This pattern almost always represents benign processes.
They are often associated with bone marrow foci that result from the heterogeneous conversion of red to yellow marrow.
Common causes:
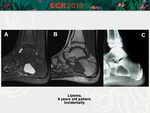
• Focal fatty marrow
• Hemangiomas/Lipoangiomas
High intensity signal in T2FS-WI or STIR,
when present,
as well as the identification of intralesional hypertrophied bone trabeculae distinguish these lesions from the bone marrow islands.
Also may shows high signal on T1 in lipohemangiomas due to the fatty content. [Fig.
4]
• Modic II degenerative endplate changes
• Bone infarcts (osteonecrotic lesions)
Geographic edge of low signal intensity surrounding the hyperintense focus is pathognomonic of this lesion.
• Healing lesions
Focal lesions of neoplastic or infectious origin may become partially or completely hyperintense when,
during the healing process,
the bone marrow reappears adjacent to the unaffected bone marrow.
There may be extremely rare cases in which this pattern may be caused by melanoma metastasis or hemorrhagic myelomatous lesions.
HYPOINTENSE FOCAL PATTERN
We ought not try to characterize a hypointense lesion of less than 5 mm.
Hypointense focal lesions (greater than 5 mm) with a higher signal compare to non-degenerated intervertebral disc or muscle are usually benign and most often represent remnants of red marrow.
Common causes:
• Remains of red marrow
A high T1 signal source at the center of the hypointense lesion,
when present,
is a diagnosis of normal red marrow.
Compared with malignant bone marrow lesions,
red marrow foci have less defined margins.
Otherwise,
other sequences and,
particularly,
chemical shift images (> 20% signal decay in out-of-phase images) and enhanced contrast-enhanced sequences in T1 (<40% contrast uptake) can help diagnose the presence of red marrow remains.
• Atypical hemangiomas
If the hypointense lesion in T1 retains some high signal in the images weighted in T2 with fat suppression,
then it is almost certainly a hemangioma (also look for reinforced trabeculae of low signal); otherwise,
it is focal fat marrow.
• Metastasis [Fig.
5]
Remember that metastases may also occur along the endplates and look for specific signs of benign lesions.
It is unlikely that there is a sclerotic border,
more clearly seen on CT images,
but also identifiable on MR images,
with untreated bone metastases.
Malignant focal bone marrow lesions are typically hypointense to disk or non-degenerated muscle,
sometimes isointense but rarely hyperintense.
A hyperintense edge in the T2-weighted images surrounding the signal of the empty lesion (halo sign T2) is diagnostic of an osteoblastic metastasis.
Irradiate bone trabeculae,
on the other hand,
favors the diagnosis of enostosis.
Images of malignant lesions of the focal marrow should be carefully inspected for the presence of extraosseous mass on the nerves or spinal cord.
T1-weighted images are best suited for evaluating the tumor that extends to the epidural space or the intervertebral foramina.
In contrast images,
the addition of fat suppression facilitates the detection of extraosseous tumors.
• Hematological neoplasms
A focal lesion that is located along a vertebral endplate is likely to be a degenerative change Modic; look for the degeneration of the adjacent disk and similar changes of the other terminal plate at the same level.
Spondylodiscitis can also present with a hypointense T1 signal along the vertebral plates.
However,
the puffed disc will be hyperintense on T2-enhanced images,
and will improve to some extent.
The presence of extraosseous soft tissue or even a frank abscess establishes the diagnosis of spondylodiscitis in the face of degenerative changes of the endplate.
The hyperintensity of the signal in the images weighted by diffusion of high B value favors the spondylodiscitis on Modic I changes.
A Schmorl nodule is easily diagnosed when there is a loss of cortical contiguity and a signal intensity similar to that of the intervertebral disc.
SIGNAL-VOID FOCAL PATTERN
Signal-void focal lesions have well-defined borders and the signal in this pattern is lower than that of hypointense focal bone marrow lesions,
and it may be produced by osteosclerotic processes or air. They remain of low signal intensity on all MR sequences due to the absence of mobile protons.
Common causes:
• Enostosis (bone island)
Enostosis is a frequent cause of benign focal signal-vacuum injury.
• Osteoblastic metastasis
• Osteoblastic lymphomatous lesions
• Myelomatous sclerotic lesions (rare)
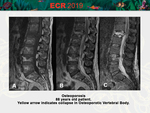
• Vertebral osteonecrosis with intravertebral gas
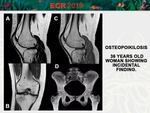
• Osteopoikilosis,
mastocytosis
Osteopoikilosis,
is a rare benign and asymptomatic sclerosing bone dysplasia.
[Fig.
6]
Characterized by multiple foci of bone sclerosis like focal signal-void lesions.
VARIEGATED PATTERN
A varied pattern (microfocal,
"salt and pepper") consists of innumerable small,
alternating,
hyperintense and hypointense foci. [Fig.
7]
Common causes:
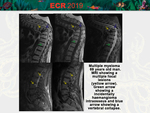
• Osteolytic metastases,
multiple myeloma.
[Fig.
8]
The variegated appearance (also called "mosaic") is caused by alternating light bulbs of high and low signal intensity that represent normal remains of bone and red marrow,
respectively.
• Osteoblastic metastasis,
osteopoikilosis (empty signal)
A varied pattern with osteolytic metastatic disease and multiple myeloma can also be observed,
where innumerable hypointense foci represent malignant deposits.
Bone osteoblastic metastases and osteopoikilosis can occur with innumerable foci,
isointense to cortical bone (signal emptying) in a varied pattern.
DIFFUSE PATTERN
Signal intensity of the entire bone marrow is altered without areas of normal pattern.
HYPERINTENSE DIFFUSE PATTERN
The abnormal marrow is hyperintense to red marrow and isointense to extraosseous fat.
Common causes:
• Normal pattern in elderly people
Increased fat content in the marrow,
reflecting a very high content of fat in the spinal cord distributed homogeneously.
• Bone depletion (aplastic anemia)
The pancytopenia that characterizes this hematological disorder leads to a marked hypocellularity of the bone marrow and to an increase in the fat content,
which results in a diffuse high signal in T1-WI.
A hyperintense diffuse pattern limited to a portion of the medulla (hyperintense regional pattern) is easy to diagnose and is related to previous irradiation of the bone marrow,
which is strictly adjusted to the radiation portals.
HYPOINTENSE DIFFUSE PATTERN
Abnormal marrow is hypointense or,
occasionally,
isointense to muscle and nondegeneratedintervertebral discs.
The bone marrow that is hypointense for the intervertebral discs or the muscle is definitely abnormal.
Use chemical shift images and enhanced by contrast for verification.
The diffuse image can be valuable; It is unlikely that a diffuse pattern of bone marrow with ADC values lower than 0.5 × 10 -3 mm2/s is malignant.
Note that a normal MRI pattern does not exclude involvement of the malignant marrow since MRI may not detect low percentages of malignant bone marrow infiltration (particularly with malignant hematologic malignancies).
Common causes:
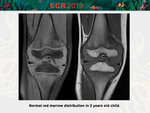
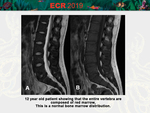
• Normal pattern in young individuals (higher content of red marrow) [Fig.
9]
If the intensity of the signal is greater than,
or occasionally,
equal to that of the discs or muscles,
it may be due to the hypercellular red marrow.
In children and young adults,
a diffuse low signal intensity column may be related to the presence of normal hypercellular red marrow.
• Red marrow reconversion
In adults,
carefully review the medical history to look for chronic anemia or other causes or red-cell reconversion (administration of hematopoietic growth factors,
pronounced physical activity,
etc.).
• Lymphoproliferative disorders
The lymphoproliferative disorders (leukemia,
lymphoma,
multiple myeloma) can manifest with a diffuse hypointense pattern.
Diffuse hypointense bone marrow patterns may be homogeneous as in leukemia or heterogeneous patients with focal areas superimposed on even lower signal intensity,
a pattern commonly observed in patients with lymphoma; focal areas of low signal intensity,
in a context of diffusely hypointense marrow,
may be related to denser aggregates of malignant cells.
• Myeloproliferative disorders and Myelodysplastic syndromes
Myeloproliferative diseases (polycythemia vera,
mastocytosis,
myelophysis) and myelodysplastic syndromes may also present with hypointense patterns of diffuse bone marrow.
[Fig.
10]
• Gaucher's disease
Gaucher disease is a metabolic disorder in which the bone marrow is replaced by abnormal histiocytes containing glucocerebrosides,
and may manifest with diffuse T1 hypointensity.
• Metastasis (rarely)
Metastatic disease,
particularly of small round cell primary tumors,
can rarely manifest with a diffuse hypointense bone marrow pattern.
SIGNAL-VOID DIFFUSE PATTERN
Common causes:
• Hemosiderosis
The ferric iron of hemosiderin is responsible for the fall in signal intensity of the bone marrow due to its shortening effects T1 and T2.
REGIONAL PATTERN
In a regional bone marrow pattern,
a specific,
small or large,
area of the marrow is affected in a more or less diffuse manner due to a regional cause.
HYPERINTENSE REGIONAL PATTERN
Common causes:
• Radiation therapy
A hyperintense pattern of regional bone marrow is observed after radiation therapy,
which causes a decrease in the bone marrow; it is confined to the radiation field with an acute transition zone to the non-irradiated bone marrow.
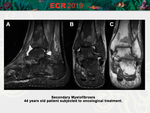
HYPOINTENSE REGIONAL PATTERN
A hypointense regional bone marrow pattern with infiltrating bone marrow processes is often seen and is generally characterized by a broad transition zone.
Abnormal bone marrow is heterogeneous and moderately hypointense to fat,
but hyperintense to muscular and non-degenerated intervertebral discs.
Areas of low signal intensity (infiltration process) can alternate with areas of high signal intensity (fat marrow).
This pattern is better recognized in the images weighted in T2 with suppression of fat.
Unlike a process of bone marrow replacement,
the infiltrative process does not completely replace the normal bone marrow,
but intermixes and coexists with it.
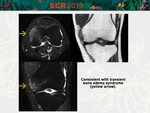
Common causes:
• Bone marrow edema syndrome (transient osteoporosis,
regional migratory osteoporosis,
complex regional pain syndrome).
[Fig.
11]
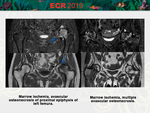
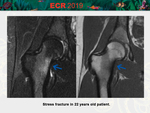
• Trauma (bone hematoma,
fracture).
[Fig.
12-13-14]
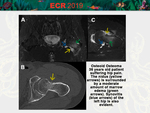
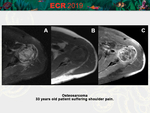
• Edema associated with bone tumors [Fig 15-16]
Edema associated with benign (for example,
osteoid osteoma) or malignant (for example,
osteosarcoma) bone tumors may be responsible for a regional hypointense pattern.
The degenerative changes of the type I endplate also present with a regional hypointense pattern.
• Changes of degenerative plate Modic type I
• Osteomyelitis (including spondylodiscitis) and Inflammation or disease of the infectious joints
Osteomyelitis and the infectious or inflammatory processes of the joints are often associated with reactive edema of adjacent bones that manifests with a regional hypointense pattern.
In spondylodiscitis,
the characteristic changes of the intervertebral disc involved point to the correct diagnosis.