1.
Ovarian/adnexal related disorders:
1.1.
Follicular cysts:
During the first half of the menstrual cycle,
follicle-stimulating hormone (FSH) drives follicular enlargement.
One or more dominant follicles with a diameter of 18–25 mm emerge.
Acute pelvic pain may occur as the follicle grows by capsular compression, at the time of ovulation (Mittelschmer z phenomenon),
or after cyst rupture or hemorrhage.
Although these follicles are cystic,
it is appropriate to refer to them as follicles and reserve the term cyst for structures larger than 2.5–3.0 cm.
Follicular cysts often measure 3–8 cm in diameter and may remain hormonally sensitive.
|
US findings:
- Unilocular,
anechoic estructure with posterior through-transmission.
- Follow-up US on days 5–10 to verify their resolution is recommended.
Large follicular cysts may persist through several cycles.
CT findings:
- Well-defined round simple fluid collection (internal attenuation is generally less than 15 HU) with thin nonenhancing walls.
|
1.2. Cystic corpus luteum:
When implantation have occurred,
luteinizing hormone drives the transformation of the remaining follicular bed into the corpus luteum with marked neoangiogenesis of its granulosa cells (which predisposes the corpus luteum to hemorrhage).
The corpus luteum is maintained by β-hCG and normally regresses at the end of the first trimester.
The failure of the corpus luteum to involute or its hemorrhage may result in cystic enlargement.
|
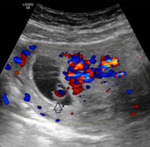
US findings:
- Thicker walls than those of follicular cysts and may be irregular.
- Anechoic or isoechoic content depending on the degree and age of hemorrhage.
- Color Doppler US depicts increased peripheral vascularity.
CT findings:
- Thinck and enhanced walls.
- High attenuation because of the presence of blood products.
|
1.3.
Hemorrhagic ovarian cysts:
It is the most frequent cause of acute pelvic pain in pre-menopausal women and one of the most frequent in pregnant women.
|
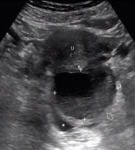
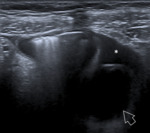
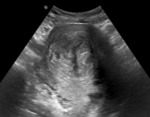
US findings:
- Complex mass with internal echoes and some degree of posterior through-transmission. Fig. 1
- Reticular pattern for the first 24 hours (this pattern is diagnostically specific).
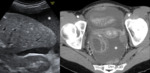
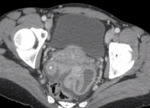
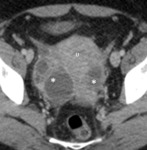
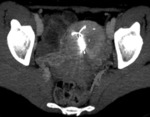
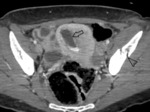
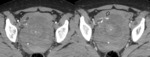
CT findings:
- Unilocular cyst with an internal attenuation of 25–100 HU.
- Fluid-fluid levels and hemoperitoneum may be present after cyst rupture. Fig. 2
|
1.4.
Endometritis (Endometriomas):
Endometriosis affects up to 10% of premenopausal women.
Ectopic endometrial tissue is estrogen sensitive,
and bleeds synchronously with the endometrium. As much as 80% of ectopic endometrial tissue is found in the ovaries and when large focal deposits of endometrial tissue are present,
these endometriomas are detectable at imaging.
In general,
it causes chronic pelvic pain,
associated with infertility.
|
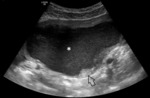
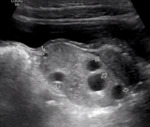
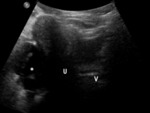
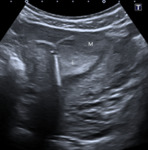
US findings:
- Uniform low-level echogenicity cytic mass (a “chocolate cyst” at gross examination). Fig. 3
- Multiple adjoining cystic structure in case of large endometriomas; and less commonly,
they appear solid.
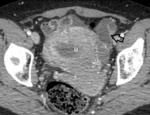
CT findings:
- Variable appereance; solid and cystic heterogeneous adnexal masses.
- The margins may be irregular,
with internal regions of low attenuation resulting from cyclical episodes of bleeding.
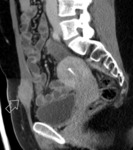
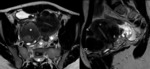
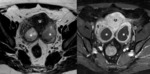
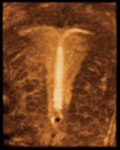
RM findings:
- The most reliable technique for its diagnosis.
- Hyperintense foci on T1-weighted sequences, not suppressión with spectral saturation of fat and hypotensity in T2-weighted sequences (shading). Fig. 4
|
There may be implantation in extraovarian sites such as the serosal surface of the uterus,
fallopian tubes,
urinary bladder,
ureters,
intestinal tract (it may result in intestinal obstruction) and abdominal wall (particularly,
in patients who have previously undergone abdominal surgery ( Fig. 5 ).
Rupture of the endometrioma and the ensuing blood products produce adhesions that may simulate pelvic inflammatory disease,
hemorrhagic cysts, or even malignancies.
Both US and CT findings have low specificity for the diagnosis of endometriomas.
Follow-up imaging is useful for differentiating endometriomas from pathologic entities such as hemorrhagic ovarian cysts,
which resolve,
and malignancies,
which progress.
1.5.
Ovarian torsion:
It represents 3% of gynecological emergencies.
Torsion occurs when the ovary becomes twisted on its vascular pedicle,
leads to the low-pressure conduits of the venous and lymphatic system become occluded.
Because ovaries receive a dual arterial supply (from the aorta via the ovarian artery and from the adnexal,
or ovarian,
branch of the uterine artery),
high-grade torsion is necessary to produce inflow occlusion.
Torsion is generally associated with the presence a benign adnexal mass.
However, it may occur in normal ovaries (most commonly in prepubertal girls).
Early diagnosis is essential to preserve the integrity of the ovary and allows for conservative management or sparing surgical intervention.
|
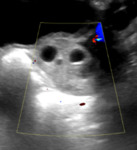
US findings:
- Enlarged ovary with central hyperechogenicity and enlarged (up to 25 mm in diameter) nonovulatory follicles at the periphery. Fig. 7
- As torsion progresses,
hypoechoic regions are observed due to hemorrhagic infarction.
- "Whirlpool sign" (swirling of the vascular pedicle).
- High resistance arterial flow and absent venous flow in Doppler images Fig. 8 .
However,
normal arterial flow do not rule out torsion.
- US scanning may depict the cyst (or,
less commonly,
the mass) that predisposed the ovary to torsion.
CT findings:
- Adnexal mass or enlarged ovary (up to 5 cm in diameter).
- Wall thickening to more than 3 mm in cystic adnexal masses.
- Additional findings are uterine deviation toward the affected side and ascites.
|
The overall accuracy of CT is inferior to that of US in the preoperative diagnosis of adnexal torsion.
1.6.
Ovarian hyperstimulation syndrome:
Ovarian hyperstimulation syndrome can occur at the early stages of pregnancy or within the luteal phase of the menstrual cycle in women undergoing an induction of ovulation treatment.
|
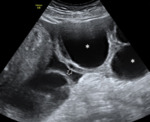
US and CT findings:
- Enlargement of both ovaries with multiple follicles of considerable size. Fig. 9
- Ascites and sometimes,
pleural effusion. Fig. 10
|
0,5-5% of cases reach a certain severity,
manifesting with oliguria,
tachypnea and hypotension.
The risk of adnexal torsion is increased and its diagnoses is challenging because ot the appearance of the ovaries in the ovarian hyperstimulation syndrome.
1.7.
Meigs syndrome: Fig. 11 Fig. 12
Meigs syndrome is the association of a ovarian fibroma or fibrothecoma with ascites and pleural effusión.
Whereas Meigs pseudosyndrome is the association of other benign ovarian tumors with ascites and pleural effusión.
1.8.
Ovarian vein thrombosis (or thrombophlebitis): Fig. 13
It occurs most frequently in postpartum patients but may occur following pelvic surgery,
pelvic trauma,
pelvic inflammatory disease or complicate treatment of tumors with chemotherapy.
In 80-90% of cases,
the right ovarian vein is involved (due to retrograde flow in the left vein).
The diagnosis can be reached with US imaging,
but CT facilitates its visualization.
|
CT findings:
- Tubular structure with an enhancing wall and low attenuation thrombus in the expected location of the ovarian vein.
- This finding should not be confused with hydroureter,
acute appendicitis,
or a thrombosed inferior mesenteric vein.
|
2.
Pelvic inflammatory disease (PID):
Group of infectious conditions of the upper reproductive tract,
including endometritis,
salpingitis,
and tuboovarian abscess. It is typically cause by an ascending lower tract infection,
although hematogenous spread and direct extension of an infection are also possible.
Neisseria gonorrohoeae and Chlamydia trachomatis are the germs involved in two-thirds of cases,
but polymicrobial infection also has been reported.
The typical syntom is aching pain usually 7–10 days after menstruation.
At the early stages of the infection,
US and CT findings may be normal.
2.1.
Endometritis:
Endometritis is the most common cause of postpartum fever.
|
US findings:
- Heterogeneous thickening of the endometrial band
- Increase of endometrial vascularization.
- Echogenic foci inside the endometrial cavity (it represents gas or detritus).
This finding can support the diagnosis,
unless there has been recent instrumentation or the patient recently gave birth.
CT findings:
- Endometrial cavity is thickened and distended with fluid.
- Associated inflammation in the parametrial soft tissues.
|
Because fluid within the endometrial canal may mimic a gestational sac,
this finding should be correlated with the β-hCG level.
2.2.
Salpingitis: Fig. 14 Fig. 15 Fig. 16Fig. 17
CT findings are often normal or demonstrate a small amount of fluid in the cul-de-sac.
Salpingitis may progress to hydrosalpinx or pyosalpinx if left untreated.
In pyosalpinx,
US images show fluid with echogenic debris distending the fallopian tubes.
At later stages,
tuboovarian abscesses may form.
2.3.
Tubo-ovarian abscess: Fig. 18 Fig. 19
Involvement is often bilateral. Although US is the primary imaging modality,
CT can be a helpful adjunct in determining the extent of disease and identifying associated complications.
|
CT findings:
- Complex fluid-attenuation collections with thick septations and thickened and irregularly enhancing walls.
- Serpiginous structure corresponding to a dilated,
pus-filled fallopian tube.
- Internal gas bubbles are the most specific radiologic sign of abscess but are unusual in tubo-ovarian abscess.
- Associated findings include thickening of the uterosacral ligaments,
increased attenuation of the presacral fat secondary to edema,
hydronephrosis and indistinct margins of adjacent bowel loops.
- Anterior displacement of the broad ligament because of the posterior position of the mesovarium may allow differentiation of a tuboovarian abscess from a pelvic abscess of other origin.
|
3.
Uterine related disorders:
3.1.
Misplaced IUD:
The US and CT appearances of Intrauterine device (IUD) vary according to the type of device.
However,
a T-shaped device is the most common within the uterus Fig. 20 .
Perforation into or through the myometrium may occur in approximately 0.1% of cases as a complication of IUD placement.
When perforation occurs,
hemorrhage and free pelvic fluid are possible,
with associated pelvic pain.
|
US and CT findings:
- The finding of an IUD (well defined structure, hyperechoic at US,
and hyperattenuating at CT) within the myometrium is highly suggestive of perforation. Fig. 21 Fig. 22
|
3.2.
Fibroid pathology:
Fibroids or leiomyomas are the most common tumors of the uterus.
The location,
in order of decreasing frequency,
is: 1) intramural,
2) subserosal and 3) submucosal.
Multiple forms of benign degeneration (hemorrhagic,
cystic,
myxoid) may occur when the fibroid outgrows its blood supply,
causing pelvic pain.
Less commonly,
it is presented as vaginal bleeding.
Sarcomatous degeneration to leiomyosarcoma is rare,
occurring in less than 0.1% of cases.
Pregnancy predispose to hemorrhagic or red degeneration of a uterine fibroid,
generally before 10 weeks of gestation.
US findings are usually diagnostic. CT is not the primary modality for evaluating fibroids; however,
fibroids are often found incidentally at CT.
|
US findings:
- Solid uterine mass with minimal echotexture.
Howerver,
heterogeneity may result from necrotic degeneration. Fig. 23
- Calcifications in a uterine mass are the most specific sign for a leiomyoma (however,
these occur in only 10% of cases).
CT findings:
- Uterine enlargement with associated solid soft-tissue mass.
- Uterine contour deformity caused by fibroids that extend beyond the mucosal or serosal layer.
- Cystic appearance and central region of low attenuation are suggestive of internal degeneration.
|
4.
Not known pregnancy:
4.1.
Gestational sac: Fig. 24 Fig. 25
The gestational sac is the first sign of early pregnancy.
It can be an incidental finding in premenopausal women.
In a woman with a positive beta-hCG,
any intrauterine sac-like fluid colletion seen o US is highly likely to be a gestational sac.
4.2.
Ruptured ectopic pregnancy: Fig. 26
Ectopic pregnancy is always a consideration in women of reproductive age with acute pelvic pain and with a positive β-hCG level.
Risk factors of ectopic pregnancy are previous ectopic pregnancy,
Fallopian tubal disorders (including tubal injury,
surgery and ligation),
DIU,
history of PID,
infertility treatments,
smoking,
maternal age.
Location of ectopic implantation,
in order of decreasing frecuency:
- Tubal ectopic (93-97%),
most common ampullar ectopic.
- Cornual ectopic (3-4%).
- Ovarian ectopic 0,5-1%).
- Cervical ectopic (1%).
- Scar ectopic of previous Cesarian section scar (1%).
- Abdominal ectopic (1%).
In case of rupture,
the clinical state can reach a certain severity,
even with hemodynamic inestability.
|
Imaging findings:
- Empty uterine cavity or no evidence of an intrauterine pregnancy.
- Pseudogestional sac (small amount of intrauterine fluid,
centrally located in the endometrial cavity) and decidual cysts.
- Complex extra-adnexal cyst or mass (intra-adnexal cyst or mass is more likely to be a corpus luteum).
- Signs of extrauterine pregnancy (only seen in a minority of cases).
- Free pelvic fluid or hemoperitoneum.
|