Classic AVM
The classic form of arteriovenous malformation involving the brain parenchyma,
it is characterized by a nidus in the transition between the feeding artery and draining vein. Its morbi-mortality is closely related to hemorrhages secondary to the rupture of an anomalous vessel or a high-flow aneurysm near or within the malformation(5,6).
Most AVMs are supratentorial,
with a description in the literature of close to 90%,
up to 9% multiple (6).
Location
Supratentorial: 85-90%.
- 1/3 deep AVM
- 2/3 Superficial AVM
Infratentorial: 10-15%.
Clinical Presentation:
Possible presentations include:
- Hemorrhage.
The risk of annual bleeding of an AVM is 1 to 3%,
it depends on the size and location (2).
- Seizures.
- Headaches.
- Ischemic events due to vascular steal.
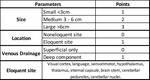
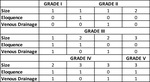
Classification:
The Spetzler-Martin AVM grading system reports morphology and location to the risk of surgery.
It's the most used.
Fig 1 and 2.
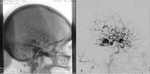
Angiographic Findings:
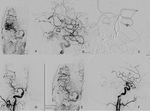
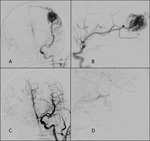
Depicts the 3 components of a classic AVM: Fig 3.
- Afferent enlarged arteries + flow-related aneurysms
- Nidus,
size and intranidal aneurysm.
- Venous drainage,
to superficial or deeps veins,
venous stenosis due to high flow venopathy.
Treatment:
The known risks for bleeding include previous hemorrhage,
association with aneurysms,
exclusive deep venous drainage and deep localization of the AVM.
For this reason,
treatment is focused on reducing bleeding,
for which there are four approaches: the conservative,
open surgery,
radiosurgery and embolization,
the last three with a clear objective of eliminating the anomalous vascular nest and maintaining normal venous drainage.
A premature venous closure can lead to fatal consequences due to increased dilatation of the vascular nest and hemorrhages.
The goals of embolization to further reduce the risk of bleeding from an AVM is to reduce its volume to less than 10cc for possible radiosurgery treatment.
The benefit of the use of embolization is given in the occlusion of the flow of deep nutritional arteries that are key in determining the morbidity and resectability of the malformation,
facilitates hemostasis,
reduces intraoperative bleeding and facilitates surgical dissection (7).
It can be used as a sole treatment or as a surgical precursor.
However,
there is a contradictory result in the ARUBA study (a randomized trial of unruptured brain arteriovenous malformations),
which compares conservative management with another type of treatment in non-injured AVM,
presenting a lower incidence of stroke or death in patients with conservative treatment (8-11).
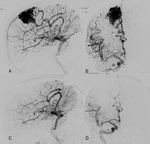
To perform this treatment is necessary a super-selective catheterization of the afferent nutritional artery,
then to embolize,
it normally is used ethylene vinyl alcohol copolymer or microparticles polyvinyl alcohol.
Fig 4.
Only afferent pedicles to the nidus are embolized in an attempt to avoid occlusion of branches irrigating normal brain(5).Fig 5-7
Cavernous malformation
It's a benign vascular hamartoma with intralesional hemorrhages.
Angiographic Findings:
- Commonly angiography is normal (occult vascular malformation).
- Slow intralesional flow without arteriovenous shunting.
- Avascular mass effect.
- In some cases,
venous pooling.
Usually treated conservatively. In some cases are surgical.
Dural AV Fistula
About AV shunts from dural vessels.
Classification:
Cognard classification and Borden classification are the two most commonly used (13).
Fig 8-9.
Angiographic Findings:
Allows systematic evaluation of feeding vessels.
Demonstrates the presence and extent of retrograde venous drainage.
Conservative treatment: observation and/or carotid compression technique.
If hemorrhage risk exists: Endovascular embolization,
surgical resection,
stereotaxic radiosurgery.
Pial AV Fistula
Pial vascular malformation with AV shunting,
without a nidus.
Angiographic Findings:
- Look for a fistula in a site of abrupt change in vessel caliber.
- The nutritional artery is often single and drains into an enlarged vein.
Usually treated with endovascular embolization.
Developmental Venous Anomaly
Angiographic findings:
- Arterial phase normal
- Capillary phase normal.
- Venous phase: "Medusa head" sign.
Usually not treated.