LK comprises of a complex arrangement of muscles,
tendons and ligaments providing primary restraint against varus angulation.
The LK can be divided into two main functional compartments:
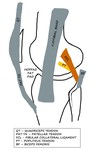
Anterolateral compartment: Fig. 1
- Joint Capsule
- Iliotibial band (ITB)
- Hoffas fat pad
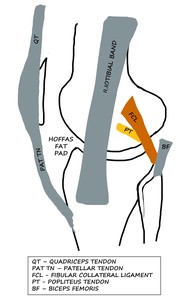
Fig. 1: LK: Schematic diagram showing the anterolateral and some of the posterolateral structures around the LK.
References: Department of Radiology, VMMC and SJH, New Delhi, India
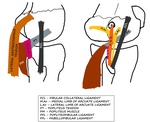
Posterolateral compartment: Fig. 2
- Biceps femoris (BF)
- Fibular collateral ligament (FCL)
- Arcuate ligament (AL)
- Popliteus muscle-tendon unit (PMT)
- Popliteofibular ligament (PFL)
- Fabellofibular ligament (FFL)
- Posterolateral capsule [1]
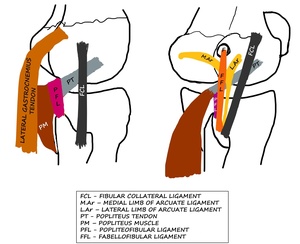
Fig. 2: LK: Schematic diagram showing the posterolateral corner structures of LK.
References: Department of Radiology, VMMC and SJH, New Delhi, India
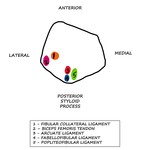
The fibular head anchors the posterolateral corner providing attachments to several structures.
[2] Fig. 3
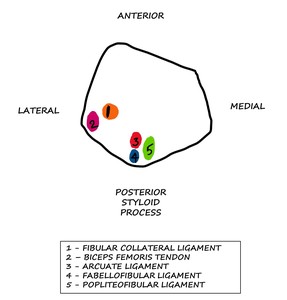
Fig. 3: LK: Schematic diagram showing the attachments of ligaments and tendons on the proximal fibula which acts as an ‘anchor’ for the posterolateral corner.
References: Department of Radiology, VMMC and SJH, New Delhi, India
LK anatomy has been described using a three-layer approach from superficial to deep:
Layer 1 – ITB,
BF
Layer 2 - Lateral patellar retinaculum,
patellofemoral ligament,
FCL
Layer 3 – PMT,
PFT,
joint capsule,
AL,
fabella,
FFL and peroneal nerve[2]
The plethora of pathologies at the LK though less common than the medial knee can be significantly more disabling.
Isolated LK injuries are uncommon being frequently associated with cruciate injuries leading to a difficult clinical diagnosis.[1]
Sonography allows a comprehensive diagnostic approach in a non-invasive,
inexpensive,
portable and radiation-free manner.
It additionally scores by allowing dynamic assessment and directing accurate targeted therapeutic interventions.[3]
Minimally invasive interventions can improve the specificity of treatment,
the patient’s experience and outcome,
the length of hospital stays,
and potentially the cost of care.
They act as a bridge between failed conservative management and aggressive surgical interventions.
Nowadays most musculoskeletal indications are treated with minimally invasive interventions with surgery reserved for recalcitrant cases.[4]