In our study,
we evaluated a great number of ependymoma cases,
with initial complain of CNS masses,
confirmed by anatomopathological studies.
Although the main imaging test for evaluation of central nervous system tumors is magnetic resonance with contrast,
in the beginning of the symptoms many patients undergo cranial CT,
mainly due to accessibility.
- General features (Table 1):
Ependymomas are heterogeneous expansive masses that generally have the same imaging characteristics at CT and MRI.
The solid component of the lesions is iso/hypoattenuating to surrounding normal brain tissue at unenhanced CT,
coarse calcification and cystic areas are common (both present in 50% of cases) and variable content of hemorrhage.
After contrast administration,
there is heterogeneous enhancement.
On MRI,
the solid portions are isointense to hypointense relative to white matter in T1WI,
hyperintense in T2WI and foci of blooming from hemorrhage or calcification are seen in T2*WI.
The signal intensity is heterogeneous within the tumor,
due to the large number of components: cystic areas with fluid signal intensity,
calcifications and old hemorrhage.
There is usually avid and heterogeneous enhancement of the soft tissue components on T1WI post gadolinium.
The enhancement is useful in differentiating tumor from adjacent vasogenic edema and normal brain parenchyma.
Restricted diffusion may be seen in solid components,
especially in anaplastic subtype.
Spectroscopy demonstrate a choline peak elevation according to the cellularity of tumor,
reduction in N-acetylaspartate,
elevated Choline/Creatine ratio and raised lipid and lactate when degeneration occurs.
Microscopically,
these tumors are characterized by well-differentiated cells.
Characteristic features include ependymal rosettes,
which are uncommon but pathognomonic and perivascular pseudorosettes, which are more common and seen in most of ependymomas.
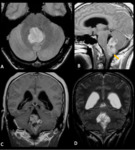
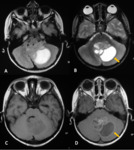
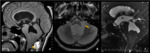
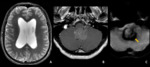
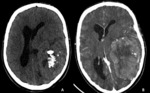
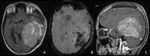
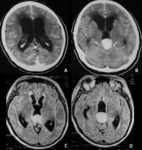
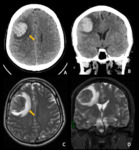
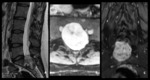
- Infratentorial ependymomas (Figures 1 – 4):
The infratentorial ependymomas tend to present in posterior fossa,
more commonly in the pediatric age group (mean age at diagnosis is 6 years).
At the time of clinical presentation,
they usually fill and distend the fourth ventricle,
determining hydrocephalus and increased intracranial pressure.
Approximately 70% of intracranial ependymomas are infratentorial,
arising from the lateral recess or from the midline inferior floor of fourth ventricle,
near the obex.
They usually extend through the foramina of Luschka into the cerebellopontine angle and/or inferiorly through the foramen of Magendie into the posterior aspect of upper cervical cord.
This characteristic of plasticity can be seen on both CT and MRI and represents a highly typical feature of this tumors,
but is not pathognomonic (a few medulloblastomas can extend through the fourth ventricular exit foramina).
In addition to the classic appearance of a fourth ventricular mass,
infratentorial ependymomas can also present as expansive lesion in cerebellopontine angle.
Ependymomas arising from a location not in the midline may have a worse prognosis,
perhaps due to involvement of critical structures such as cranial nerves.
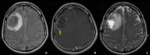
- Supratentorial ependymomas (Figures 5 – 9):
Approximately 30% of intracranial ependymomas are supratentorial and generally manifests in older age group (mean age at diagnosis vary from 18 to 24 years).
These tumors are most commonly located in the brain parenchyma than the infratentorial ependymoma,
so the patients tend to present with focal neurologic deficits,
headache and seizures,
having a better prognosis than posterior fossa counterpart.
Supratentorial ependymomas may be intraventricular or intraparenchymal.
Intraventricular tumors present as well-circumscribed masses that usually fill the ventricular lumen and occasionally may extend into the adjacent brain parenchyma.
They generally arise along the surfaces of the lateral ventricles or along the septum pellucidum.
Third ventricular ependymomas are rare.
Intraparenchymal lesions are believed to arise from trapping of embryonic rests of ependymal tissue in the developing cerebral parenchyma.
They are usually large and often contain cystic components (while infratentorial ependymomas are often more solid tumors).
This may occur due to delayed clinical symptoms and larger size at the time of diagnosis.
A variable appearance of the tumor is also described,
varying from completely solid enhancing masses,
cysts with a mural nodule or more heterogeneous masses.
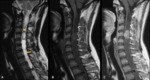
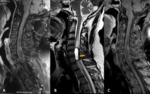
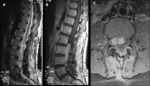
- Spinal ependymomas (Figures 10 – 14):
Spinal ependymomas are the most common spinal cord tumor,
seen both in adult and pediatric population.
In adults they are the most prevalent intramedullary neoplasm,
comprising 60% of all glial spinal cord tumors,
with the peak incidence is in the fourth decade (39 years being the mean age at presentation).
Males are more frequently affected than females.
In children,
they are the second most common intramedullary neoplasm,
representing 30% of pediatric spinal tumors.
Intramedullary ependymomas are believed to arise from ependymal cells that line the central canal of medulla and occur most commonly in the cervical region.
Cysts are a common feature,
most of them are polar (nontumoral).
About 20% of ependymomas demonstrated the “cap sign”,
a rim of extreme hypointensity seen at the poles of the tumor on T2WI.
This finding is thought to be secondary to hemorrhage,
with hemosiderin deposition,
and is highly suggestive of ependymoma.
Syringohydromyelia is also quite variable presentation,
occurring up to 50% of cases.
These tumors are characterized by slow growth and tend to compress adjacent spinal cord tissue.
As most primary intramedullary tumors,
there is usually a long antecedent history before the diagnosis is established.
The patients typically present back or neck pain,
sensory deficits,
motor weakness or bowel or bladder dysfunction.
Sensory symptoms are frequent presentations and may be explained by the proximity of these centrally located tumors to the spinothalamic tracts.
In the case of spinal ependymomas,
it is important keep mind the increased relation with neurofibromatosis type 2.
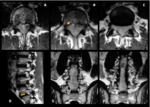
The myxopapillary subtype constitutes about 13% of all spinal ependymomas and tends to have an earlier clinical presentation (mean age at 35 years),
frequently seen in male patients.
This mucoid tumor has a distinct predilection for the conus medullaris or filum terminale and represent the most common neoplasm in this region (83% of cases).
Occasionally,
they occur in the extradural space,
probably arising from the coccygeal medullary vestige at the distal portion of the neural tube.
Myxopapillary ependymomas usually manifest with lower back,
leg or sacral pain and weakness or sphincter dysfunction.
Although most of these tumors are slow growing,
those located near the sacrum may be more aggressive,
creating large lytic areas of bone destruction.