We present common and not common appearance of several types of PID on CT and MRI imaging.
CT and MRI were performed in our hospital with patients at age from 20’s to 80’s who were suspected PID
They were confirmed PID clinically or pathologically.
Our case presentation is listed in a Table including TOA with IUD insertion or without IUD insertion,
infected endometriotic cyst with prominent wall thickening or with slight wall thickening,
pyosalpinx under steroid medication,
chronic pyosalpinx caused by chlamydial infection,
pyometra,
infected myoma replaced uterus with abscess formation associated with severe diabetes mellitus.
As a case of mimicking PID,
degenerating uterine leiomyoma was added.
To remind ovarian malignancies overlapping PID clinically and radiographically,
we also presented one case of seromucinous borderline tumor of the ovary (Table 1).
Case 1. (Fig.6) TOA
40’s female with fever and abdominal pain who had the previous episode of endometrial cyst resected.
WBC 12200/μL and CRP 16.55mg/dL were elevated.
CT and MRI showed contrasted wall thickening of the lobulated cystic lesion.
ADC map indicated restricted diffusion of abscess.
On CT and MRI,
fat layer density or signal intensity became inhomogeneous and irregular adjacent to the tubo-ovarian abscess.
TOA was confirmed pathologically.
Case 2. (Fig.7) TOA with IUD
40’s female with fever with intrauterine device (IUD) inserted eight years before.
WBC 15600/μL and CRP 22.49mg/dL were elevated.
CT showed the linear metal within the uterine cavity but it was not detected on MRI.
Multilocular cystic lesion of bilateral adnexa demonstrated wall thickening with prominent contrast enhancement.
ADC map indicated restricted diffusion.
TOA was suspected clinically.
At the upper abdominal portion,
CT showed peripheral enhancement of the liver on early phase that is known as perihepatitis,
Fits-Hugh-Curtis syndrome.
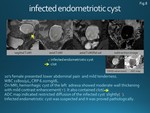
Case 3. (Fig.8) infected endometriotic cyst
20’s female with lower abdominal pain and mild tenderness.
WBC 11800/μL and CRP 6.02mg/dL were elevated.
On MRI,
hemorrhagic cyst of the left adnexa showed moderate wall thickening with mild contrast enhancement.
It also contained clot of low signal intensity on T2WI.
ADC map indicated restricted diffusion slightly.
MR imaging suggested infected endometriotic cyst that was confirmed pathologically.
Case 4. (Fig.9) infected endometriotic cyst
40’s female with lower abdominal pain who had the previous history of endometriotic cyst resecting.
WBC 11000/μL and CRP 15.31mg/dL were elevated.
On CT and MRI imaging,
hemorrhagic cyst showed prominent wall thickening with contrast enhancement of the left ovary.
ADC map indicated restricted diffusion.
endometriotic cyst was considered infected.
MR imaging suggested infected endometriotic cyst that was proved pathologically.
Case 5. (Fig.10) pyosalpinx
30’s female with lower abdominal pain and fever with steroid medication for SLE.
WBC 25100/μL and CRP 26.76mg/dL were elevated.
On both CT and MRI imaging,
cystic lesion of the left adnexa showed wall thickening with prominent contrast enhancement.
ADC map indicated restricted diffusion of abscess.
TOA was suspected,
however,
pyosalpinx was confirmed pathologically after the fallopian tube resection.
Case 6. (Fig.11) chronic pyosalpinx
20’s female with lower abdominal pain and brownish-red vaginal discharge.
WBC 6700/μL and CRP 2.52mg/dL were elevated.
On CT and MRI imaging,
cystic lesion of the bilateral adnexa showed wall thickening with prominent contrast enhancement.
ADC map indicated restricted diffusion of abscess.
TOA was suspected,
however,
pyosalpinx was confirmed pathologically after fallopian tube resection.
Chlamydial infection was proven by the vaginal secretion.
Case 7. (Fig.12) pyometra
80’s female with fever who was suspected ovarian abscess on TVUS.
WBC 33600/μL and CRP 17.95mg/dL were elevated.
CT showed huge cavitary formation with air-fluid level within the uterus.
After pyometra was pointed out on CT,
drainage was performed from the uterine cavity.
She became asymptomatic after about 400cc of pus was drained.
Case 8. (Fig.
13) infected uterine leiomyoma and abscess
50’s female with abdominal fullness and untreated diabetes mellitus.
WBC 9700/μL and CRP 32.06mg/dL,
Hb-A1C 13.2%.
MRI and CT showed huge cavitary formation and ill-defined tumor with replaced the uterus.
Hysterectomy was performed after abscess drainage.
This huge uterine tumor was confirmed huge subserosal leiomyoma sized at 25cm by gynecologists and was confirmed necrotic leiomyoma pathologically.
Case 9. (Fig.
14) uterine leiomyoma with degeneration
40’s female with abdominal pain who was suspected degenerating uterine leiomyoma on TVUS.
WBC 15900/μL and CRP 9.80mg/dL were elevated.
Degenerative or infectious uterine leiomyoma was suspected on the initial MRI.
After antibiotic therapy,
degenerating portion was decreased in size and hysterectomy was performed.
Pathologically leiomyoma was revealed degenerative with necrosis and hemorrhage.
This case wa considered resembling PID because of overlapping acute pelvic pain and MRI findings with diminished internal enhancement of uterine leiomyoma.
Case 10. (Fig.
15) ovarian borderline tumour with infection
20’s female with right lower quadrant abdominal pain.
WBC 7700/μL and CRP 9.18mg/dL were elevated,
but CA125 slightly increased at 76.1U/mL.
The clinical presentation was suggestive of PID with endometriotic cyst.
On T2WI,
tiny papillary projection was recognized with mild enhancement and moderate restricted diffusion of the right ovarian tumour.
This appearance was suggestive to remind ovarian neoplasm.
Histologically,
the papillary projection was composed of mucinous-type,
tubal-type and eosinophilic type epithelium with mild atypia.
Cystic component was lined with endometrial-type epithelium and stromal cells.
Therefore this ovarian mass was diagnosed as seromucinous borderline tumour associated with endometriotic cyst.