WHAT IS POST TB SEQUELAE?
These are the radiological changes in the chest which are secondary to complications of primary or secondary pulmonary TB.
These changes may vary from mild to severe.
Complications of TB after treatment completion can often be misinterpreted for another active disease so it is important that we recognize and understand the radiologic manifestations of the thoracic sequelae.
Some residual changes can be compatible with life and not cause any symptoms such as calcified mediastinal lymph nodes and mild pleural fibrosis,
however,
few changes can be debilitating such as cicatrization collapse and fibrothorax.
Post TB sequelae can be categorized into parenchymal,
airway disease,
pleural/chest wall,
vascular and mediastinal.
Details are given in (Table 1)
PATHOPHYSIOLOGY OF PULMONARY TB:
Tuberculosis is an infectious disease which spreads from human to human by airborne transmission.
(Fig.
1) The infection can be either primary,
latent or reactivated TB.
Primary pulmonary infection can be accompanied by lymphohematogenous seeding of many organs,
and reactivation may occur as early as three months or many years after initial infection.
The risk of reactivation of tuberculosis is greatest in the year after infection,
declining sharply thereafter for most patients.
The course of the disease depends on the interaction between the host response and the virulence of the organism.
The major host defense against the tubercle bacillus is cell-mediated immunity,
by means of macrophages and T lymphocytes.
When host factors prevail,
there is gradual healing with formation of parenchymal scars.
When the organism overpowers host defenses,
the disease progresses,
either locally or in other parts of the lung or body after spread of bacteria via the airways,
lymphatic vessels,
or bloodstream.
More fulminant course is expected in an immunocompromised host.
Therefore,
various forms of sequelae and complications may result from both primary and post primary pulmonary tuberculosis.
RADIOLOGICAL MANIFESTATIONS OF POST TB SEQUELAE:
PARENCHYMAL:
Tuberculoma: (Fig.2)
These may be a manifestation of either primary or postprimary tuberculosis.
These present radiologically as rounded soft tissue densities which are rarely seen on chest X ray but are easily visualised on CT.
They may be solitary or multiple with wide range of size from a few millimiters to more than 4 cm.
They usually have smooth margins with calcification in upto 20-30%.
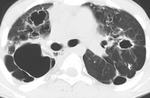
Thin walled cavity: (Fig.3)
These may be seen in both active and inactive disease.
Serial imaging helps determine the stability or activity of pulmonary disease.
The wall of a chronic cavity varies from 1 cm to less than 1 mm in thickness and may be smooth,
sometimes simulating an emphysematous bulla.
It can be difficult to distinguish true cavities from bullae,
cysts,
or pneumatoceles.
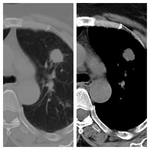
Cicatrization collapse: (Fig.4)
This is a common finding after postprimary tuberculosis.
Complete destruction of a whole lung or a major part of a lung is common in the end stages of tuberculosis.
Such damage results from a combination of parenchymal and airway involvement.
It may result from a progressive primary infection or from postprimary tuberculosis with a prolonged process of cavitation,
spread to new areas,
and subsequent fibrosis.
Radiologically this presents as an area of alveolar destruction with loss of lung volume and ipsilateral mediastinal shift.
It is more often unilateral more than bilateral.
Once the lung is destroyed,
the activity of tuberculosis is difficult to assess with radiologic studies.
Aspergilloma: (Fig.5)
The residual tuberculous cavities post treatment may be a source of colonization of superadded organisms such as fungal ball.
This presents radiologically as the ‘air crescent sign’ with a soft tissue density in the cavity which moves with change of body position.
It may be asymptomatic or present with hemoptysis.
Bronchogenic Carcinoma: (Fig.6)
Although rare it may develop in tuberculous scar tissue.
It may also be a parallel finding along with pulmonary TB or it may be an underlying cause for reactivation of latent TB due to the immunocompromised status of the patient.
Radiolograhically it manifests as an abnormally enhancing soft tissue mass lesion which may present on the background of old TB changes.
AIRWAY DISEASE:
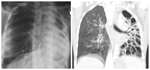
Bronciectasis: (Fig.7,
Fig.
8))
This is a common finding in post TB sequelae and it occurs by destruction and fibrosis of the lung parenchyma with irreversible secondary bronchial dilatation (traction bronchiectasis).
It can occur with both primary or secondary exposure.
Bronchiectasis located in the apical and posterior segments of the upper lobe is highly suggestive of a tuberculous origin.
Tracheobronchial stenosis:
May be caused by granulomatous changes in the tracheobronchial wall or by extrinsic pressure from enlarged peribronchial lymph nodes.
Stenosis begins as simple erythema and edema with extensive granulation tissue destroying and replacing the mucosa and submucosa and subsequent fibrosis may result in tracheobronchial narrowing.
The left main bronchus is most frequently involved in fibrotic disease.
On CT scans,
irregular luminal narrowing with wall thickening,
enhancement,
and enlarged adjacent mediastinal nodes are common findings.
Broncholithiasis: (Fig.
9)
This is an uncommon complication of pulmonary tuberculosis and is defined as the presence of calcified or ossified material within or just adjacent to the lumen of the tracheobronchial tree. Radiographic manifestations include a change in the position or disappearance of a calcific focus on serial radiographs or development of airway obstruction,
resulting in lobar or segmental atelectasis,
mucoid impaction,
or expiratory air trapping.
CT shows a calcified lymph node that is either endobronchial or peribronchial and is associated with findings of bronchial obstruction,
such as atelectasis,
obstructive pneumonitis,
or bronchiectasis.
(Fig.8)
PLEURAL/CHEST WALL:
Pleural thickening with calcification: (Fig.10)
Tuberculous pleuritis usually resolves completely even in the absence of treatment,
however,
in some patients,
chronic complications occur during the healing of the tuberculosis lesions or appear as late sequelae such as pleural thickening and pleural calcification.
It is usually asymptomatic but may also present with discomfort while breathing.
CT shows pleural thickening and specks of calcification which are usually focal and unilateral but may be bilateral.
Empyema: (Fig.
11)
Pleural infection is usually caused by rupture of a subpleural caseous focus into the pleural space; and it progresses to become chronic tuberculous empyema,
which is persistent,
grossly purulent pleural fluid containing tubercle bacilli which are difficult to culture.
CT scans show a focal fluid collection with pleural thickening and calcification and with or without extrapleural fat proliferation.
Chyliform or pseudochylous pleural effusion is most commonly caused by tuberculous empyema.
The diseased pleura may result in an abnormally slow transfer of cholesterol and other lipids,
originating from degenerated red and white blood cells,
out of the pleural space and lead to accumulation of cholesterol in the pleural fluid.
CT shows a fat-fluid or fat-calcium level.
Fibrothorax: (Fig.12,
Fig.13)
This is a medical condition characterised by scarring (fibrosis) of the pleural space surrounding the lungs that is severe enough to cause reduced movement of the lung and ribcage.
On CT it manifests as diffuse pleural thickening but without effusion suggesting inactivity.
Patients with diffuse pleural thickening should be closely monitored for the development of restrictive lung disease with serial pulmonary function tests.
Bronchoplueral fistula: (Fig.14)
Bronchopleural fistula associated with tuberculosis is either spontaneous,
secondary to trauma or a surgical procedure.
High mortality can result from both the acute and chronic phases.
The diagnosis is based on an increasing amount of sputum production,
air in the pleural space,
a changing air-fluid level,
and contralateral spread of pneumonic infiltration.
CT can demonstrate the sites of communication between the pleural space and either one or more airways or the lung parenchyma in patients with bronchopleural fistula with an air fluid level in the fluid cavity.
Pneumothorax: (Fig.15,
Fig 16)
It occurs in approximately 5% of patients with postprimary tuberculosis,
usually in severe cavitary disease but rarely in miliary tuberculosis.
It is usually caused by the pleural caseous infiltrates which liquefy resulting in pleural necrosis and rupture.If any apical abnormality is seen after reexpansion of a spontaneous pneumothorax,
active tuberculosis should be considered.Tube drainage is the treatment of choice.
VASCULAR COMPLICATIONS: (Fig.17)
Pulmonary arteries and veins in an area of active tuberculous infection may demonstrate vasculitis and thrombosis.
Bronchial arteries may be enlarged in bronchiectasis associated with tuberculosis or in parenchymal tuberculosis itself.
In patients with bronchiectasis,
nodular and tubular structures with an appearance unlike that of lymph nodes or normal vessels in the mediastinum and around the central airway on high-resolution CT scans are suggestive of hypertrophied bronchial arteries.
This is important to diagnose so as to avoid a biopsy of the vessel.
Rasmussen aneurysm is a rare phenomenon caused by weakening of the pulmonary artery wall from adjacent cavitary tuberculosis.
Hemoptysis is the usual presenting symptom and may be life-threatening when it is massive.
Progressive weakening of the arterial wall occurs as granulation tissue replaces both the adventitia and the media.
The granulation tissue in the vessel wall is then gradually replaced by fibrin,
resulting in thinning of the arterial wall,
pseudoaneurysm formation,
and subsequent rupture.
MEDIASTINAL:
Calcified lymph nodes: (Fig.18)
The incidence of mediastinal lymphadenopathy is the highest during childhood and it decreases with increasing age.
It is observed that with anti-tubercular treatment,
the nodes may either disappear or form a residual mass composed of fibrotic tissue and calcifications.
Fibrosing mediastinitis: (Fig.19)
It involves excessive fibrosis in the mediastinum.
Tuberculous mediastinitis progresses insidiously without significant clinical symptoms and may result in mild symptoms,
including cough and low-grade fever,
and symptoms due to compression of the superior vena cava,
esophagus,
and tracheobronchial tree.
The radiographic findings include mediastinal widening or a localized mass.
CT findings include a mediastinal or hilar mass,
calcification in the mass,
tracheobronchial narrowing,
pulmonary vessel encasement,
superior vena cava obstruction,
and pulmonary infiltrates.
Bronchial obstruction secondary to fibrosis may result in obstructive pneumonia or atelectasis.
Pericardial TB: (Fig.20)
Tuberculous pericarditis is very rare and reported in up to 1% of cases of tuberculosis.
Pericardial involvement is commonly caused by extranodal extension of tuberculous lymphadenitis into the pericardium because of the close anatomic relationship between the lymph nodes and the posterior pericardial sac.
At CT,
lymphadenopathy and pericardial thickening with or without effusion may be seen.
Constrictive pericarditis occurs in about 10% of patients with tuberculous pericarditis.
It is characterized by fibrous or calcific constrictive thickening of the pericardium,
which prevents normal diastolic filling of the heart.
CT shows pericardial thickening of more than 3 mm with or without pericardial effusion.