MRI-SCANNER
Both 1.5T and 3T MRI scanner are currently used to perform chest-MRI.
While scan protocol with 1.5T have been recommended3,
lung MRI is feasible also at 3T magnetic field,
despite signal decay can be faster due to magnetic susceptibility effects dependent on the field strength8.
MRI-SEQUENCES - STATE OF ART
New technological improvements have enhanced MRI resolution and SNR,
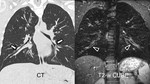
with image quality comparable to Computed Tomography(CT),
in particular for lung morphological changes in pathologies like Cystic Fibrosis(CF) or even superior to CT for the assessment of functional changes8,9.
MRI compared to CT represents a one-stop shop solution,
which allows both morphological and functional imaging in a single session.
Ultra-short-sequences
Most advanced techniques use Gradient Echo(GRE) sequences with TE in range of microsecond(ultrashort-TE,
UTE),
achieving sub-millimetric isotropic voxel size and resolution comparable with CT in visualizing lung structures,
included fissures and airways walls10.
3D-radial UTE sequences used in quiet breathing neonates permitted the visualization of regions of increased parenchymal signal,
like regional fibrosis or atelectasis,
or decreased signal,
like alveolar simplification11.
UTE showed sensitivity and specificity comparable to CT for several lung diseases,
such as CF also in early lung disease12.
For instance,
in CF patients a 3D-noiseless free-breathing sequence,
known as PETRA (pointwise encoding time reduction with radial acquisition imaging) detected lung structures alteration at segmental level such as bronchiectasis and parenchymal modification13 and showed bronchi up to the fourth/sixth generation,
with a good agreement with CT14.
In these hybrid sequences the outer k-space is filled with radial half-projections,
while the gap in the middle k-space is filled on a Cartesian trajectory comparable to single point sequences.
PETRA sequences have been shown to allow fast MRI imaging and to have shorter encoding times over the whole k-space compared to UTE15.
Zero-TE(ZTE) is another sequence with ultrashort T2/T2-star where the encoding can start simultaneously upon signal excitation,
giving a TE around zero and reducing the signal decay caused by lung parenchyma T2-star.
It has been demonstrated that ZTE is a promising sequence to study lung parenchyma since it showed a significantly higher parenchymal signal and intratracheal air than UTE,
with higher SNR16.
UTE has been recently used interstitial lung diseases(ILD),
where chest MRI showed good agreement with CT scan for emphysema,
bullae,
bronchiectasis and reticular opacities17.
In ILD patients,
chest MRI have shown interesting results to detect lung inflammation18.
Gradient-echo-sequences
Other non-UTE Gradient Echo sequences identified consistent structural changes in Broncho-Pulmonary-Dysplasia premature children respect full-term patients19.
3D-GRE T1-weighted volumetric-interpolated-breath-hold sequences like VIBE(Siemens) allowed the detection of lung nodules in PET-MRI20,
while the non-contrast CAIPIRINHA-VIBE(Controlled-Aliasing-In-Parallel-Imaging-Results-in-Higher-Acceleration) identified pulmonary lesions with diameter bigger than 5mm in 3T MRI with high accuracy in comparison with CT.
A chest-MRI protocol including VIBE sequences has been compared with low-dose CT showing a much lower false positive rate for cancer detection21.
Bronchiectasis and mucus plugs can be detected by balanced steady-state-free-precession(bSSFP) sequences by enhancing water-like signal of tissues.
Steady state sequences are GRE sequences where the longitudinal and transverse magnetization are kept constant22.
Failo et.al9 used an ultra-short TR/TE 2D-SSFP obtaining a very good correlation between HRCT and MRI in children with CF. In particular the correlation was good for the detection of bronchiectasis,
mucus plugging and atelectasis,
while it was moderate for trapped-air.
Spin-echo-sequences
Lung diseases with increased proton density,
namely consolidations and effusions,
can be assessed by T2-weighted sequences.
Airways diseases like CF,
Chronic Obstructive Pulmonary Disease (COPD) and asthma may present inflammatory wall changes with edema and intraluminal mucus which are highlighted by T2w images,
including post-contrast imaging where wall inflammation demonstrates contrast-enhancement23.
T2-w cardiac and respiratory triggered Fast-Spin-Echo sequences combined to fat saturation techniques have been used to detect lung inflammation in ILD24 using a 3T-MRI scan.
Signal intensity was measured placing small region-of-interest (ROI) and high-resolution CT(HRCT) was used as reference standard.
Active inflammatory lung tissue showed high T2w signal while chronic and fibrotic tissue had intermediate signal comparable to the muscle.
Moreover,
areas of active ILD with ground-glass-opacities in CT corresponded to lung areas with MRI-SI twice higher that of the intermediate signal areas.
PROPELLER(GE) or BLADE(Siemens) are TSE readouts which collect data using rotating k-space blades,
reducing respiratory artifact25.
Respiratory-triggered proton-density-weighted PROPELLER/BLADE sequences were compared in 1.5T scanner with 64-rows CT in stable CF patients and had lower sensitivity in the detection of severe bronchiectasis,
but showed good intra- inter-observer agreement with CT to assess CF-related lung abnormalities26.
Half Fourier acquisition single-shot turbo spin echo (HASTE-Siemens) are were used as non-contrast sequences for the evaluation of pulmonary consolidation,
necrosis and emphyema27.
In CF patients HASTE sequences with parallel imaging technique identified with good correlation with CT for bronchiectasis,
bronchial wall thickening,
mucus plugging,
sacculation/abscesses,
collapse/consolidation and segmental or lobar destruction28.
T2-star-sequences
T2-star imaging have been proposed to differentiate interstitial patterns and to quantify fibrosis in ILD.
Buzan et al.29demonstrated that there is an increment in SI of T2 mapping measurements with the severity of lung remodeling in ILD.
The results depend on the influence of free water and bound water molecules on T2 relaxation time: a lower number of free water molecules leads to lower T2 values like in normal lung tissue while higher number leads to higher T2 relaxation time like in fibrosis.
Authors also found significant difference in T2 relaxation time between ground-glass opacities,
reticulation and honey-combing.
Moreover T2-star maps have been proposed in a recent protocol for functional imaging in ILD using 3D-SPGR T2-star multi-echo sequences both in inspiration and expiration,
confirming that T2-star is longer in fibrotic tissue while R2-star(R2-star=1/T2-star) is therefore smaller compared to normal lung tissue18.
Contrast-enhanced-MRI
Gadolinium-enhanced-3D-MRI-angiography(CEMRA) can identify subsegmental pulmonary arteries of a normal lung30.
Dynamic contrast-enhanced MRI showed a reduced contrast-enhancement in COPD patients with sign of emphysema.
The contrast administration in chest-MRI can be combined with cardiac MRI for the assessment of right ventricular structure and function for example in the evaluation of pulmonary hypertension31.
For the evaluation of the late enhancement of fibrotic lung tissue 3D fat-saturated SPGR sequence has been proposed after 10 and 20 minutes after gadobenate-diglutamine injection in ILD study protocol18.
Dynamic-sequences for airways collapse
Central airways collapse can be assessed by static and dynamic MRI acquisitions using key-hole techniques during breath-hold or forced-expiratory maneuvers.
Compared to CT,
cine-MRI has been demonstrated to be feasible and better to quantify severity of tracheobronchomalacia,
since during the dynamic maneuver MRI enables to acquire the moment of maximum collapse of trachea while CT provide a single snapshot32.
Diffusion-weighted-imaging (DWI)
Diffusion-weighted-imaging(DWI) allows tissue characterization through the diffusivity of water molecules within tissues.
While there is still a limitation of DWI in the detection of lung nodules smaller than 1cm,
some authors showed that SI in DWI can accurately differentiate benign from malignant nodules33.
Apparent-diffusion-coefficient(ADC) values seem to be useful to differentiate central lung carcinoma masses from post-obstructive consolidations34 and to differentiate epithelioid mesothelioma from non-epithelioid (sarcomatoid and biphasic) type35.
DWI sequences have been suggested to quantify lung inflammation in CF disease and strongly correlated with the disease severity36.
A 2D-DWI multi-b-value acquisition has recently been proposed to assess lung inflammation in ILD18.
Fourier-Decomposition
Fourier-Decomposition is a non-contrast enhanced technique used to assess ventilation and perfusion defects.
It is based on 2D-SSFP sequences with high temporal resolution without cardiac or respiratory gating in coronal and sagittal view.
It has been used for the lung perfusion assessment also in CF children37 and to quantify regional ventilation in COPD patients.