Patient population: during the period between June 2012 and June 2015,
among 3518 percutaneous breast biopsies performed under ultrasound,
stereotactic or MRI guidance in our Institute,
85 were classified as B1 (0.02%).
The mean age of these women was 55.2 years (range 27-80 years).
Imaging guidance: among 85 B1-lesions,
4 biopsies (4.7%) were performed under stereotactic guidance,
while 81 biopsies (95.3%) were performed under ultrasound guidance.
None of the biopsies performed under MR guidance was classified as B1.
Histopathological findings: among 85 B1-lesions,
70 (82.4%) were described as "normal mammary parenchyma",
while 15 (17.6%) were found to be "inadequate for diagnosis / insufficient material".
Among these last 15 lesions,
in 8 cases the pathologist described the presence of atypical cells.
Of the 85 B1-lesions,
18 (21.2%) were found to be breast cancers: 12/18 (66.8%) at surgical excision,
4/18 (22.2%) with re-biopsy,
1/18 cases (5.5%) with re-biopsy at 6 months follow-up (Fig. 1),
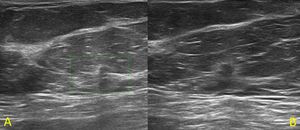
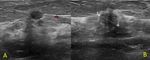
Fig. 1: Fifty-nine year-old patient with recent retraction of the right nipple. Mammographic examination was normal. With ultrasound, on the upper-outer quadrant of the right breast a hypoechoic 5 mm lesion with indistinct margins (U4b) was found. Histological diagnosis was “normal mammary parenchyma” (A). At 6 months follow-up (B) the lesion was re-biopsied because of a small increase in size and because of the presence of perilesional hyperechoic halo. The final histological diagnosis was "infiltrating ductal carcinoma".
and in 1/18 (5.5%) with re-biopsy at 24 months follow-up (Fig. 2).
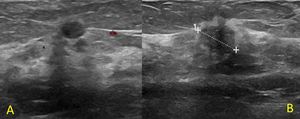
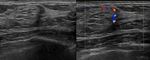
Fig. 2: Sixty-four year-old patient recalled from screening for a small mass in the left breast. At ultrasound a small, hypoechoic area in the upper peri-areolar region of the left breast (U3) was found. The histological diagnosis was "normal mammary parenchyma" (A). At 6-months follow-up no changes were noted. At 24-months follow-up (B) the lesion appeared hypoechoic, with irregular shape and indistinct margins (U5); at re-biopsy it resulted an "infiltrating ductal carcinoma".
Statistical analysis: the degree of suspicion according to BIRADS (≤R4a,
≥R4b) and the presence or absence of cellular atypias resulted significantly different between Breast Cancer and Non Breast Cancer groups (both p<0.0001).
Breast Cancer group included 77.8% (14/18) ≥R4b lesions and 38.9% (7/18) lesions with atypical cells,
while Non Breast Cancer group included 4.5% (3/67) ≥R4b lesions and 1.5% (1/67) lesions with atypical cells.
The other features were not significantly different between the 2 groups (Table 1).
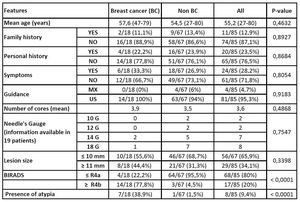
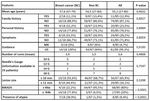
Table 1: Features assessed in Breast Cancer and in Non Breast Cancer group, with p-values.
Malignancy was associated with BI-RADS ≥R4b and/or presence of atypical cells in 83.3% (15/18) of cases (p<0.0001); the remaining 3/18 malignancies were ≤10mm.