ULTRASOUND (US) EVALUATION OF LK –
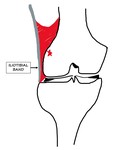
Patient position - Supine with leg internal rotated and knee slightly flexed. Fig. 4
Probe - High-frequency transducer.[5]
Fig. 4: LK: Patient position for LK sonography.
References: Department of Radiology, VMMC and SJH, New Delhi, India
LK CHECKLIST:
The main five structures evaluated are the iliotibial band,
fibular collateral ligament,
the biceps femoris tendon,
popliteus tendon and the lateral meniscus.
(For each structure,
a table showing the probe positioning and normal appearance of that structure will be provided,
along with their image references.)
1) ILIOTIBIAL BAND (ITB) Table 1 Fig. 5 Fig. 6 Fig. 7

Table 1: ITB: Probe positioning and normal appearance.
References: Department of Radiology, VMMC and SJH, New Delhi, India
Fig. 5: ITB - Probe position for evaluation ITB.
References: Department of Radiology, VMMC and SJH, New Delhi, India
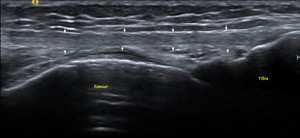
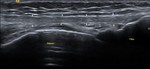
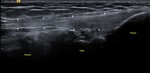
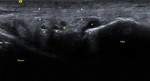
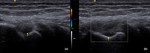
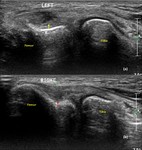
Fig. 6: ITB – Ultrasound (US) image showing the normal ITB (white arrows).
References: Department of Radiology, VMMC and SJH, New Delhi, India
Fig. 7: VIDEO: Normal ITB on US.
References: Department of Radiology, VMMC and SJH, New Delhi, India
2) FIBULAR COLLATERAL LIGAMENT (FCL) Table 2 Fig. 8 Fig. 9

Table 2: FCL: Probe positioning and normal appearance.
References: Department of Radiology, VMMC and SJH, New Delhi, India
Fig. 8: FCL: Probe position for evaluation of FCL.
References: Department of Radiology, VMMC and SJH, New Delhi, India
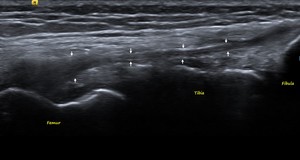
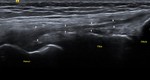
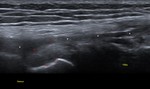
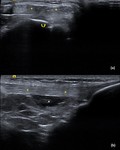
Fig. 9: FCL: US image showing the normal FCL (white arrows) with its femoral and fibular attachments.
References: Department of Radiology, VMMC and SJH, New Delhi, India
3) BICEPS FEMORIS (BF) Table 3 Fig. 10 Fig. 11

Table 3: BF: Probe positioning and normal appearance.
References: Department of Radiology, VMMC and SJH, New Delhi, India
Fig. 10: BF: Probe position for evaluation of BF.
References: Department of Radiology, VMMC and SJH, New Delhi, India
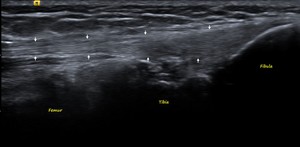
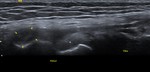
Fig. 11: BF: US image showing the normal BF (white arrows) with its musculotendinous junction and fibular attachment.
References: Department of Radiology, VMMC and SJH, New Delhi, India
4) POPLITEUS Table 4 Fig. 12

Table 4: POPLITEUS: Probe positioning and normal appearance.
References: Department of Radiology, VMMC and SJH, New Delhi, India
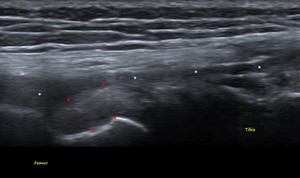
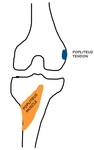
Fig. 12: POPLITEUS TENDON - US image showing the normal Popliteus tendon (red arrows) at its femoral attachment. FCL (white stars) is seen superficial to it.
References: Department of Radiology, VMMC and SJH, New Delhi, India
5) LATERAL MENISCUS (LM) Table 5 Fig. 13 Fig. 14

Table 5: LM: Probe positioning and normal appearance.
References: Department of Radiology, VMMC and SJH, New Delhi, India
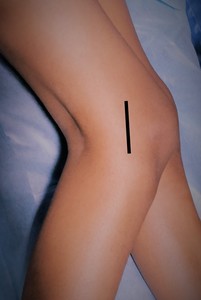
Fig. 13: LM: Probe position for evaluation of LM.
References: Department of Radiology, VMMC and SJH, New Delhi, India
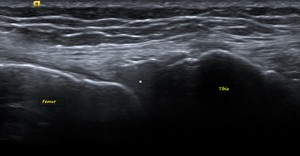
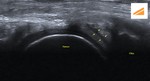
Fig. 14: LM: US image showing the normal homogenous triangular iso-hyperechoic LM (white star).
References: Department of Radiology, VMMC and SJH, New Delhi, India
PATHOLOGIES AND INTERVENTIONS:
ILIOTIBIAL BAND:
Aka Maissiat’s band.
Origin - Formed by the coalescence of the aponeurotic coverings of the tensor fascia lata and gluteus maximus muscles.
Insertion - At least five distal insertions of the ITB about the knee have been described including linea aspera,
lateral epicondyle,
Gerdy's tubercle (GT),
lateral patellar retinaculum and onto tibia posterolateral to GT. Fig. 15
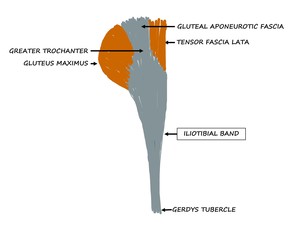
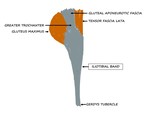
Fig. 15: Schematic diagram showing the origin and insertion of the ITB.
References: Department of Radiology, VMMC and SJH, New Delhi, India
ITB FRICTION SYNDROME (ITBFS) occurs due to chronic overuse so that the classic presentation is that of an active young person with LK pain that increases with physical activity.
ETIOGENESIS –
- Irritation of ITB and underlying fat against the lateral epicondyle caused by its anterior and posterior movement with knee extension and flexion.[6] Fig. 16 Fig. 17 Fig. 18
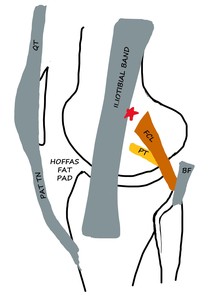
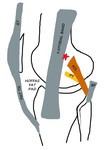
Fig. 16: ITB - Schematic diagram of LK In Extension - ITB slightly overlies the lateral epicondyle (red star), just anterior to the proximal insertion of FCL. PAT TN - Patellar tendon, QT - Quadriceps tendon, PT - Popliteus tendon, BF - Biceps femoris, FCL - Fibular collateral ligament.
References: Department of Radiology, VMMC and SJH, New Delhi, India
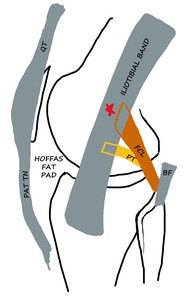
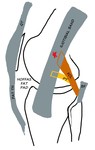
Fig. 17: ITB: Schematic diagram of LK in Flexion - ITB overlaps the lateral epicondyle (red star). It also contacts the proximal fibers of the FCL and crosses the popliteus tendon with further flexion. PAT TN - Patellar tendon, QT - Quadriceps tendon, PT - Popliteus tendon, BF - Biceps femoris, FCL - Fibular collateral ligament.
References: Department of Radiology, VMMC and SJH, New Delhi, India
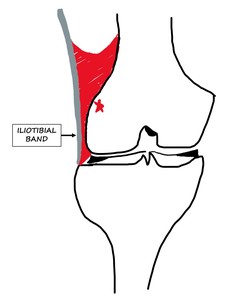
Fig. 18: ITBFS: The red area is the space between the ITB and lateral epicondyle (red star) that is affected by ITBFS.
References: Department of Radiology, VMMC and SJH, New Delhi, India
SONOGRAPHIC FINDINGS: Fig. 19
- Early stage - Heterogeneity and hyperechogenicity of the fat tissue interposed between ITB and femur
- Late stage -
- Development of contiguous adventitious bursae.
- Thickening and heterogeneity of ITB.[7]
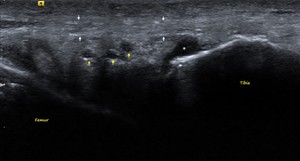
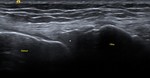
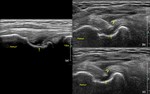
Fig. 19: ITBFS: US image showing the mildly heterogenous ITB (white arrows). Few cysts (yellow arrows) and a fluid pocket (white star) are seen within the fat pad posterior to the ITB consistent with formation of adventitious bursae.
References: Department of Radiology, VMMC and SJH, New Delhi, India
INTERVENTIONS: Fig. 20 Fig. 21
- For inflammation - US-guided steroid – local anesthetic (S-LA) injections are given which are both therapeutic and diagnostic.[6]
- Associated iliotibial bursitis is treated with aspiration followed by S-LA injections.[4,6]
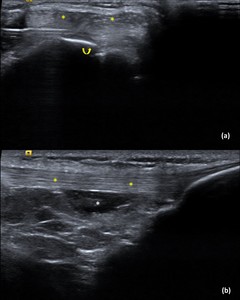
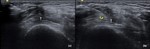
Fig. 20: ITBFS – Intervention: A 28-year-old male runner presented with left lateral knee pain centered around the lateral epicondyle, clinically diagnosed as a case of ITBFS.
Intervention performed: Using a 22G needle the target site was infiltrated with LA. The needle was further advanced within the fat pad posteriorly and 4-5ml of a diluted Steroid-LA solution was administered.
a) Pre-injection axial Image of the left anterolateral knee: Shows the ITB (yellow stars) with the needle within the underlying fat (curved yellow arrow).
b) Post-injection longitudinal Image of the left anterolateral knee: Shows the ITB (yellow stars) with the Steroid-LA solution (white star) within the fat.
References: Department of Radiology, VMMC and SJH, New Delhi, India
Fig. 21: VIDEO: ITBFS INTERVENTION: A 28-year-old male runner presented with left lateral knee pain centered around the lateral epicondyle, clinically diagnosed as a case of ITBFS. Intervention performed: Using a 22G needle the target site was infiltrated with LA. The needle was further advanced within the fat pad posteriorly and 4-5ml of a diluted Steroid-LA solution was administered.
References: Department of Radiology, VMMC and SJH, New Delhi, India
FIBULAR COLLATERAL LIGAMENT:
Aka ‘True lateral collateral ligament’.
Origin - Lateral femoral epicondyle.
Insertion – Lateral aspect of the fibular head and neck anterior and distal to the fibular styloid process.
It often has a conjoined insertion with the biceps femoris tendon
FCL is extracapsular.
FCL has no meniscal attachment.
[2]
Grades of FCL injury:
- Grade 1 – Mild edema
- Grade 2 – Partial tear
- Grade 3 – Complete tear [8]
FCL SPRAIN:
SONOGRAPHIC FINDINGS: Fig. 22
US appearances of different grades of FCL injury:
- Grade 1 – Hypoechoic thickening without fiber discontinuity.
- Grade 2 – Partial fiber discontinuity.
- Grade 3 – Complete fiber discontinuity.[9,10]
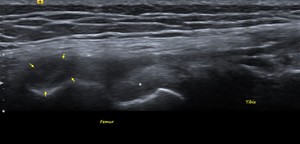
Fig. 22: FCL – GRADE 1 INJURY: Longitudinal US image shows hypoechoic thickening of the FCL at its femoral attachment with maintained fiber continuity (yellow arrows), consistent with mild sprain. Also seen in the image is the normal popliteus tendon (white star) deep and inferior to it.
References: Department of Radiology, VMMC and SJH, New Delhi, India
INTERVENTIONS: Fig. 23 Fig. 24
- Platelet-rich plasma (PRP) injections have been tried for rapid healing of ligamentous injuries.
- S-LA injections can be used for symptomatic pain relief.
[4]
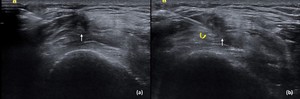
Fig. 23: FCL – GRADE 2 INJURY:
A 37-year-old male presented with left lateral knee pain. On US scanning, a partial tear of FCL was found.
Intervention performed: Using a 22G needle the target site was infiltrated with LA. The needle was then advanced to the partial tear site in the FCL and 2-3ml of a diluted PRP solution was administered.
a) Axial US image shows focal hypoechoic area within the FCL with fiber discontinuity consistent with partial tear (white arrow).
b) Axial US image shows needle tip (curved yellow arrow) within the tear site (white arrow).
References: Department of Radiology, VMMC and SJH, New Delhi, India
Fig. 24: VIDEO: FCL – GRADE 2 INJURY INTERVENTION: A 37-year-old male presented with left lateral knee pain. On US scanning, a partial tear of FCL was found. Intervention performed: Using a 22G needle the target site was infiltrated with LA. The needle was then advanced to the partial tear site in the FCL and 2-3ml of a diluted PRP solution was administered.
References: Department of Radiology, VMMC and SJH, New Delhi, India
POPLITEUS MUSCULOTENDINOUS COMPLEX:
Origin - Posteromedial tibial surface proximal to the soleal line.
Insertion - In a depression on the lateral femoral condyle,
anteroinferior to the FCL attachment. Fig. 25
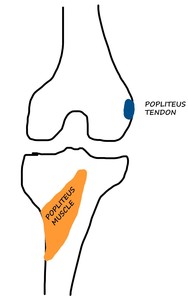
Fig. 25: POPLITEUS: Schematic diagram of the posterior knee showing the wide attachment of the popliteus muscle on the tibia (posteromedial tibial surface proximal to the soleal line), and the attachment of the popliteus tendon at the lateral femoral condyle.
References: Department of Radiology, VMMC and SJH, New Delhi, India
Popliteus tendon is intracapsular,
but extra-articular and extrasynovial.
Musculotendinous injuries classification:
- First degree – Minimal fiber disruption
- Second degree – Partial tear without retraction
- Third degree – Complete tear
Points to include in the Radiology report:
1. Site of the tear - intra- or extra-articular
2. Extent - partial or full-thickness
3. Presence of a bone fragment attached to the avulsed tendon
4. Degree of tendon retraction
5. Associated ligamentous and meniscal injuries
POPLITEUS TENDINOSIS AND PARTIAL TEAR:
SONOGRAPHIC FEATURES:
- Tendinosis – Tendon appears hypoechoic and may be bulky.
Fig. 26
- Tears are seen as partial or complete fiber discontinuity.[2] Fig. 27 Fig. 28 Fig. 29
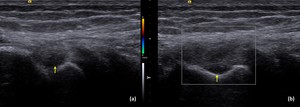
Fig. 26: POPLITEUS TENDINOSIS:
a) Longitudinal US image shows a focal hypoechoic area within the popliteus tendon with mild thickening of the tendon at its femoral attachment (yellow arrow). Fiber continuity is maintained.
b) Doppler shows no increased vascularity. Findings are consistent with chronic tendinosis.
References: Department of Radiology, VMMC and SJH, New Delhi, India
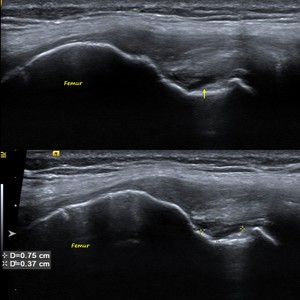
Fig. 27: POPLITEUS PARTIAL TEAR: Longitudinal US image showing partial thickness articular surface tear of the popliteus tendon at its femoral attachment measuring 7.5x3.7mm (yellow arrow).
References: Department of Radiology, VMMC and SJH, New Delhi, India
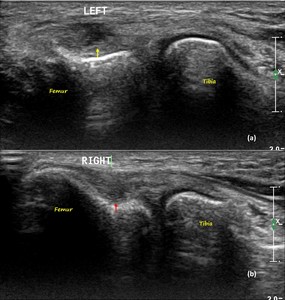
Fig. 28: POPLITEUS PARTIAL TEAR AND TENDINOSIS:
a) US image of left knee shows high grade partial thickness tear at the non-articular aspect of the popliteus tendon near its femoral attachment (yellow arrow).
b) US image of right knee shows a small focal hypoechoic area within the popliteus tendon at its femoral attachment with maintained fiber continuity (red arrow), consistent with mild tendinosis.
References: Department of Radiology, VMMC and SJH, New Delhi, India
INTERVENTIONS: Fig. 29
- S-LA injections - For tendinosis and tendinitis.[11]
- Platelet‑rich plasma / Prolotherapy – For partial tears.
[4]
- Complete tears with retraction require surgical management.
[2]
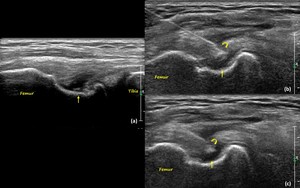
Fig. 29: POPLITEUS PARTIAL TEAR WITH INTERVENTION:
A 29-year-old male presented with right lateral knee pain. US scanning revealed a high grade partial tear of the popliteus tendon at its femoral attachment.
Intervention performed: Under US guidance the target site was infiltrated with LA using a 23G needle. The needle was then advanced to tear site in the popliteus tendon and 1-2ml of PRP was administered.
a) US image of the right knee shows a high grade partial thickness tear of the popliteus tendon at its femoral attachment (yellow arrow).
b and c) US images show needle tip (curved yellow arrow) within the tear site (yellow arrow).
References: Department of Radiology, VMMC and SJH, New Delhi, India
LATERAL MENISCUS:
The menisci are two fibrocartilaginous crescent-shape discs located between femoral condyles and proximal tibia playing a significant role in maintaining the complex biomechanics of the knee joint.[12,13] Fig. 30
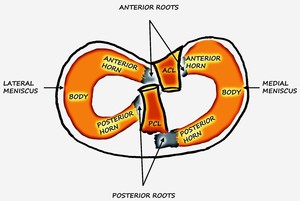
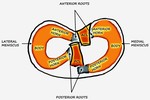
Fig. 30: LM: Schematic diagram of the tibial plateau showing the medial and lateral menisci and the anterior and posterior cruciate ligaments. ACL - Anterior cruciate ligament, PCL - posterior cruciate ligament.
References: Department of Radiology, VMMC and SJH, New Delhi, India
The lateral meniscus is nearly circular or O shaped and covers a larger portion of the tibial plateau surface than the medial meniscus.
There is no attachment of the lateral meniscus to the FCL.[14]
MENISCAL TEARS -
Three main types: Fig. 31 Fig. 32
- Vertical Longitudinal - Runs perpendicular to the tibial plateau and parallel to the long axis of the meniscus and divide the meniscus into central and peripheral halves
- Horizontal Longitudinal - Runs parallel to the tibial plateau and involves either one of the articular surfaces or the central free edge dividing the meniscus into superior and inferior halves.
- Radial - Runs perpendicular to both the tibial plateau and the long axis of the meniscus transecting the longitudinal collagen bundles as it extends from the free edge toward the periphery.
Displaced Vertical Longitudinal,
Horizontal Longitudinal and Radial tears are called bucket handle,
flap,
and parrot beak tears respectively.
A combination of two patterns is referred to as a complex tear.[15]
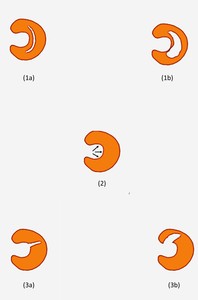
Fig. 31: LM TEAR: Schematic diagram showing the three major types of meniscal tears.
1a – Vertical longitudinal tear,
1b – Bucket handle tear (Displaced vertical longitudinal tear),
2 – Black arrows showing the direction of the Horizontal longitudinal tear,
3a – Radial tear,
3b – Parrot beak tear (Displaced radial tear)
References: Department of Radiology, VMMC and SJH, New Delhi, India
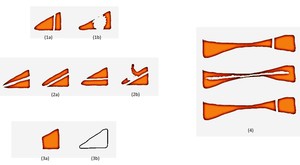
Fig. 32: LM TEAR: Schematic diagram showing the three major types of meniscal tears. (Figures 1-3 show the menisci in the vertical short axis view, Figure 4 shows the menisci in vertical long axis view.)
1a – Vertical longitudinal tear; 1b - Bucket handle tear (Displaced vertical longitudinal tear);
2a - Horizontal longitudinal tear; 2b – Flap tear (Displaced Horizontal longitudinal tear);
3a – Radial tear (Truncated meniscus); 3b Radial tear (Ghost meniscus);
4 – From top – bottom –
Vertical longitudinal tear, Horizontal longitudinal tear and Radial tear.
References: Department of Radiology, VMMC and SJH, New Delhi, India
SONOGRAPHIC FEATURES: Fig. 33 Fig. 34
- Linear or irregular hypoechoic clefts extending to the articular margins of the meniscus or through the meniscus.
- Sudden changes in the meniscal contour.
- Blunting of the medial surface.
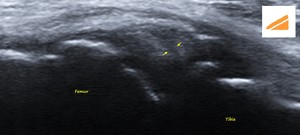
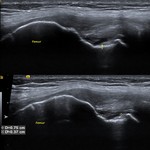
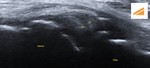
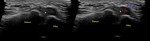
Fig. 33: LM - HORIZONTAL LONGITUDINAL TEAR: US image of the lateral knee in the coronal plane shows a hypoechoic linear cleft (yellow arrows) within the lateral meniscus, extending from its periphery up to its inferior articular surface.
References: Department of Radiology, VMMC and SJH, New Delhi, India
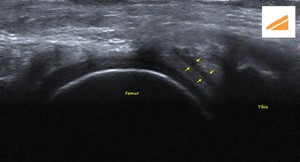
Fig. 34: LM - HORIZONTAL LONGITUDINAL TEAR: US image of the lateral knee of another patient, in the coronal plane, shows a hypoechoic linear cleft (yellow arrows) within the lateral meniscus, extending from its periphery up to its inferior articular surface.
References: Department of Radiology, VMMC and SJH, New Delhi, India
PARAMENISCAL/ MENISCAL CYSTS –
Meniscal cysts occur secondary to fluid extrusion from a meniscus tear.
SONOGRAPHIC FEATURES: Fig. 35
- They appear as anechoic cystic lesions superficial to the meniscus.
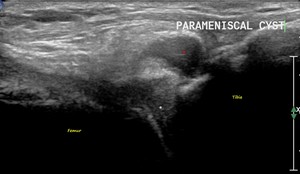
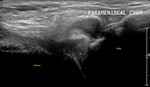
Fig. 35: PARAMENISCAL CYST: US image of the lateral knee in the coronal plane shows an anechoic cystic structure (red star) lateral to the lateral meniscus (white star).
References: Department of Radiology, VMMC and SJH, New Delhi, India
INTERVENTION: Fig. 36
- Cyst aspiration followed by S-LA injection.
[16]
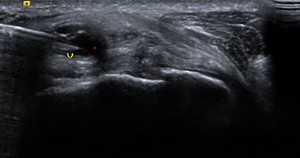
Fig. 36: PARAMENISCAL CYST - INTERVENTION:
A 42-year-old female patient presented with left lateral knee pain and swelling. US scan revealed presence of a parameniscal cyst.
Intervention - Using a 23G needle the target site was infiltrated with LA. The needle was then advanced into the parameniscal cyst and fluid was aspirated. After complete aspiration 2-3ml diluted Steroid-LA solution was administered within the cyst.
US image of the lateral knee shows an anechoic cystic structure (red star) lateral to the lateral meniscus with needle tip in situ (curved yellow arrow).
References: Department of Radiology, VMMC and SJH, New Delhi, India
MENISCAL EXTRUSION -
Meniscal tissue extending 3 mm or greater beyond the edge of the tibial plateau.
SONOGRAPHIC FEATURES: Fig. 37
- Projection of meniscus >3mm from the tibial plateau.[12]
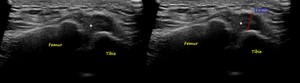
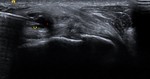
Fig. 37: MENISCAL EXTRUSION: US image of the lateral knee in the coronal plane shows hypoechoic meniscal tissue (white star) extending 5mm beyond the tibial plateau margin.
References: Department of Radiology, VMMC and SJH, New Delhi, India
PROCEDURAL CHECKLIST:
PRE - PROCEDURE -
Tests before the procedure:
- Blood tests for coagulopathy assessment including PT,
INR and platelets.
INR should be below 1.5.
- Triple Marker tests including HBsAg,
HCV and HIV.
Detailed sonographic examination of the target area including Doppler study before planning the needle trajectory.
Stringent sterile conditions must be followed:
- Cleaning the target area with 5% povidone‑iodine.
- Cleaning the site and transducer with a disinfectant.
- Sterile gloves are used and drapes may be applied to appropriately confine the area.
- Sterile probe covers can also be used if available.
Needle selection:
- Larger needles – 16-20 G are used for aspirating thick material like pus and blood.
- Smaller needles – 22-24 G are used for most other injections.
DURING THE PROCEDURE:
Most MSK procedures are performed using the in-line approach wherever feasible.
Procedures are usually performed under LA using diluted 2% lignocaine injected into the puncture site.
INJECTABLES USED:
Local Anaesthetics (LAs) - Most commonly used agents in musculoskeletal interventions acting as both therapeutic and diagnostic.
Lignocaine and Bupivacaine are commonly used.
Intraarticular injections may cause chondrolysis.
Most available LAs contain methylparaben as preservative,
which can be neurotoxic.
Therefore,
when performing perineural injections preservative‑free forms should be used.
Corticosteroids – Potent anti-inflammatory and pain modulating drugs.
Used in several MSK disorders including arthritis,
bursitis,
tenosynovitis,
tendinopathies,
entrapment neuropathies and ganglion aspirations.
Usually,
take 48‑72 hours to be effective and are therefore combined with LAs for a rapid onset of action.
Most commonly used corticosteroids are triamcinolone and methylprednisolone.
Side effects include – Post-injection flare,
chondromalacia,
tendon ruptures,
skin atrophy,
fat necrosis and skin depigmentation.
Platelet‑rich plasma – Created from an autologous blood sample through a platelet separation and concentration process.
It modulates tissue healing by a targeted release of growth factors.
PRP has both anti-inflammatory and pro-inflammatory effects that depend on the degree of platelet activation.
The most common side effect is injection site pain.
Prolotherapy - Uses locally irritant substances to stimulate growth factor production and fibroblast proliferation.
The most commonly used agent is hyperosmolar dextrose usually in a concentration of 25% mixed with saline.
POST‑PROCEDURAL INSTRUCTIONS:
- Rest for 48-72 hours.
- Local ice packs.
- Analgesics for steroid flares and SOS.
- Graded return to activity after 1-4 weeks depending on the underlying condition.
CONTRAINDICATIONS FOR THE USE OF MSK INJECTIONS:
- Local site infection.
- Allergy or hypersensitivity to the injectate
- Coagulopathies [4]