Among the diseases that originate in the pancreas,
two entities stand out because they are not easy to differentiate using imaging techniques: pancreatitis of the groove and pancreatic neoplasms,
among which are the ductal adenocarcinoma because of its greater frequency and in more isolated cases the neuroendocrine tumor (gastrinoma).
Groove pancreatitis is a rare type of chronic pancreatitis that can occur in its segmental form in which there is involvement of the groove and the head of the pancreas or in its pure form in which only the groove is affected preserving the pancreatic gland.
It usually affects men in the 4th or 5th decade of life with a history of severe chronic alcoholism associated with smoking.
The clinic is varied but usually produces postprandial pain,
vomiting,
weight loss and less commonly an oscillating jaundice.
Certain complications have been described,
such as perforation or gastrointestinal bleeding and,
exceptionally,
the malignant degeneration of the heterotopic pancreas.
The pathogenesis is unknown,
but the alteration in pancreatic secretion through the Santorini canal related to the damage caused by excess of alcohol is proposed as the most accepted mechanism.
Peptic ulcers,
gastric resections,
cysts in the duodenal wall or in the pancreatic head and pancreatic heterotopias have also been postulated as possible triggers.
The diagnostic tests that are used are the endoscopy that provides accurate information of the location and extension and usually objectifies thickening and stenosis of the duodenum as well as the common bile duct,
endoscopic retrograde cholangiopancreatography (ERCP) that although difficult to perform in advanced phases can demonstrate the smooth stenosis of the common bile duct,
without alterations in the main pancreatic duct,
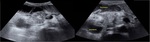
ultrasound that evidences a hypoechoic mass in the groove región with thickening of the duodenal wall that causes a narrowing of the second portion and a common bile duct obstruction (Fig.
1),
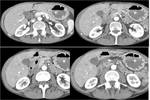
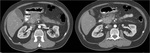
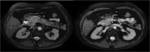
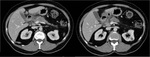
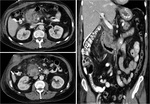
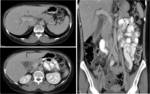
CT where a hypodense lesion is observed in the groove and small cystic lesions in the duodenal wall (Fig.
2,
3,
4,
6) and MRI,
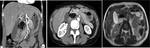
where we can identify a laminar mass in the groove that is hypointense in T1 and iso or hyperintense in T2 sequences (Fig.
5).
In these last two tests a heterogeneous enhancement of the lesion is observed after contrast administration and a normal appearance of the adjacent vessels,
although they may be displaced in some cases.
The importance of groove pancreatitis is that it can simulate a pancreatic carcinoma,
it can coexist with it or even to mask it.
So in both cases the differential diagnosis is difficult to find either by ultrasound,
CT or MRI.
In the milder cases,
the treatment is conservative with analgesics and alcohol withdrawal,
although in many cases surgical treatment is chosen if the symptoms do not improve,
if there are complications or if there are diagnostic doubts.
In these cases,
the technique of choice is cephalic duodenopancreatectomy since it allows an accurate diagnosis and an effective treatment.
Adenocarcinoma is the most frequent malignant tumor of the pancreas and has a poor prognosis because most cases are diagnosed in advanced stages due to the non-specificity of the initial symptoms.
These tumors frequently settle in the pancreatic head causing abdominal pain,
weight loss and obstructive jaundice.
It usually affects men from 6th to 8th decade of life with active exposure to tobacco.
The elevation of the tumor markers CEA and CA 19.9 can be of help especially for the monitoring of therapeutic response and follow-up.
For its diagnosis,
the technique of choice is CT,
where a hypodense and poorly defined mass is usually observed (Fig.
7).
After contrast administration the mass enhances homogeneously but less than the rest of the parenchyma.
It can produce an abrupt ductal obstruction,
a mass effect of the contour of the gland,
an atrophy of the remaining pancreatic parenchyma,
a dilation of the biliary and pancreatic ducts and in more advanced cases a vascular and neighboring organs infiltration.
It has been shown that pancreatic carcinomas that reach the pancreatic area can not be differentiated from groove pancreatitis by imaging techniques in cases where there are no cystic lesions within the mass and / or thickenings of the duodenal wall.
Regarding the pathology of duodenal origin we must establish the differential diagnosis between the duodenal diverticulum,
without forgetting the possibility of tumors of origin in the periampullary region.
The duodenal diverticulum normally affects the 2nd and 3rd portion of the duodenum and can be complicated by diverticulitis.
For its diagnosis,
it is useful the visualization of the oral contrast or gas within itself and its communication with the duodenum (Fig.
8).
Duodenal exophytic adenocarcinoma is an infrequent neoplasm that is most commonly located in its second portion.
It is presented as a mass that can produce invasion of the bile duct and obstruction of the intestinal loops (Fig.
9).
Similarly,
the duodenopancreatic groove contains lymph nodes so we will have to take into account in the diagnosis pathologies that affect them,
mainly metastasis,
lymphoma or infections.
If there is a striking increase in lymph node size,
it may be difficult to distinguish it from a pancreatic tumor,
but in the first case the pancreatic or bile ducts are not usually obstructed.
The pathology that can affect the duodenopancreatic groove can also have its origin in the distal third of the common bile duct,
among which cholangiocarcinoma or common bile duct cysts stand out due to their frequency.
Distal cholangiocarcinoma can be presented as a mass that infiltrates the groove and produces a dilatation with abrupt sharpening of the bile duct caused by the thickening of the ductal wall or by a polypoid mass.
In the image tests,
its ring enhancement is characteristic.
The choledochal cyst can simulate a liquid collection in the groove.
This lesion is observed as an abrupt change of caliber in the junction between the dilated segment and the normal conduit.
For its confirmation it is necessary to observe communication of the distal common bile duct with the hepatic ducts.