Results
Interim analysis of 258 breast lesions from the period November 2017 - June 2018 is performed.
A total of 199 benign and 59 malignant lesions were analysed,
with the result of lesion types listed in Fig.2.
The age of the group with benign lesions (mean = 43.48 CI 95%41.9-45.0) is significant lower than the group with malignancy (mean = 52.5 CI 95% 49.7 - 55.4) (see Fig.3).
The Emean,
Emax and ESD and the lesion-to-fat ratio (elasticity ratio) of the malignant group were significantly higher than benign group,
while there is no significant difference between the ROI size and the depth of the lesion (see Fig.3).
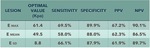
The sensitivity,
specificity and AUC of ROC were 50%,
88% and 0.77 for Emean(cutoff at 49.50kPa) ,
69.5%,
89.9% and 0.82 for Emax (cutoff at 61.4kPa) and 66.1%,
87.9% and 0.83 for ESD (cutoff at 8.8kPa) respectively.
Discussion
There are a number of studies have shown the qualitative findings and quantitative parameter from SWE are useful in differentiating benign and malignant breast lesions [5-10,
12-13].
The utilization of shear wave elastography to improve specificity has beeen well proven.
The earlier studies mainly focus on absolute stiffness of the lesion,
the Emean and Emax. Berg WA et al.
suggested that adding the quantitative assessment with maximum elasticity (Emax) of 80kPa in their study can improve specificity of breast US assessment without loss of sensitivity [6].
Au FW et al.
found that elasticity ratio (i.e.,
the ratio between the mean elasticity of the mass and the mean elasticity of the adjacent adipose tissue) is the most discriminatory factor when compared to Emean and Emax [7]. Our results echoed the usefulness of these parameters.
Recent studies have explored on the assessment of heterogeneity with elastography which may serve as additional parameter to further improve the performance of SWE.
Blank MAB et al.
suggested to use the "stiffness gradient" calculated from the elasticity parameter to improve the differentiation of benign and malignant lesions [8].
We have adopted the ESD as a parameter to assess heterogeneity as described by Gweon et al.
[14],
which is a more handy measurement simultaneously available during acquisition of the elastography image.
It can be used in adjunct to the assessment of Emax or Emean to further improve the diagnostic accurary.
Though similar results are obtained in our study,
our data appears less impressive compared to Gweon et al.
results.
This may be attributed to the fact that the placement of ROI of different operators are not unified and not the whole lesion is included in assessment to reflect the heterogeneity. Nonetheless,
with the cutoff values obtained in our study,
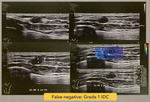
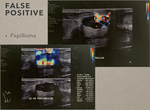
false positive and false negative cases do occur (see Fig 8 and 9).
There are several limitations in our study.
Firstly,
not all operative final patholofical diagnosis are available at time of analysis and some of the pathological diagnosis is based on the core biopsy results.
Besides,
there is also lack of comparison of different measuring methods,
including the the placement of ROI at different position in same lesion as only one view and one measurement (fat reference and lesion only) obtained.
Limited comparison on the same lesion with findings only based on conventional ultrasound findings versus additional benefit with elasticity parameters were made.
The assessment of the quality of the images,
including the presence of artifacts,
are not addressed in this study.
Lastly,
the follow-up period of the study is also not long enough (6-14 months only).