Magnetic resonance imaging (MRI) has an important role in the detection and characterization of focal,
diffuse liver diseases and biliary tract pathology.
Contrast agents improve the detection of focal liver lesions by increasing the lesion-to-liver contrast.
Some contrast agents have special properties for example that they are excreted in the biliary tract and thus provide useful anatomic and functional evaluation of the biliary tree.
Gd-EOB-DTPA (Primovist) is one of the hepatocyte specific contrast agents designed to evaluate liver lesions in MRI.
After intravenous administration,
Gd-EOB-DTPA is distributed in the extracellular space,
in healthy subjects approximately 50% of the administered dose is transported through the hepatocytes and excreted into the bile.
Gd-EOB-DTPA transport in the hepatocytes is mediated by two different transport systems located at the sinusoidal and canalicular membranes of the cell.
The contrast agent enters the hepatocytes through the organic anion transporting polypeptides OATP1B1 and OATP1B3 which belong to the solute carrier transporter superfamily of the OATPs (SCTO).
Following transport through the hepatocytes,
it is excreted into the bile via the multidrug resistance protein 2 (MRP2),
which belongs to the ATP-binding cassette C (ABCC) transporter subfamily.
The other 50% of the contrast agent that is not cleared by the hepatobiliary system is excreted by glomerular filtration in the kidneys.
Gd-EOB-DTPA can provide information regarding lesion vascularity in the early arterial and venous phases and regarding hepatocyte presence and function in the delayed hepatobiliary phase performed 20min after injection.
Generally,
hepatobiliary-specific agents have a higher cost than nonspecific extracellular fluid agents,
this cost if often countered by the additional information obtained from the study,
which can help us avoid the need for other imaging studies,
follow-up,
biopsy,
or even surgery.
Suggested MRI protocol:
The usual MRI protocol of Primovist is as follows:
Axial T1-weighted in- and opposed-phase gradient echo
Axial and coronal T2-weighted FS fast spin echo
Aixal and coronal T2-weighted cholangiopancreatography
- · Contrast agent injection:
0.1ml/kg.
3D axial T1-weighted fat suppressed gradient echo
- · Hepatobiliary phase imaging
- Time of imaging(min)
Varies usually about 45-60 minutes.
Biliary phase is usually obtained at 25min.
- Parenchymal assessment and lesion detection/characterization
Axial T1-weighted fat suppressed
Without contrast
Arterial phase
Portal venous phase
Optional delayed imaging at 3min
Biliary excretion phase at about 25 min
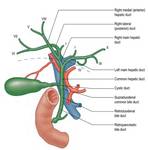
Normal Biliary tree anatomy:
The biliary tree is divided into intra-hepatic and extra-hepatic bile ducts.
There is significant variability in the biliary tree among individuals,
the classical description is present in approximately 60% of the population.
Intrahepatic Ducts:
Bile canaliculi unite to form segmental bile ducts which drain each liver segment.
The segmental ducts then combine to form sectional ducts with the following pattern: segments VI and VII: right posterior duct (RPD),
segments V and VIII: right anterior duct (RAD).
The right posterior and anterior ducts unite to from the right hepatic duct (RHD).
Segmental bile ducts from II-to-IV unite to form the left hepatic duct (LHD).
The left and right hepatic ducts unite to form the common hepatic duct (CHD). Bile duct(s) from segment I drain at their union.
Extrahepatic Ducts:
The common hepatic duct is joined by the cystic duct from the gallbladder to form the common bile duct.
The common bile duct joins with the main pancreatic duct to form the ampulla of Vater,
which drains at the major duodenal papillae located on the medial wall of the duodenum (Fig 1).