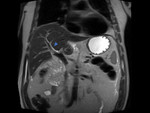
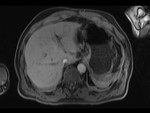
T2- weighted MR cholangiography is a well-known method of studying the biliary system,
but there are cases in which there is a need for a functional and detailed anatomy study that is not possible with conventional techniques.
In this case T2- weighted MR cholangiography (MRC) in conjunction with EG-3D T1 Fatsat Gd-EOB-DTPA enhanced MRI can provide the required information.
Contrast enhanced cholangiography MRI is also useful in the evaluation of different types of biliary tract pathology like assessment of bile duct obstruction,
detection of bile duct injury,
leakage and stricture,
liver failure and post procedure evaluation.
We will provide examples below based in our experience using Primovist in different clinical settings.
Benign biliary strictures:
In about 95% of the cases these arise from surgical injury from procedures such as laparoscopic cholecystectomy,
hepatic resection,
liver transplantation and biliary enteric anastomosis.
Other causes include trauma,
inflammation from choledocholithiasis,
ischemia involving the hepatic artery and primary sclerosing cholangitis (PSC).
A benign stricture usually involves a short segment,
with a regular margin and symmetric narrowing.
Contrast enhanced MRC can show the extent and location of the stricture.
Biliary leakage:
Biliary leakage is a serious complication in hepatobiliary surgery.
Considerable morbidity and mortality are associated with this process therefore early diagnosis is important.
Studies like ultrasound,
computed tomography (CT) and MRC can detect fluid collections and provide non-specific findings to biliary leakage,
but theses studies can't identify their content or if there is communication with the biliary tree.
Invasive methods such as Endoscopic Retrograde Cholangiopancreatography (ERCP),
Percutaneous Transhepatic Cholangiography (PTC) or intraoperative cholangiogram,
that are used to identify and possibly treat the leak,
but they carry the risk that involves every invasive procedure.
MRI cholangiography using hepatocyte-specific contrast agents like Gd-EOB-DTPA,
are non-invasive and allow us to visualize an active bile leakage.
Communication with the biliary tree can be established by the visualization of contrast material in fluid collections (biloma) or outside the biliary ductal system and duodenum on delayed phase imaging.
This information helps us identify the type of bile duct injury and gives us important anatomical and functional information which can help orientate treatment.
Evaluation of liver function:
In a healthy patient,
an optimal hepatocellular phase can be obtained after 10 minutes,
but in a cirrhotic patient it can take up to 20 minutes.
Because Gd-EOBDTPA uptake is mediated by the same transporter responsible for bilirubin transport,
we can suspect biliary obstruction or diminished hepatobiliary function in patients with reduced or no visualization of the biliary system after 30 minutes.
Case 1:
A 43-year-old male patient with cirrhotic alcoholic liver disease and impaired renal function that required hepatic transplant (April 2017) and a mild transplant rejection treated with an increase of immunosuppression; because of altered hepatic function and signs of cholestasis an MRC was performed on May 2018.
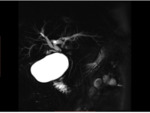
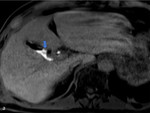
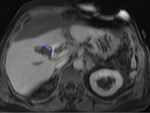
The initial MRC revealed dilatation of intrahepatic biliary ducts and of the common hepatic duct because of stenosis of the anastomosis of the common hepatic duct of the donor with the bile duct of the receptor.
The MRC also showed a large 9.3cm subhepatic,
encapsulated collection (Fig 2).
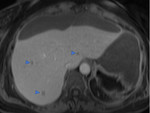
A contrast enhanced MRC was performed.
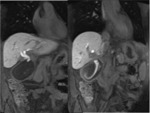
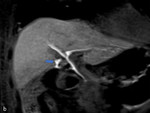
This second study revealed transit of contrast,
during the biliary excretion phase,
from the common hepatic duct to the collection,
confirming the suspicion of a biloma (Fig 3).
Case 2:
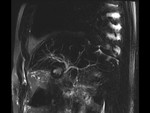
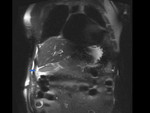
A 33-year-old patient with a total gastrectomy because of a gastric carcinoma and a history of dehiscence of the esofagus-yeyunal anastomosis has high debit in a left sided drainage,
therefore a biliary leak is suspected.
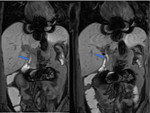
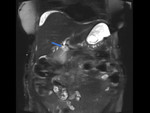
Initial MRC reveals a non-dilated biliary tree and no apparent collections.
After contrast administration during the delayed phases contrast has a normal transit through the biliary tree,
with no evidence of leakage (Fig 4).
Case 3:
An 85-year-old patient has a complicated cholecystectomy with a vascular lesion.
The presence of biliary content in a drainage rises the suspicion of biliary leakage.
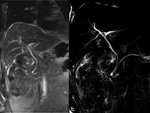
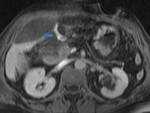
Initial MRC reveals a non-dilated biliary tree and no apparent collections (Fig 5).
After hepatobiliary-specific contrast administration during the delayed phases contrast is seen accumulating in the vesicular fossa and outside of the biliary tree confirming leakage (Fig 6,7).
A ERCP is performed confirming the leak of the cystic duct.
Case 4:
A 68-year-old female patient is suspected of having a high debit biliary leak following a total duodenopancreatectomy because of a tumour in the uncinate process.
Initial studies revealed a non-dilated biliary tree,
the biliary ansatomosis and a moderate amount of perihepatic fluid (Fig 8).
A contrast enhanced hepato-biliary MRC demonstrates contrast leakage from the biliary-enteric anastomosis(Fig 9,10).
Contrast enhanced T1 axial MRI also revealed several new hipovascular well defined non-enhancing lesions compatible with metastasis distributed thought the liver (Figure 11).
Case 5:
A 65-year-old male patient with a solitary kidney and a total pancreatectomy because of pancreatic metastasis due to renal carcinoma,
has a complicated postsurgery; with renal failure and a low debit biliary leak and signs of cholestasis.
A hepato-biliary specific contrast enhanced MRC is performed to evaluate the biliary-enteric anastomosis. Initial sequences reveal a nondilated biliary tree,
small amount of perihepatic fluid and periportal edema (Fig 12,13,14).
85 minutes after hepatobiliary-specific contrast administration,
no contrast is excreted to the biliary tree.
(Fig 15).
These findings suggest liver failure,
which is later corroborated clinically and through laboratory testing.
The patient suffered renal and multicausal liver failure with cholestasis,
without signs of cytolysis,
ascites,
or encephalopathy.
The patient has a good outcome after conservative treatment.