In our study,
we evaluated a great number of suprasellar injuries.
In most of them,
the anatomic approach was followed,
however many lesions affect more than one compartment,
making difficult to precise its origin.
For those cases,
the identification of normal structures,
such as the pituitary gland and its relationship with the injury helps to determine the etiology.
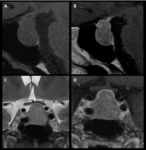
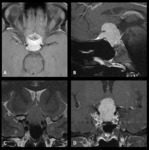
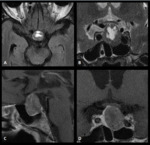
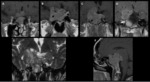
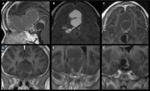
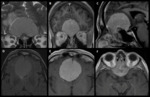
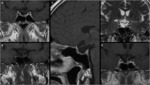
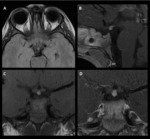
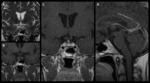
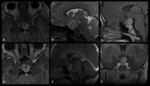
1 – Adenomas (Fig.
1-4):
Pituitary adenomas are adenohypophysal tumors composed of secretory cells that produce pituitary hormones.
Adenomas comprise the majority (80%) of the lesions.
A large percentage of these (approximately 75%) are functioning and result in endocrine abnormalities,
as hyperprolactinemia.
Patients can be asymptomatic or present symptoms due to compression of adjacent structures,
particularly the optic chiasm and optic nerves.
At imaging they present usually as T2/FLAIR hyperintense and hypo or hyperintense on T1WI.
Upon immediate imaging after contrast enhancement,
they are typically hypointense on T1WI relative to the remaining normal pituitary tissue.
As there is up to a 20% false-negative rate in the detection of microadenomas,
dynamic contrast-enhanced MRI can be performed to increase the sensitivity and specificity.
Microadenomas are defined as lesions ≤10 mm and macroadenomas are >10 mm in diameter.
Approximately,
10% of adenomas can be complicated by hemorrhage,
infarction or necrosis/cystic change,
which alters the MRI signal intensities.
Adenomas can expand cephalad into the suprasellar cistern and compress the optic chiasm and optic nerves,
caudally to erode the sella turcica and laterally to compress or invade the cavernous sinuses.
2 – Craniopharyngiomas (Fig.
5):
Craniopharyngioma is a benign,
often partly cystic sellar/suprasellar mass that arise from remnants of Rathke's pouch along the path of the craniopharyngeal canal.
They are predominantly solid,
spherical and may occur in either the intrasellar or suprasellar regions,
affecting children at 5-10 years and adults at 50-70 years old.
The symptoms can be visual disturbances,
endocrine abnormalities,
motor deficits and increased intracranial pressure.
The main histologic subtypes are adamantinomatous and squamous papillary.
Adamantinomatous are more often encountered in the suprasellar region in children and the squamous papillary presents more frequently in adults.
Calcification is seen in 80% of lesions and is best delineated on CT.
Cystic areas are observed in 85% of cases and can have a variable appearance on MRI depending on the degree of methemoglobin and/or high protein.
Usually present as hyperintense on T2/FLAIR with nodular or rim enhancement.
On magnetic resonance spectroscopy it can present lipid-lactate peak.
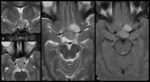
3 – Meningiomas (Fig.
6):
Meningiomas in suprasellar cistern originate from the tuberculum sella,
anterior clinoid processes,
diaphragm sellar,
planum sphenoidale or upper clivus.
They can cause osseous changes including hyperostosis and erosion.
In MRI they are isointense to slightly hypointense on T1WI and isointense to slightly hyperintense on T2WI,
the enhancement is homogenous and intense.
The vascular supply to these lesions usually derived from the carotid,
meningeal and ophthalmic arteries.
4 - Pituitary apoplexy (Fig.
7):
It is a well-described acute clinical syndrome with ophthalmoplegia,
headache and visual loss due to pituitary infarction/hemorrhage.
Profound pituitary insufficiency may develop and present as a life-threatening situation.
Pituitary apoplexy may occur in the setting of massive hemorrhage or tumor necrosis.
Acute hemorrhage will appear hypointense on T2WI and hyperintense on T1WI as the hemorrhagic products evolve. There is usually no hemosiderin deposition associated with pituitary hemorrhage.
5 - Ectopic posterior pituitary (Fig.
8):
An ectopic posterior pituitary occurs as a disruption of normal embryogenesis of the posterior pituitary and is one of the most common causes of pituitary dwarfsm.
This condition can also be caused by trauma or neoplastic processes,
which disrupt the transport of hormones from the hypothalamus to the neurohypophysis.
Congential ectopic neurohypophysis is associated with other midline abnormalties such as septo-optic dysplasia.
This can lead to growth hormone deficiency or even the stalk interruption syndrome (absence or hypoplastic infundibular stalk and adenohypophysis).
MRI is the only modality adequately able to identify ectopic posterior pituitary and it is best seen on sagittal midline T1WI.
Usual features consist of high signal tissue nodule at the median eminence (floor of the third ventricle).
The expected posterior pituitary bright spot is frequently located in the suprasellar region.
6 - Lymphocytic hypophysitis (Fig.
9):
Hypophysitis represent an inflammation of the pituitary gland that compromises an complex group of disorders with two major histologic forms: lymphocytic hypophysitis (LH) and nonlymphoocytic hypophisitis.
LH is an autoimmune disorder seen primarily in peripartum/postpartum females,
but has also been reported in males and postmenopausal women and associated with other autoimmune disorders in approximately 25%. On MRI,
there is intense enhancement of a pituitary mass extending along the infundibulum to the floor of the hypothalamus.
The posterior pituitary bright spot may be absent,
showing that both adenohypophysis or the neurohypohysis can be affected. The sellar flor is intact,
not expanded or eroded.
Dynamic MRI studies have shown that blood supply to the neurohypophysis is often compromised.
Patients may present with visual field impairment and headache due to mass effect on adjacent structures.
As the pituitary parenchyma is destroyed by the inflammatory process,
partial or pan-hypopituitarism develops. However,
the condition is responsive to corticosteroid treatment and can spontaneously resolve.
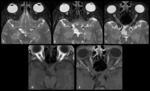
7 – Glioma (Fig.
10-12):
Optic pathway gliomas are relatively uncommon tumors,
usually seen in the setting of neurofibromatosis type I (NF1).
Histologically,
the majority are pilocytic astrocytomas.
They are characterized by imaging by an enlarged optic nerve seen either on CT or MRI,
showing low T1WI and a high central T2WI signal on MRI,
with variable enhancement.
They typically present in children,
accounting for 10-15% of supratentorial tumors in this age group,
often in the setting of NF1,
being low-grade and indolent tumors.
This injury is very rare in adults,
but when occurs,
they are aggressive tumors with no association to NF1.
Clinical presentation varied depending on the extent and location of the tumor,
varying from decreased vision,
proptosis,
polyuria/polydipsia,
obesity,
sexual precocity and endocrine dysfunction.
In large intracranial tumors symptoms of raised intracranial pressure,
focal neurological deficits and hydrocephalus from distortion of the midbrain may also be encountered.
 Abbreviations:
Abbreviations:
T1WI: T1 weighted imaging
T2WI: T2 weighted imaging
FLAIR: Fluid Attenuation Inversion Recovery