Clinical presentation
The clinical presentation of ureteral injury is varied.
Patients may present with fever,
hematuria,
dysuria,
anuria,
flank pain,
flank ecchymosis,
lower back pain,
peritonitis with or without leukocytosis,
incontinence,
vaginal urinary leak,
or they may even asymptomatic.
[6] Lack of hematuria does not exclude ureteric injury.
If there is any sign of hematuria,
further imaging or exploration should be performed.
[2]
Laboratories may show increased serum creatinine and blood urea nitrogen levels,
although these signs and symptoms are neither sensitive nor specific.
A high index of suspicion is vital when evaluating for ureteric injuries and low threshold for further imaging or exploration,
to avoid delayed diagnosis and treatment.
Indications for imaging
CT Urography has replaced retrograde pyeloureterography,
retrograde pyeloureterography and sonogram as the primary modality to evaluate the ureters.
[13] It usually includes three phases: non-enhanced,
contrast enhanced (corticomedullary vs nephrographic) and excretory phases.
In the setting of trauma,
the contrast enhanced phases are usually sufficient,
with the excretory phase being the most important.
Split-bolus technique combines the contrast enhanced and excretory phases into a single scan,
therefore reducing image acquisition to two scans in an effort to reduce radiation dose.
This is done by splitting the contrast bolus and injecting the second bolus 5-15 mins after the first bolus.
Image acquisition occurs 100 secs after the second bolus administration in order to obtain a nephrographic phase image.
In order to achieve adequate opacification of the ureters in the excretory phase,
oral hydration with 1L of water 1 hour before study,
if clinical scenario permits.
[9] Ureteral injury diagnosis is sometimes delayed due to underexcretion by an injured kidney and lack of a urinoma.
[13] In these cases,
additional delayed scans could be considered.
Retrograde pyelography is done via cystoscopy and believed to be the most accurate method for diagnosing ureteral injury.
Unfortunately,
this can only be done in stable patients.
[2]
Intraoperative one-shot intravenous urography is sometimes employed in unstable patients; however,
it is non-diagnostic for ureteral injuries in 33% to 100% of cases.
[4]
Ureteral injury - Review cases
Mechanisms of injury
Ureteral injuries represent 2.5% of all genitourinary trauma based on a retrospective analysis on the National Trauma Data Bank on 2002-2006.
The ratio of blunt vs penetrating injuries is 38.5% vs 61.5%.
[11] Associated injuries are present in 90.4% of ureteral trauma cases,
with the small and large bowel being the most common associated injured organ.
[7]
Penetrating trauma
Among penetrating trauma cases,
gunshot wounds are the most common cause,
representing 88% of penetrating trauma.
However,
the ureters are affected in only 2% to 5% of abdominal gunshot wound cases.
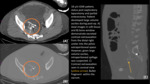
[11] Ureteral damage can result from partial/complete transection by the missile trajectory or devascularization from blast injury resulting in ureteral necrosis. Fig. 1

Fig. 1
Blunt trauma
Ureteral injury in the setting of blunt trauma is most commonly caused by acceleration and deceleration forces usually resulting in ureteral avulsion.
Among blunt trauma etiologies,
motor vehicle collisions are the most common (49%).
Blunt trauma cases have a higher association with pelvic fractures (20% vs 1%) when compared to penetrating trauma.
[11] Most common anatomical site of injury is the ureteropelvic junction.
[13] Mechanisms include avulsion,
disruption by bony fractures or compression against bone structures.
[11] Fig. 2

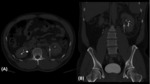
Fig. 2: Abdominopelvic CT with IV contrast in a patient with blunt abdominal trauma resulting in left kidney interpolar laceration with associated subcapsular hematoma. Axial (A) and coronal (B) delayed phase bone window images show minimal urinary contrast extravasation at the ureteropelvic junction worrisome for left proximal ureteral injury.
Iatrogenic injuries
The ureters are small structures with a long course along important abdominal and pelvic structures,
rendering them extremely vulnerable to iatrogenic injury.
Iatrogenic injuries account for approximately 75% of all ureteric injuries,
making them the most common mechanism of injury.
[1] They most commonly affect in the distal one-third of the ureter and the pelvic ureter.
[2] They may result from gynecological,
urological,
urogynecological,
obstetric,
colorectal,
general,
or vascular surgery procedures.
[2,10] Although preoperative ureteric stenting decreases the risk of ureteral injuries,
it does not eliminate it.
[2] Ureteral iatrogenic injuries include: ligation,
lacerations,
transections,
devascularization,
and crush injuries. Fig. 3

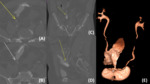
Fig. 3: Abdominopelvic CT with IV contrast in a patient with multiple intra-abdominal surgeries, including prior sigmoidectomy who presented to the ED with colocutaneous fistula status post intervention with a suspected ureteral injury. Axial delayed view (A) shows the normal contrast opacified mid right ureter. Delayed phase axial (B), coronal (C) and sagittal (D) reconstructions show a right distal ureteral transection, at the level of the pelvic inlet, with interfascial ureteral contrast extravasation along the extraperitoneal spaces(arrows). Volume-rendered 3D reconstruction (E) shows the right distal ureteral transection with associated urinoma (yellow arrow). The left ureter shows adequate contrast opacification up to its normal ureterovesical junction.
Imaging characteristics
Avulsion
As previously stated,
the most common site of avulsion injury is the ureteropelvic junction (UPJ).
The main theory that explains this finding is that the ureter is fixed in the retroperitoneum while the kidney is relatively mobile.
When submitted to hyperextension due to acceleration and deceleration forces it results in shearing and avulsion at the UPJ.
[11] Ureteral avulsion is three times more common in children than in adults,
likely due to their increased laxity and higher potential degree of hyperextensibility.
[1] A medial or perirenal contrast extravasation without renal injury is worrisome for UPJ injury.
If distal ureteral contrast is present,
then findings would favor a UPJ laceration,
otherwise an avulsion is suspected which would require immediate surgical management.
[10] Additional findings of missed ureteric injury would include localized collections (urinoma),
ascites or hydronephrosis.
[2]
Laceration vs transection
Ureteral laceration/transection is most commonly associated with the direct missile impact of gunshot wounds.
The upper,
mid and distal ureteral segments are affected at approximately the same ratio (43,
38 and 37 cases in a 118 study by Perez-Brayfield).
A ureteral transection is suspected if there is contrast extravasation and no distal intraureteral contrast present.
If distal ureteral contrast is noted,
then extravasated contrast would most likely be due to a laceration.
Surgical repair is based on location (upper,
mid or distal ureter) and extent of injury.
Avulsion repair can include primary anastomosis,
ureterocalicostomy,
ureteroureterostomy or ureteral reimplantation into the bladder without or with renal mobilization,
while lacerations involving less than 50% of the ureteral diameter can be managed with ureteral stenting.
Gunshot wounds usually require debridement while stab wounds do not.
[4] Fig. 4, Fig. 5, Fig. 6, Fig. 7, Fig. 8

Fig. 4

Fig. 5

Fig. 6

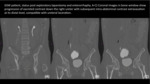
Fig. 7: Abdominopelvic CT of a patient with multiple gunshot wounds, arterial phase axial (A) and sagittal (B) soft-tissue views showing abundant hemoperitoneum and free fluid. Axial (B) and sagittal (D) delayed images demonstrate urinary contrast extravasation associated to the left ureterovesical junction (yellow arrows in B and D) consistent with transection of the distal ureter at the left ureterovesical junction.

Fig. 8: Abdominopelvic CT of a patient with multiple gunshot wounds; arterial phase coronal (A) soft-tissue window showing abundant hemoperitoneum and free fluid. Coronal (B) delayed image demonstrates urinary contrast extravasation associated with discontinuation of the left distal ureter at the ureterovesical junction (yellow arrow in B). Posterior volume-rendered 3D reconstruction of the same patient shows the left distal ureteral transection with associated urinoma (yellow arrow in C).
Contusions
Ureteral contusions are visually diagnosed during exploration,
and if unrecognized can lead to delayed leaks and strictures.
If the ureteral contusion is severe,
resection and surgical reconstruction is recommended.
[2]
Devascularization
Blast injury by the missile can cause ureteric intramural microvascular damage by thrombosis and ischemia,
resulting in ureteral necrosis.
These types of injuries are at risk for delayed complications (days to weeks),
which include urine leakage,
fistula and strictures.
[2,7] Although there are no direct imaging finding of ureteral necrosis,
the complications can be easily recognized on CT urography as contrast diversion (leakage,
fistula) or ureteric dilations (strictures).
Common misses / Imaging pitfalls
When dealing with ureteral injuries,
prompt diagnosis is of utmost importance since delayed in diagnosis leads to a marked increased risk of complications (fistula,
urinoma,
infection,
renal unit loss,
death). [2,6] Due to the widespread availability and relative low cost of CT scanners,
CT is the front-runner in evaluation of the polytraumatized patient,
ureteric injuries are most commonly diagnosed by CT.
As described earlier,
these injuries may present with contrast extravasation on the delayed phase of a contrast-enhanced CT,
hydronephrosis,
ureteric obstruction,
urinary ascites,
and localized fluid collections,
among others.
[6] However,
as one may note,
these are nonspecific signs and patients with ureteric injuries may present with none of these.
It is vital for radiologists and interpreting physicians to be cautious when evaluating post-traumatic abdominopelvic CT scans or CT urograms to rule out ureteral injuries; a high index of suspicion is needed to adequately assess the urinary tract for leaks or collections and reliably diagnose ureteric injuries.
[2]
Common mimickers include,
but are not limited to: ordinary ascites,
abscesses,
hematomas,
or cystic masses,
all of which may be mistaken for urine leaks and urinomas.
Residents and radiologists should always review excretory phase images in patients with trauma and post-surgical patients and must always window to assess for possible contrast extravasation of excreted contrast material,
which may be missed on soft-tissue windows. Fig. 9, Fig. 10, Fig. 11

Fig. 9: Axial excretory phase images of a patient with multiple gunshot wounds who presented with abdominal distention and abundant discharge by surgical wound. (A) shows abundant intraperitoneal low-attenuation free fluid with mild thickening enhancement of the peritoneal lining, concerning for developing peritonitis. (B) shows a rim enhancing fluid collection in the left psoas muscle/posterior pararenal space and paravertebral muscles, in favor of abscess formation. The intra-abdominal fluid collections were drained. Arrow in (C) confirms this collection to be an urinoma with pooling of excreted contrast and transected left ureter.

Fig. 10: Patient with multiple gunshot wounds to the abdomen. Axial views of IV contrast enhanced abdominopelvic CT on excretory phase show the normal right ureter (A) , site of distal right ureteral laceration (B), and excreted contrast pooling into urinoma (C). Sagittal views soft-tissue window (D) and bone window (E) show the site of right ureteral laceration. On the initial radiology report this was read as large volume ascites.

Fig. 11: Same patient as in previous figure, delayed phase axial views bone window (A) and soft-tissue window of abdominopelvic CT performed 6 days later after patient developed leukocytosis. Axial images show active contrast extravasation of excreted contrast from the distal aspect of the right ureter into the pelvis. Fluoroscopy images (C) and (D) during percutaneous nephrostomy placement by Interventional Radiology service after ureteral ligation in the OR.
Complications
Complications after ureteral injuries are best avoided with prompt diagnosis and managements.
Delayed in diagnosis leads to higher rates of severe complications which result in increased morbidity and mortality.
[7] Although ureteral injuries rarely occur alone and commonly the same patient has multiple additional injuries,
associated bowel injuries or fecal contamination do not increase the risk of complications.
[2] The most common complications are: infection/periureteral abscesses,
fistulas,
ureteral strictures,
and urine leaks/urinomas.
[3,7]
Ureteral strictures,
delayed necrosis and urinary fistula usually occur if ureteral contusions are left untreated.
Severe blast injuries or contusions may result in damage to the ureteral blood vessels leading to thrombosis and ischemia,
eventually resulting in possible delayed necrosis,
urine leakage and/or ureteral fistulas.
[7] High-velocity gunshot wounds result in higher risk of delayed urinary leaks,
wound dehiscence after repair,
renal loss,
and overall mortality.
[2] Complications resulting from repair and missed injuries include: retroperitoneal abscesses,
infected urinomas and fistulas. Fig. 12, Fig. 13

Fig. 12: Excretory phase images of a patient who suffered multiple gunshot wounds, axial bone window (A-B), axial soft-tissue window (C-D) and coronal soft-tissue window reconstructions (E-F) showing a large intra-abdominal right hemiabdomen/midline abdomen peripherally enhancing fluid collection, with mass effect upon the adjacent abdominal structures. There is active contrast extravasation of the right ureter arrows in (A), (B) and (C), compatible ureteral laceration with active urine leak and urinoma with superimposed infection.

Fig. 13: Abdominal radiograph AP upright of the same patient as the previous figure showing interval placement of a right double-J catheter, with distal tip seen within the urinary bladder.
Management
Ureteral injuries are best managed early,
and the treatment depends on the location and/or mechanism of injury.
Post-traumatic patients who are hemodynamically unstable are usually and best managed by a planned staged repair,
which typically includes ureteric exteriorization or ligation.
[2] Final reconstruction is reserved for when the patients are stable.
Penetrating injuries
Ureteric contusions or injuries resulting from proximity of gunshot wounds are regularly treated with ureteric stenting.
However,
large contusions often need segmental excision and uretero-ureterostomy (UU).
If untreated,
ureteric contusions may result in ureteric strictures,
delayed necrosis and urinary fistula may result.
[2] High velocity gunshot wounds are best managed with primary repair.
If injuries are diagnosed in a delayed manner or urinary leak occurs after repair,
the customary management is percutaneous nephrostomies and depending on the case,
antegrade ureteric stenting.
[2] In the case of urinomas,
percutaneous drainage is the typical solution. Fig. 14

Fig. 14
Blunt injuries
The most common locations for ureteral injuries resulting from blunt trauma are at the ureteropelvic junction and proximal ureters.
When partial ureteric lacerations result from blunt trauma,
these are effectively managed by primary repair or ureteric stenting.
If complete transection/avulsion injuries occur,
the regular management is UU or ureteropyelostomy.
Iatrogenic injuries
Iatrogenic injuries are the most common type of ureteral injuries.
Surgical management depends solely on location,
time of diagnosis and type of injury.
When dealing with ligation injuries the management is ureteral de-ligation,
ureteric stenting and/or UU; nephrostomies are a means for urinary diversion.
[2] Crush injuries are also best treated with stents and/or UU.
[2] Since devascularization injuries are habitually diagnosed late,
they are managed with stents or surgical repair.
[2] Missed injuries are best treated with nephrostomies and for injuries with delayed diagnosis the regular management is retrograde stenting.
[2]