Keywords:
Genital / Reproductive system male, Oncology, Artificial Intelligence, MR, CAD, Diagnostic procedure, Staging, Cancer, Pathology
Authors:
M. Xu1, L. Gong2, D. Dong2, J. Tian2, X. Fang1; 1Wuxi/CN, 2Beijing/CN
DOI:
10.26044/ecr2019/C-3172
Methods and materials
Prostate cancer patients with identified postoperative pathological results and was collected continuously from 2008 to 2016 in Wuxi People’s Hospital.
All patients were scanned at a single institution with 3.0-T MR scanners (MAGNETOM Verio,
Siemens Healthcare,
Erlangen,
Germany) using pelvic phased-array coils.
In total,
207 patients with GS=7 were identified and involved in this study,
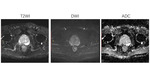
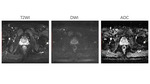
which GS (4+3)(Fig.1) vs.
GS (3+4)(Fig.2) close to 1:1.
For every standard prostatic MRI examination conducted in our hospital,
the protocol included a combination of T1-weighted imaging (T1WI),
T2WI,
DWI and its derivative ADC imaging.
We used three types of MR images in our study: T2WI,
DWI,
and ADC.
[5] Every slice of the prostate gland was confirmed and segmented on both the T2WI,
DWI and ADC MR images.
The standard of histological-radiological correlations was established through a systematic consensus-seeking correlative review of histological and MR findings by an experienced genitourinary pathologist.
Intra-class correlation coefficients (ICCs) were used to evaluate the intra- and inter-observer agreement of the feature extraction.
Two radiologists with experience over 10 years in prostate MR imaging participated in the evaluation of tumor masking.
There were Intra- and Inter- observer randomly selected 61 patients to reproduce of tumor masking,
and initial radiomic features were extracted to analyze.
An ICC greater than 0.8 was considered presenting good agreement.
The predictive performance was calculated using receiver operating characteristic (ROC) curve and P <0.05 were considered statistically significant.