Type:
Educational Exhibit
Keywords:
Neuroradiology spine, Bones, CT, MR, Conventional radiography, Diagnostic procedure, Congenital
Authors:
M. Boumediene1, A. DAGHFOUS2, E. JEMEL3, M. Boukoucha3; 1Tunis/TN, 2BEN AROUS/TN, 3Tunis /TN
DOI:
10.26044/ecr2019/C-3192
Findings and procedure details
The scanner allows precise and meticulous study of the bone structures and a great ease of interpretation thanks to the multiplanar cuts.
Indeed,
the scanner offers the possibility of multiple oblique views,
in any plane,
which facilitates the understanding of complex structures.
The advantage of CT is also in its sensitivity and specificity in the detection of minor bone malformations which remains superior to MRI,
100% in most series [3].
The CT also allows a satisfactory analysis of the bone relations with medullar strucures in the case of malformative association of bone and nerve.
Hence the interest of pointing out that in case of particularly complex malformations,
it is necessary to know the precise question posed by the surgeons before embarking on a scanning scan and this to spare the patient an unnecessary irradiation [4].
The diagnosis of basilar impression is relatively difficult on axial cuts especially when it is minimal.
Axial sections show a tip of the odontoid at the anterior part of the foramen magnum.
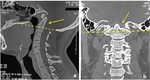
The diagnosis is much more obvious on sagittal reconstructions especially after tracing the lines of Chamberlain and Mac Gregor (Figure 1).
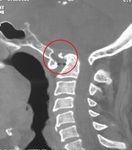
The oblique coronal and sagittal reconstructions find all their interest in the diagnosis of the occipitalization of the atlas,
in particular the partial forms where the fusion can represent only a small lateral attachment,
difficult to visualize on the MRI (Figure 2).
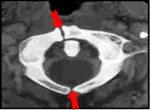
Due to the absence of an MRI signal in the cortex of the C1 anterior arch and the odontoid,
the CT scan better demonstrates the dislocation of C1-C2 and facilitates a more subtle interpretation than MRI (Figure 3).
Concerning the atlas anomalies,
the CT allows to visualize the dehiscence of the vertebra,
moreover it offers an excellent contrast between the ossified and non ossified parts of the C1 arc which allows a precise appreciation of the extent of the anomaly (Figure 4).
The scanner sometimes shows at the basal part of the clivus,
a medial notch separating two bony protuberances,
or ridges in ratio proatlas.
This notch should not be confused with a dehiscence of the anterior arch of the atlas.
The main advantage of MRI is the study of the bulbo-medullary junction and the visualization of the stress exerted on the spine by the bone malformation as well as by a possible Chiari malformation associated.
In MRI,
the diagnosis is rather easy and the different hinge marks in the coronal,
axial and sagittal planes described in conventional radiography apply perfectly as they were established more than 50 years ago.
However,
there are specific difficulties with MRI.
Indeed,
in some cases it may be difficult to define the edge of the bony palate on T2 sagittal sequences,
and one should look for cortical hyposignal of bone on T1-weighted sequences [5].
To define basilar invagination it is recommended to measure the shortest distance perpendicular to the upper end of the odontoid [6] (Figure 5).
The incidence of atlanto-occipital fusion would be 0.2 to 2% [7] (Figure 6).
MRI shows a continuous bone marrow between the unsegmented basiocciput and the C1 anterior arch with a characteristic "comma" configuration,
it also shows the absence of occipitoatloid ligaments or membranes and a modified path of the vertebral artery.
.
The first cervical vertebral fused to the occipital bone almost always appears hypoplastic,
which shortens the hinge and places the odontoid at the anterior part of the occipital foramen.
The fusion may only be outlined and appear as an atloido-occipital pinch.
Most often there is a synostosis of the condylo-atloid joints.
The major malformations of the axis affect the odontoid and are represented by the agenesis of the odontoid (dens aplasia) and the mobile odontoid (os odontoïdeum) [8].
They are associated with instability of the COJ.
The mobile odontoid (os odontoïdeum) is translated on MRI by a separation between the odontoid and the body of C2.
The odontoid separated appears rounded,
with regular contours,
limited by a thin cortex and clearly separated from the body of the axis whose upper surface is regularly corticalized.
These characteristics allow the differential diagnosis with a fracture of type 2,
recent or old,
of the odontoid.
The COJ is unstable and during flexion the spinal canal narrows between the postero-superior corner of the body of the axis and the posterior arch of the atlas [9].
The anterior dislocation of C1 on C2,
determines a maximal odonto-atloid diastasis in bending of the head,
at the origin of an acute medullary compression from which the gravity of this malformation (Figure 7).
In MRI,
atlantoaxial dislocation appears indifferent and may be more obvious in flexion when dynamic maneuvers are possible.
The atlantoaxial interval is at most 2 mm in the adult and 4 mm before the age of 15 years.
Although the CT diagnosis is obvious MRI is more difficult to interpret because of the absence of signal at the cortical level of the anterior arch of the atlas and the odontoid,
it can show,
moreover,
a hypotrophic transverse ligament [10].
Congenital stenosis of the occipital foramen is observed,
most often in the context of achondroplasia [11],
it is an exceptional malformation.
The MRI shows a simultaneous reduction in the sagittal and transverse diameters of the foramen magnum.
It is responsible for posterior compression of the bulb and cervical cord.
Coronal sections in MRI appreciate the asymmetries of the occipital condyles,
the lateral masses of the atlas and/or the axis.
Asymmetry of the hinge in the frontal plane and induced static disturbances are evaluated thanks to the intervestibular line of Wackenheim.
Asymmetry often affects the three bones at the same time,
sometimes asymmetry of the odontoid is associated [11].
The hypertrophy and the too internal position of the occipital condyles can induce a myelopathy by transverse stenosis of the spinal canal.
The analysis of bone asymmetries,
although obvious in CT,
is more delicate in MRI because of the variable signal and the difficulty of defining the cortical bone in some cases [11].
Axial MRI sequences,
easily identify partial agenesis of the atlas and demonstrate the associated malformations.
These malformations can probably weaken the atlas,
but should not be confused with fractures [12].