Introduction:
The pterygopalatine fossa (PPF) is a small space in the deep face that act as a neurovascular crossroad between the oral cavity,
nasal cavity,
nasopharynx,
orbit,
masticator space,
and the middle cranial fossa.
Therefore,
it needs to be evaluated very carefully during head and neck imaging,
since a myriad of neoplastic lesions can affect it.
These are difficult to detect clinically and to treat,
if not diagnosed accurately.
The multiple connections of the PPF with the neck spaces facilitate loco-regional spread of diseases.
Imaging anatomy,
contents,
and connections of the PPF
The PPF is an inverted pyramid-shaped space that is bordered anteriorly by the posterior wall of the maxillary sinus,
medially by the palatine bone and posteriorly by the pterygoid plates and its roof is formed by the sphenoid bone.
Contents:
1- Pterygopalatine ganglion (PPG)
2- Maxillary division of the trigeminal nerve (V2) and its branches
3- Vidian (pterygoid) nerve
4- Distal branches of the maxillary artery
5- Emissary veins
computed tomography (CT) is the modality of choice for evaluating the various bony communications of the PPF.
Connections of the PPF:
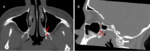
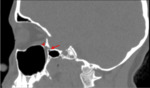
1-Palate via the greater and lesser palatine canals (Fig.1)
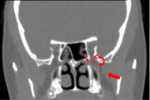
2-Infratemporal fossa (ITF) through the pterygomaxillary fissure (PMF)(Fig 2).
3-Nasal cavity via the sphenopalatine foramen (SPF) (Fig. 2)
4-Orbit via the inferior orbital fissure (IOF) (Fig. 2 and 5).
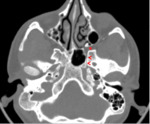
5-Foramen lacerum through the vidian canal (Fig.
3)
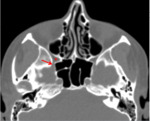
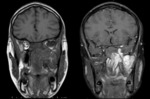
6-Middle cranial fossa through the foramen rotundum(Fig.
4 and 5)
Magnetic resonance imaging (MRI) is better for assessment of pathologies of the PPF,
especially perineural spread of tumors (PNS).
Key CT and MR imaging appearances in PPF pathology
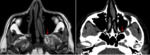
On non-contrast enhanced CT,
the PPF is seen normally as a hypodense space (Fig. 6).
On T1W MR images,
normal PPF shows hyperintense signal of fat (Fig.6).
It could show small flow voids (branches of the internal maxillary artery).
Mild post-contrast MR enhancement within the PPF is normal.
Infiltration of the fat with soft tissue lesions,
expansion of the PPF,
and erosion of its bony walls are indicators of its pathological involvement.
Widening of communicating neural foramina and/or infiltration of the fat within the neural foramina suggests PNS.
Bony abnormalities are best evaluated by CT whilst soft tissue infiltration of the fat is best evaluated on T1W MR images.
Contrast-enhanced T1W MR images,
especially with fat-saturation,
can demonstrate PNS within the PPF easily.
Neoplastic conditions:
The PPF can be infiltrated either by direct tumour invasion or by PNS.
Direct invasion of the PPF is usually noted in tumours of the nasal cavity and nasopharynx like juvenile nasopharyngeal angiofibroma (JNA),
nasopharyngeal carcinoma (NPC),
and masticator space sarcomas.
PNS usually occurs in a retrograde fashion,
toward the central nervous system.
PPF is often the site of PNS,
from cancers of the palate,
cheek,
maxillary sinus,
and nasopharynx.
Imaging is vital for diagnosing PNS as it may be clinically occult in about 40 % of patients.
The occurrence of PNS within the PPF has serious impact on treatment and prognostic.
Direct tumour invasion into the PPF
JNA:
JNA is a benign,
vascular,
locally aggressive tumour,
which originates at the SPF.
It occurs almost exclusively in males and in adolescence (~15 years).
It appear as lobulated soft tissue mass centered on the sphenopalatine foramen (which is usually expanded) Extensive bony destruction is usually not a feature,
but rather bone is remodelled or resorbed. Occurrence of lateral extension into the PPF is important,
because the PPF act as a portal allowing multidirectional invasion into the maxillary sinus anteriorly,
the ITF laterally via the PMF (Fig. 7),
the pterygoid fossa posteriorly,
and the orbit/cranial fossa superiorly via the IOF.
Moreover,
JNA can extend from the PPF further intracranially via the Vidian canal.
This multidirectional invasion of JNA is accompanied by higher morbidity.
NPC :
NPC is an aggressive primary malignancy arising in the nasopharyngeal mucosa.
It is commonly diagnosed between 40 and 60 years of age.
It appears as soft tissue masses mostly centered at the fossa of Rosenmüller.
It grows aggressively eroding the surrounding structures and destructing the surrounding bones.
Cervical lymph nodes assessment is critical due to common nodal involvement at the time of diagnosis.
The retropharyngeal nodes are usually the first affected.
However,
in third of cases,
these nodes are skipped,
and level II nodes are involved first
Masticator space sarcomas:
Mesenchymal tumours such as rhabdomyosarcoma (RMS),
fibrosarcoma,
etc.
are common primary tumours of the masticator space/ITF.
They are only seen in children.
Sarcomas of the masticator space can extend medially via the PMF and infiltrate the PPF,
which then allows further intracranial spread.
PNS to the PPF
Cancers of the palate
PNS from carcinomas of the palate usually occurs in retrograde fashion to the PPF via greater and lesser palatine nerves followed by further extension along V2 and the Vidian nerve into the middle cranial fossa and the cavernous sinuses.
Cancers of the maxillary sinus
Maxillary sinus tumors are known for PNS.
The PPF may be directly involved by the tumour through the posterior wall of the sinus or it may be infiltrated by PNS via the posterior superior alveolar nerve(s) and/or Infraorbital nerve via the Infraorbital fissure.
Cancers of the cheek
Cutaneous malignancies of the cheek like SCC and basal cell carcinoma can also extend perineurally to the PPF via branches of the Infraorbital nerve.
Potential pitfalls in imaging of the PPF
Infective and inflammatory conditions in the PPF may be confused with perineural spread of malignancy.
A schwannoma may also be confused with PNS by causing thickening and enhancement of the affected nerve.
Therefore,
clinical correlation is essential to look for sinusitis/mucormycosis,
etc.
Image-guided fine-needle aspiration of abnormal soft tissue may provide further evaluation in selected cases.