CLASSIFICATION SYSTEMS
Classification of CHC has evolved over time with Allen & Lisa originally describing 3 distinct subtypes in 1949.
This was subsequently updated by Goodman et al in 1989. The most recent and widely accepted WHO classification recognizes the important role of hepatic progenitor cells in the development of CHC and updated the classification into classical type and subtypes with stem cell features.
-
Allen & Lisa (1949)
-
Type A : Synchronous separate nodules of HCC and ICC
-
Type B: Contiguous masses that may mingle
-
Type C: Truly intermingled masses of both HCC & ICC/glandular components.
-
Goodman et al (1985)
-
Type I: Collision tumors or HCC and ICC in separate nodules in the same liver
-
Type II: Transitional tumors with intermingling of HCC and ICC
-
Type III: fibrolamellar variant of HCC
-
WHO (2010)
-
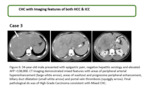
CHC classical type: areas of typical appearing HCC intermixed with CC and identifiable transition zones,
where the two components merge and show tumor cells with intermediate morphology.
-
CHC with stem cell features
Typical
Intermediate cell
Cholangiocarcinoma subtype
CLINICAL AND IMAGING APPEARANCES
Demographic and clinical features of patients with CHC differ from patients with conventional HCC,
however similarly to conventional HCC there are variations in risk factors between Asian and Western Populations.
Asian series report an increased association with chronic liver disease including hepatitis and an older male population.
Western series demonstrate a more balanced gender distribution and a weaker association with chronic liver disease.
Tumor markers can be helpful in raising the possibility of a CHC tumor,
as both CA19.9 and AFP can be elevated in contrast to conventional HCC,
typically associated with elevated AFP and ICC which demonstrates elevated CA 19.9.
While imaging features of HCC and ICH are well documented,
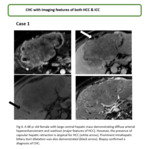
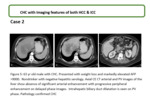
appearance of CHC is variable and heavily influenced by the relative composition and ratio of the underlying histologic subtypes frequently demonstrating mixed features of both HCC and ICC.
The sonographic appearances of CHC are nonspecific and US is most useful as a tool to enable image guided biopsy.
Contrast enhanced computed tomography (CT) and dynamic contrast enhanced magnetic resonance imaging (MRI) are the diagnostic imaging modalities of choice.
Imaging Features of HCC Imaging Features of ICC
Arterialenhancement Progressive/delayed enhancement
Washout on PV/equilibrium phase Capsular retraction
Pseudocapsule Biliary duct dilatation
Intratumoral Fat Necrosis
Tumor Thrombus Lymph node metastases
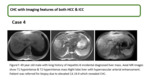
CHC tumors show significant overlap between classic imaging features of HCC & ICC however several studies demonstrate imaging appearances more closely resembling ICC.
Several studies also describe increased multifocality,
more frequent vascular and lymph node invasion.
Reflecting the pathological heterogeneity of these tumors,
accurate radiologic diagnosis of CHC imaging is challenging with differentiating between CHC and ICC proving the most difficult.
However,
given that the importance of differentiating CHC from HCC with respect to patient management and treatment options emphasis should be placed on identification of imaging features which raise the possibility of mixed pathologic subtype thereby ensuring accurate preoperative diagnosis.
In particular,
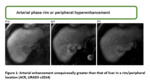
a peripheral enhancement pattern,
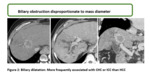
biliary duct dilatation or capsular retraction should raise the possibility of CHC or indeed IHC and commit the patient to further investigation.
Features raising possibility of CHC:
Peripheral enhancement pattern
Biliary duct dilatation
Capsular retraction
TREATMENT:
TREATMENT:
Surgical Management
No clear consensus guidelines exist for management of CHC,
however complete surgical resection remains the only curative option in eligible patients.
Due to the high frequency of lymph node metastases,
hepatic resection combined with hilar lymphadenectomy is recommended for CHC in non-cirrhotic patients.
Hepatic transplantation is generally not considered for CHC patients due to poor prognosis and high rates of tumor recurrence.
Systemic Therapy
Systemic chemotherapeutic regimen appears to only minimally impact survival and treatment regimens should be based on careful consideration of the clinicopathological features.
Regional Therapy
The increased fibrotic component and decreased vascularity of CHC limits the usefulness of treatments widely used in the setting of unresectable HCC,
such as Transarterial chemoembolization (TACE) and percutaneous treatments such as percutaneous ethanol injection (PEI) however they may have a role of carefully selected tumors with greater tumor vascularity.
Alternative regional treatments such as radiofrequency ablation,
cryoablation and radioembolization may have a role in treatment as part of a multimodality approach,
however due to small numbers and short duration of followup benefit remains unclear.